Background: Localised drivers in the form of intermittent focal and rotational activations have been proposed as mechanisms sustaining persistent AF. The possibility of a relationship between these phenomena has not been explored and any interaction with structural remodelling remains unclear.
Methods: Patient undergoing catheter ablation for persistent AF were included. Patients underwent pulmonary vein isolation (PVI) with further ablation being limited to focal and rotational drivers identified on CARTOFINDER activation maps. Potential focal drivers were defined as ≥2 consecutive focal activations with radial spread and rotational drivers were defined as ≥1.5 rotations of 360 degrees A study-defined ablation response included i) AF termination to sinus rhythm or atrial tachycardia (AT) and ii) CL slowing ≥30 ms. Study aim was to assess the relationship of drivers to underlying structural remodelling (i.e. low voltage zones (LVZs) <0.5 mV) and to determine whether there was a temporal (≤500 ms) and spatial (≤12 mm) relationship between focal and rotational drivers.
Results: Forty-one patients were included with a mean AF duration of 12.6 ± 5.8 months. In these patients, 111 CARTOFINDER dynamic activation maps were created post-PVI on which 93 potential drivers were prospectively identified and targeted with ablation (2.3 ± 0.9 per patient). An ablation response was achieved with 86 (92.5%) drivers (57 focal and 29 rotational; 58 (67.4%) CL slowing ≥30 ms and 28 (32.6%) AF termination). Rotational drivers showed a predilection to LVZs (21/29, 72.4%) whilst focal driver did not and occurred in LVZs no more often than would be expected by chance (11/57, 19.3%; p<0.001). The proportion of the left atrium (LA) occupied by LVZs was predictive of identifying rotational drivers (AUC 0.96, 95% CI 0.90–1.00; p<0.001). In patients where the LA was made up of ≤15% of LVZs, only focal drivers were identified. Rotational drivers were mapped to nLVZs however, all of these were either associated with no ablation response (n=2) or CL slowing of ≥30 ms (n=8) and none lead to AF termination on ablation.
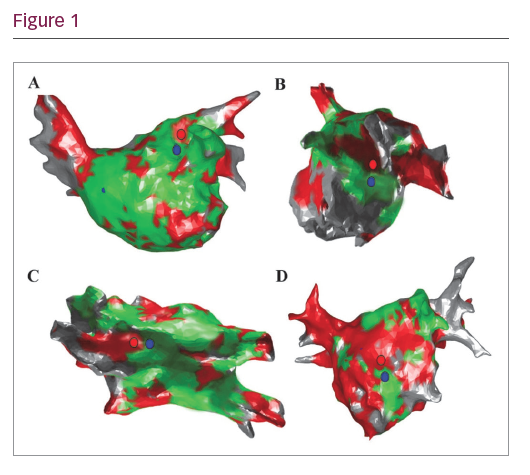
Eighteen out of 21 (85.7%) rotational drivers mapped to LVZs showed temporal and spatial relationship to a focal driver of which all were mapped to nLVZ. Figure 1 demonstrates rotational (blue circle) and focal (red circle) driver sites occurring in close vicinity to each other whereby the rotational driver is mapped to an LVZ and the focal driver to the border of the scar. Focal and rotational driver mapped to the LAA)
roof/LAA, B) lateral wall, C) roof and D) mid anterior wall.
When considering all 57 confirmed focal drivers, the presence of an LVZ within 12 mm was a strong predictor for whether a paired rotational driver would also occur in that vicinity with a sensitivity of 100% (95% CI 81.5–100.0%) and specificity of 71.8% (95% CI 55.1–85.0%). Rotational drivers were more likely to terminate AF with ablation when they were paired to a focal driver (odds ratio of 11.7; 95% CI 1.8–74.2; p=0.009).
Conclusions: Although rotational drivers are mostly dependent on structural remodelling, focal driver are not. Rotational drivers mapped to LVZs usually demonstrate spatial and temporal relationship to focal drivers. The ablation response suggests that rotational activity is more important when it occurs in LVZs and in particular, when it is paired with a focal activation. These novel mechanistic observations outline a plausible model for patient specific mechanisms maintaining AF.