Introduction: Patients with structural heart disease (SHD) are susceptible to ventricular tachycardia (VT) and arrhythmic death. Use of anti-arrhythmic drugs is often confounded by unacceptable side effects or suboptimal effectiveness. Catheter ablation (CA) is a viable option in these patients. This study aims to: 1) determine long-term outcome of patients with SHD undergoing CA for VT; and 2) identify potential predictors of favourable ablation outcome and improved survival.
Method: This single-centre longitudinal study enrolled patients with ischaemic (ICM) and non-ischaemic cardiomyopathies (NICM) undergoing CA for VT. Follow-up data on 5-year survival and ICD shocks for VT were collected. Potential demographic, clinical and procedural predictors of VT-free survival were assessed. Cox regression and Kaplan–Meier analyses were performed.
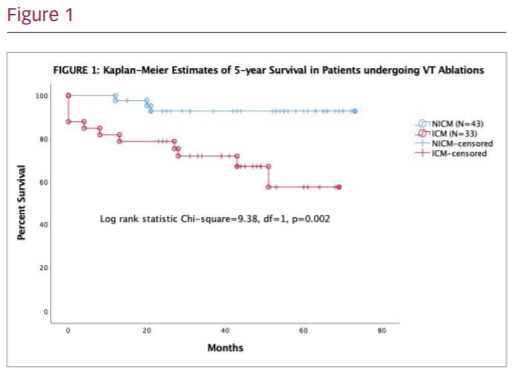
Results: Seventy-six patients (ICM 43%, NICM 57%; male 79%) were included. Electrical storm is more prevalent in the ICM group (ICM 50% vs. NICM 14%). At ablation, unstable clinical VT were more prevalent in ICM group (52% vs. 32%, p<0.05) despite similar VT inducibility. In these patients, only substrate-based ablation was performed. Ablation endpoint was determined by VT non-inducibility (ICM 70% vs. NICM 76%, p=ns). Acute complication rate was 18.4% including vascular complications (5.3%), cardiac tamponade (1.3%), stroke (1.3%), MI (1.3%), cardiogenic shock (2.6%) and death (1.3%). In both groups, there were significant reduction in ICD shocks after CA. However, NICM group demonstrated superior long-term VT-free survival (Figure 1). Independent predictors of mortality include age >60 years, LVEF <35%, electrical storm, declined eGFR and substrate-based ablation strategy. VT non-inducibility as ablation endpoint independently predicts freedom from ICD shocks.
Conclusion: VT ablation significantly reduces ICD shocks for VT but mortality remains high in some patients. VT non-inducibility as ablation endpoint partially prognosticates VT recurrence. Future studies are warranted to refine patient profiling, thereby further optimising long-term VT ablation outcomes.