Introduction: Guidelines recommend providing primary care practitioners direct access to echocardiography (echo), prior to specialist cardiology input, in patients whom they suspect have heart failure, based on symptoms and raised N-Terminal pro Brain Natriuretic Peptide (NTproBNP). Early access can lead to increased detection of Heart Failure with a reduced Ejection Fraction (HFrEF). However, it is noted that Atrial Fibrillation (AF) may contribute to falsely raised NTproBNP levels, and this is thought to reduce the diagnostic yield of HFrEF. As a result, some services exclude patients with AF from their direct access pathways. We sought to determine the true burden of AF on the diagnostic yield within our local health economy, to evaluate whether existing Open Access Echocardiography (OAE) pathways should be modified in this group of patients to improve cost-effectiveness.
Methods: The study cohort included all consecutive patients who received an echo via the OAE pathway between January 2017 and September 2019. The cohort was grouped based on NTproBNP levels, pre-referral, into group A (400-2000 ng/L) and B (>2000 ng/L). The diagnostic yield in patients with and without AF in both groups were calculated as the percentage of patients with a positive diagnosis of HFrEF compared to those with a normal ejection fraction (nEF). These were compared using independent sample t-tests for nominal variables and chi-square tests for dichotomous and categorical variables.
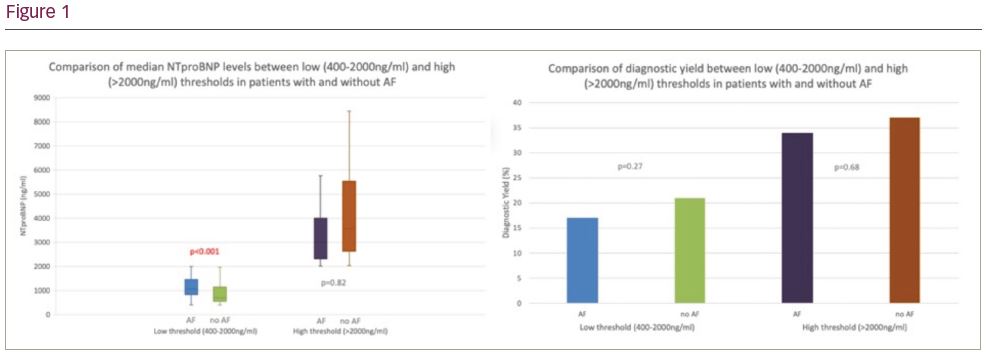
Results: Over 32 months, 487 patients met our OAE criteria and received an echo. 164 patients were ≤75 years old and 323 were >75 years old. Median age was 77 years (IQR 72-84) and 48.8% were male. Overall diagnostic yield for HFrEF was 20.4% vs 35.7% in GpA vs GpB patients (p<0.001). In GpA, there were 140 patients with AF and 196 without AF. The median NTproBNP in the two subgroups were 1043 ng/mL (IQR 845-1443) vs 701 ng/mL (IQR 548-1137) (p<0.001), and diagnostic yield was 17% and 21% respectively (p=0.27). In GpB, there were 90 patients with AF and 61 without AF. The median NTproBNP in the two subgroups was 3019 ng/mL (IQR 2323-3986) vs 3567 ng/mL (IQR 2636-5298) (p=0.821), with diagnostic yield returning at 34% vs 37.7% respectively (p=0.68).
Conclusion: Our results demonstrate that very high NTproBNP levels were associated with a significantly higher diagnostic yield for HFrEF with a 15% improvement at the higher threshold. AF was associated with significantly higher NTproBNP levels in patients at the lower threshold but not at the higher threshold, however this did not translate into a clinically meaningful difference in the overall diagnostic yield of HFrEF. Based on our results, raising NTproBNP thresholds for AF patients or excluding them from screening pathways is not recommended. Alternative measures, such as the use of novel biomarkers, may improve the diagnostic yield of HFrEF in patients with modestly elevated NTproBNP.