Introduction: The DiamondTemp ablation (DTA) catheter system delivers high-power, open-irrigated, temperature-controlled radiofrequency (RF) ablation. This study assesses the feasibility of this new technology for VT ablation in patients with ICM.
Method: 10 patients (mean age 73.4 years [64–84 years]) with a diagnosis of ICM were recruited over 3 months. 4 patients were classified as high risk and 6 as intermediate risk using the PAINESD score. All patients were on optimal anti-arrhythmic drug therapy: B-blocker (n=10), amiodarone (n=7), mexiletine (n=3). The Ensite Precision Cardiac Mapping System was used to construct substrate maps with the Advisor HD Grid mapping catheter with an average point density of 2,344/26,165 (points used/points collected). Ablation lesions were delivered as per standard protocol: Temperature set to 60°C for an empirical lesion duration of 60 s, or shorter if i) failure to achieve a temperature of 45°C, ii) impedance drop of 15 Ω reached or iii) rising impedance. Metrics recorded during the ablation included time, power, impedance, and temperature, were collected at a rate of 1 Hz. Mapping was performed as per the UHCW VT mapping and ablation workflow with analysis of pre- and post-ablation bipolar and unipolar total scar area (TSA), border-zone area (BZA), dense scar area (DSA), late potential area (LPA), mean bipolar and unipolar voltages of ablation target areas (ATA). Standard VT induction protocols was performed at the end of each procedure.
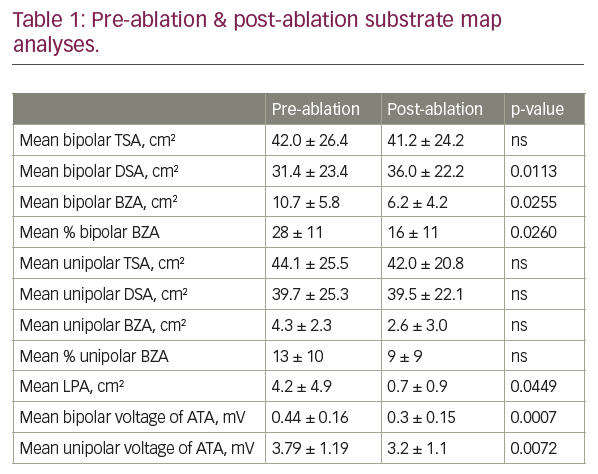
Results: Average number of lesions per case was 51.8 ± 17.7, average time per lesion was 44.5 ± 11.1 s, average power per case was 47.8 ± 1.2 W, average temperature per case was 49.8 ± 2 °C, average maximum temperature per lesion was 55.2 ± 2 °C at an average duration of 25.8 ± 8 s and the average impedance drop per lesion was 11.2 ± 2.4 Ω at an average duration of 23.0 ± 7 s. Map data analysis is displayed in Table 1. There was a significant reduction in the average BZA of 4.4 cm2 or 12% (p=0.026) and LPA of 3.5 cm2 (p=0.0449). There was a significant reduction in the mean bipolar voltage of ATA, 0.14 mV (p=0.0007) and mean unipolar voltage of ATA, 0.59 mV (p=0.0072). There was no inducible clinical or non-clinical VT at the end of 9 procedures, with no stimulation performed at the end of 1 case due to pericardial tamponade requiring drainage.
Conclusion and implications: The DTA catheter system resulted in a significant reduction of both mean bipolar and unipolar voltages of the ATA. The average bipolar BZAs and LPAs were significantly reduced with no inducible clinical or non-clinical VT at the end of the tested procedures. This is the first study to report the efficacy and safety of the DTA catheter system in VT ablation, which positively impacts on key substrate ablation targets with consistent on-table endpoint testing outcomes. Further studies investigating both long-term clinical outcomes and performance to comparable ablation technology is required.







