Background: Palpitations are a common reason for GP appointments in primary care and a frequent reason for cardiology referral. In Wakefield, this translated to approximately 24,000 primary care and out-of-hours consultations in 2021.
Purpose: The purpose of this pilot was to evaluate a pathway for palpitations diagnosis and management in primary care. The proposed pathway was designed to avoid unnecessary referrals to secondary care, to shorten the waiting time to diagnosis for patients and to cut down
visits to A&E and out-of-hours service in primary care.
Method: The pathway piloted at Health Care First, which is a federation for 30,000 patients, was based on a community cardiology approach, where a GP with special interest in cardiology could offer the service for the wider community. The pathway began with an initial clinical evaluation comprising medical history, physical examination and a standard 12-lead electrocardiogram (ECG). After ruling out of any red flags and otherwise deemed appropriate to continue to be assessed with the proposed diagnostic method, the patients were provided with
a handheld ECG device for intermittent 30-second ECG registration at home. During a 4-week investigation period, the patients would record their ECG when experiencing symptoms. The primary care team remotely monitored the traces, which were received on a cloud-based system with artificial intelligence capabilities, and if pathology was recorded, patient was contacted and informed of the management plan. If after 4 weeks no pathology was found, patients received a discharge consultation for reassurance and the final report was generated.
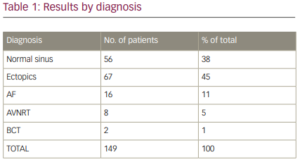
Results: During the 18-month pilot, we screened a total of 149 patients. Out of the patients screened, 16 (11%) were diagnosed with atrial fibrillation (AF) and 67 (45%) were diagnosed with benign ectopics as the cause of their palpitations. Two rare occurrences of life threatening
broad complex tachycardias were also detected, both of which ended up needing defib implantation. Table 1 further presents the results by
diagnosis for rest of the patients.
Conclusions: The results from the pilot indicated a reduction in GP/out-of-hours consultations by 50% and over 90% reduction in referral to secondary care for Holter monitoring by implementing an easy-to-use handheld ECG as part of the community-led palpitation pathway. The results further implied that a district-wide implementation could lead to at least 120 new AF diagnoses in Wakefield district per year, having a knock-on benefit of stroke reduction and cost economic impact in the society by reducing anxiety, lost employment hours and increasing productivity. Another key outcome seen is the reassurance value of conducting symptomatic palpitation monitoring to reassure patients, the majority of whom had either normal sinus rhythm or benign ventricular ectopics and had failed to be satisfied with conventional Holter monitoring in the past.