Coronary artery disease (CAD) is encountered on a daily basis in the field of medicine. Between 2009 and 2012, the global prevalence of CAD was 154 million, based on data from the Global Burden of Disease study; for the same period in the USA, it was approximately 15.5 million, based on data collected by the American Heart Association (AHA).1,2 Dual antiplatelet therapy (DAPT), composed of acetylsalicylic acid (ASA [aspirin]) and a P2Y12 inhibitor, has been recommended for patients who have clinical acute coronary syndrome (ACS) with or without percutaneous coronary intervention (PCI), or in patients who are considered to have high cardiovascular (CV) risk.3 When choosing DAPT for patients, many different factors are taken into consideration, such as the optimal P2Y12 inhibitor to combine with ASA, length of therapy, perceived benefit for the patient and potential for bleeding complications, particularly if the patient has had bleeding diathesis in the past. The data for starting and potentially continuing DAPT beyond current guidelines are constantly evolving. More studies continue to be published to fill gaps in the current knowledge or to re-evaluate existing data on this topic. The purpose of this article is to review the available data regarding the use of DAPT in patients with high CV risk.
A narrative literature review and a hand search of the reference lists of included articles and relevant reviews were performed. Studies were identified by searching PubMed, Google Scholar and Embase for English-language articles from 1985 through December 2020 by using the medical subject heading terms and keywords ‘antiplatelet therapy’ and ‘high-risk cardiovascular disease’, alone or in combination. Both authors critically reviewed the design, population characteristics and results of the selected studies.
Dual antiplatelet therapy after stroke or transient ischaemic attack
Similar to CAD, there is a high burden of stroke in the USA. Patients with a history of stroke or transient ischaemic attack (TIA) have an increased risk of further CV disease (CVD).4 In a study by Wang et al., 1,106 patients with prior ischaemic stroke were compared to 9,194 patients with no record of prior ischaemic stroke who were undergoing PCI.4 The primary outcome was major adverse CV and cerebrovascular events, recurrent stroke and stent thrombosis (ST) after a median follow-up period of 29 months. Patients with prior ischaemic stroke had a higher incidence of the primary endpoint (adjusted hazard ratio [HR] 1.294; 95% confidence interval [CI] 1.100–1.522; p=0.002), recurrent stroke (adjusted HR 2.463; 95% CI 1.729–3.507; p=0.000) and stent thrombosis (adjusted HR 1.787; 95% CI 1.075–2.971; p=0.025).4
One of the earliest studies to evaluate the role of DAPT in patients with prior history of stroke or TIA was the ESPS-2 (European Stroke Prevention Study-2), published in 1996, where 6,602 patients with prior history of stroke or TIA were randomized into one of four treatment options that consisted of ASA alone, dipyridamole alone, ASA and dipyridamole or placebo, and were followed for 2 years.5 At the end of the study period, compared with placebo, the combination of ASA and dipyridamole reduced stroke risk by 37.0% (p<0.001), 18.1% with ASA alone (p=0.013), and 16.3% with dipyridamole alone (p=0.039). There was no significant difference in death among the groups (p=0.616). However, there was a significantly increased incidence of moderate or severe/fatal bleeding in the treatment groups, with 8.2% in the ASA-only group, 8.7% in the ASA and dipyridamole group, 4.7% in the dipyridamole group and 4.5% in the placebo group. Therefore, the results of the ESPS-2 study suggest that a treatment strategy of DAPT consisting of ASA and dipyridamole was more effective at preventing recurrent stroke than a treatment strategy consisting of either medication alone.5
Another pivotal trial that evaluated the role of a DAPT strategy was the ESPRIT (European/Australian Stroke Prevention in Reversible Ischaemia) trial (ClinicalTrials.gov Identifier: NCT00161070).6,7 In this study, 2,739 patients with a history of ischaemic stroke or TIA were randomized to ASA alone or ASA with dipyridamole; the primary endpoint of composite of death from vascular causes, non-fatal stroke, myocardial infarction (MI) or major bleeding were evaluated. DAPT using ASA and dipyridamole had an incidence of the primary composite endpoint in 13% versus 16% in those patients receiving ASA only (absolute risk reduction 1.0%; 95% CI 0.1–1.8%). However, there was a higher rate of discontinuation of DAPT treatment compared with ASA alone (34% versus 13%) due to adverse events, with headache cited as the main reason for discontinuation of treatment.6
One of the latest trials to evaluate DAPT therapy in patients with prior ischaemic stroke was published in 2018.8 In this study, 3,572 patients with a history of ischaemic stroke were randomized to a treatment strategy composed of ASA only, ASA plus dipyridamole and clopidogrel. The primary endpoint of all-cause mortality and a combined endpoint of all-cause mortality and major adverse cardiac events, stroke or MI, were compared. ASA plus dipyridamole showed a lower risk of mortality at 0–90 days (HR 0.62; 95% CI 0.43–0.91) and clopidogrel was associated with a lower risk of mortality at 1–3 years (HR 0.39; 95% CI 0.26–0.60).8 Support for DAPT after ischaemic stroke comes from CHANCE (Clopidogrel in High-risk Patients With Acute Non-disabling Cerebrovascular Event; NCT00979589), in which patients with high-risk TIA and low National Institutes of Health Stroke Scale (NIHSS) stroke were treated with clopidogrel load in the first 24 hours, followed by DAPT for 21 days, versus aspirin alone.9,10 At 90 days, the stroke rate in the DAPT arm was 8.2%, compared with 11.7% with aspirin monotherapy.
The POINT (Platelet-oriented inhibition in new TIA and minor ischaemic stroke) trial (ClinicalTrials.gov Identifier: NCT00991029) confirmed the utility of short-term DAPT use and reported that DAPT reduced a composite of stroke, MI or vascular death at 90 days, but patients suffered increased major haemorrhage.11,12 Secondary analysis showed DAPT benefit at 7- and 30-days post stroke. Beyond 30 days, haemorrhagic complications outweighed benefit.12 A recent meta-analysis of 16 randomized controlled trials with a total of 29,032 patients reported that, among patients who present with ischaemic stroke/TIA, short-course clopidogrel plus aspirin for 21 days immediately following the index event appears to be more effective than, and as safe as, monotherapy for secondary stroke prevention.13 The AHA/American Stroke Association guidelines recommend that in patients presenting with minor non-cardioembolic ischaemic stroke (NIHSS ≥3) who have not received intravenous tissue plasminogen activator, treatment with DAPT (aspirin and clopidogrel) started within 24 hours after symptom onset and continued for 21 days is effective in reducing recurrent ischaemic stroke for a period of up to 90 days from symptom onset.14
Dual antiplatelet therapy after acute coronary syndrome (ST elevation myocardial infarction/non-ST elevation myocardial infarction)
The ischaemic benefit of DAPT has been not only demonstrated in patients with prior stroke, but also in the setting of ACS. One of the landmark studies to evaluate the role of DAPT therapy in ACS was the CURE trial (Clopidogrel in Unstable Angina to Prevent Recurrent Events).15 In this trial, 12,562 patients who presented within 24 hours of symptom onset of ACS were randomized to receive clopidogrel or placebo in addition to ASA for 3–12 months. The primary outcome of composite of death from CV causes, non-fatal MI, and stroke was seen in 9.3% of patients receiving clopidogrel, compared with 11.4% in patients who received placebo (relative risk [RR] 0.80; 95% CI 0.78–0.90; p<0.001). The use of clopidogrel with ASA was also shown to reduce the incidence of in-hospital refractory or severe ischaemia, heart failure and revascularization procedures. However, there was a greater incidence of major bleeding observed in patients that received clopidogrel compared with placebo (3.7% versus 2.7%; RR 1.38; p=0.001), but there was no difference noted in the incidence of life-threatening bleeding or haemorrhagic stroke between the two groups (2.1% versus 1.8%; p=0.13).15
In patients with non-ST elevation MI (NSTEMI) who underwent PCI, the use of DAPT therapy with ASA and clopidogrel was evaluated in the PCI-CURE study.16 In the original CURE study, 2,658 patients who underwent PCI were randomized to receive clopidogrel or placebo in addition to ASA before PCI; treatment was continued for a mean period of 8 months.15 The primary endpoint of CV death, MI or any revascularization was observed in 4.5% of the patients in the clopidogrel and 6.4% in the placebo group (RR 0.70; 95% CI 0.50–0.97; p=0.03). Furthermore, the PCI-CURE study also demonstrated that the protective effect of DAPT was seen throughout the 8-month study period, with an overall reduction in CV death or MI of 31%. Despite a statistically significant increased incidence of major bleeding events in patients treated with clopidogrel in the CURE trial, the PCI-CURE trial did not show a statistically significant difference in the incidence of major bleeding from PCI to 30 days (p=0.69) or from PCI to follow-up (p=0.64) between the two treatment groups.16
The clinical and mortality benefits of DAPT have been demonstrated in patients with NSTEMI in the previously mentioned trials. However, DAPT therapy has been evaluated in patients with ST elevation MI (STEMI) in three landmark trials. The first of these trials is the CLARITYTIMI 28 (Clopidogrel as Adjunctive Reperfusion Therapy – Thrombolysis in Myocardial Infarction) trial (ClinicalTrials.gov Identifier: NCT00714961) where 3,491 patients were randomized to receive – along with ASA – either clopidogrel or placebo, a fibrinolytic agent and heparin if appropriate, and scheduled for subsequent angiography 48–192 hours after the start of the study medication.17,18 The primary endpoint was the composite of an occluded infarct-related artery on angiography, or death or recurrent infarction before angiography.18 The primary endpoint was observed in 21.7% of patients receiving placebo and 15.0% in the clopidogrel group, which represents a 36% reduction in the odds ratio (95% CI 24–47%; p<0.001). When the components of the primary endpoint were analysed individually, treatment with clopidogrel reduced the odds ratio of the occluded infarct-related artery by 41% (p<0.001), and the rate of recurrent MI by 30% (p=0.08); no difference was seen in the rate of death from any cause when compared to placebo (2.2% versus 2.6%; p=0.49). At 30 days of treatment, DAPT with clopidogrel showed an odds reduction in the composite endpoint of death from CV causes, recurrent MI or recurrent ischaemia needing urgent revascularization, by 20% (p=0.03). Analysis of the individual endpoints showed an odds reduction of recurrent MI of 31% (p=0.02), an odds reduction of 24% of recurrent myocardial ischaemia needing urgent revascularization (p=0.11) and a 46% odds reduction in stroke (p=0.052). Between the two study groups there was no statistically significant difference in the rate of major bleeding observed at 30 days between the clopidogrel and placebo groups (1.9% versus 1.7%; p=0.80).18
Further evidence for the use of DAPT in patients with STEMI was provided by the pre-specified analysis of the subgroup of 1,863 patients who underwent PCI during the study period of the CLARITY-TIMI 28 trial, known as the PCI-CLARITY trial.19 The primary outcome studied was the incidence of the composite of CV death, recurrent MI or stroke between PCI and 30 days. Treatment with clopidogrel was associated with a significant reduction in the primary endpoint of composite of CV death, recurrent MI or stroke by 46% after PCI (3.6% versus 6.2%; adjusted odds ratio 0.54; 95% CI 0.40–0.95; p=0.03). There was also no difference in the rate of thrombolysis in major or minor bleeding noted between the groups treated with clopidogrel and with placebo (2.0% versus 1.9%; p>0.99).19
The third landmark trial to evaluate the efficacy of DAPT in patients with STEMI was the COMMIT trial (Clopidogrel and Metoprolol in Myocardial Infarction Trial).20 This trial was different from the CLARITY-TIMI 28 and CLARITY-PCI trials in terms of patient selection, as these two trials only studied patients with STEMI. The COMMIT trial evaluated 45,852 patients with suspected acute STEMI, left bundle branch block or ST-segment depression, who were randomized to receive DAPT with ASA and clopidogrel or ASA with placebo. The primary endpoints studied were the composite of death, re-infarction or stroke, as well as death from any cause during the treatment period. At the end of the study period, treatment with clopidogrel reduced the rate of death, re-infarction or stroke by 9% (9.2% versus 10.1%; p=0.002), as well as reducing death from any cause by 7% (7.5% versus 8.1%; p=0.03). Similar to the previous trials, the risk of fatal haemorrhage, haemorrhage needing transfusion or intracranial bleeds was not significantly higher in the patients treated with clopidogrel, patients over the age of 70, or in those for whom fibrinolytic therapy was administered (0.58% for the clopidogrel group versus 0.55% in the placebo group; p=0.59).20
The efficacy of DAPT in patients presenting with ACS has been demonstrated, however; the optimal P2Y12 inhibitor in this setting was evaluated in the PLATO (Platelet Inhibition and Patient Outcomes) trial (ClinicalTrials.gov Identifier: NCT00391872) and the TRITON-TIMI 38 trial (A Comparison of Prasugrel [CS-747] and Clopidogrel in Acute Coronary Syndrome Subjects Who Are to Undergo Percutaneous Coronary Intervention; ClinicalTrials.gov Identifier: NCT00097591).20–24 In the PLATO trial, ticagrelor was compared to clopidogrel in 18,624 patients admitted to the hospital with ACS with or without the presence of ST elevation and with symptom onset within the previous 24 hours. The primary outcome evaluated was the time to first occurrence of composite of death from vascular cause, MI or stroke. The secondary endpoints were composite of death from any cause, MI or stroke; the composite of death from vascular cause, MI, stroke, severe recurrent cardiac ischaemia, recurrent cardiac ischaemia, TIA or other arterial thrombotic events; MI alone; death from CV causes alone; stroke alone; and any cause mortality. At 12 months, the primary endpoint occurred in 9.8% of patients treated with ticagrelor, versus 11.7% in the patients treated with clopidogrel (HR 0.84; 95% CI 0.77–0.92; p<0.001). There was also a significant difference in patients treated with ticagrelor versus clopidogrel for the other composite endpoints: MI alone (5.8% versus 6.9%; p=0.005), death from vascular causes (4.0% versus 5.1%; p=0.001) and all-cause mortality (4.5% versus 5.9%; p<0.001). There was no difference found in the incidence of stroke alone between the two study groups (1.5% versus 1.3%; p=0.22) but, more importantly, also in the rate of major bleeding (11.6% versus 11.2%; p=0.43). However, treatment with ticagrelor was associated with higher rates of major bleeding not related to coronary artery bypass graft (CABG; 4.5% versus 3.8%; p=0.03), as well as fatal intracranial bleeding (0.1% versus 0.01%; p=0.03). There was also a higher incidence of dyspnoea (13.8% versus 7.8%) and ventricular pauses within the first week of treatment in patients treated with ticagrelor. As a result, the PLATO trial demonstrated that in patients with ACS with or without ST elevation, treatment with ticagrelor significantly reduced the rate of death from vascular causes, MI or stroke without increasing the incidence of major bleeding.23
In the TRITON-TIMI 38 trial, 13,608 patients with ACS who were awaiting PCI were randomized to usual care plus either prasugrel or clopidogrel.24 At a mean follow-up of 15 months, the prasugrel group had less CV mortality, non-fatal MI or non-fatal stroke than the clopidogrel group (9.9% versus 12.1%). There was more non-CABG-related thrombolysis in myocardial infarction (TIMI) major bleeding (2.4% versus 1.8%) and CABG-related TIMI major bleeding (13.4% versus 3.2%) in patients receiving prasugrel. There was no difference in either CV or all-cause mortality. A subgroup analysis of STEMI patients reported a greater RR reduction for the same primary endpoint of CV mortality, non-fatal MI or non-fatal stroke (6.5% versus 9.5%; HR 0.68; 95% CI 0.54–0.87; p=0.0017) without an increased risk of bleeding, except for CABG-related TIMI major bleeding.25 In contrast to the positive endpoint of TRITON-TIMI 38, the TRILOGY ACS (A Comparison of Prasugrel and Clopidogrel in Acute Coronary Syndrome Subjects) trial (ClinicalTrials.gov Indentifier: NCT00699998) did not demonstrate a risk reduction of a similar primary endpoint with prasugrel in patients with unstable angina/NSTEMI not scheduled for revascularization.26,27
However, when discussing patients that are considered to have a high bleeding risk, DAPT duration is only one part of the clinical decision-making process, particularly in those patients undergoing PCI with stent placement. In a trial on polymer-based or polymer-free stents in patients at high bleeding risk (Onyx ONE; A Randomized Controlled Trial With Resolute Onyx in One Month Dual Antiplatelet Therapy [DAPT] for High-Bleeding Risk Patients; ClinicalTrials.gov Identifier: NCT03344653), 1,996 patients at high risk of bleeding undergoing PCI were randomized to either the Resolute Onyx™ drug-eluting stent (DES; Medtronic, Fridley, MN, USA) or the BioFreedom™ drug-coated stent (Biosensors Europe SA, Morges, Switzerland).28,29 All patients were given DAPT for 1 month and then continued on single antiplatelet therapy, composed of either ASA or a P2Y12 inhibitor, which was chosen at the discretion of the physician, and followed for a period of 1 year. The primary outcome was a composite of CV death, MI and stent thrombosis, and was seen in 17.1% of the patients who received the Resolute Onyx DES versus 16.9% of those who received the BioFreedom drug-coated stent (non-inferiority p=0.011, superiority p=0.84). There was a high, but not statistically significant, incidence of Bleeding Academic Research Consortium (BARC) 2–5 bleeding between the two groups, (15.1% versus 13.7%; p=0.4), similar stroke rates (2.2% versus 2.3%), but higher rates of target lesion revascularization with the BioFreedom drug-coated stent (2.8% versus 4.0%).28
Further evidence on the use of shorter durations of DAPT in patients considered to be at high risk for bleeding was provided by the LEADERS-FREE trial (A Randomized Clinical Evaluation of the BioFreedom™ Stent; ClinicalTrials.gov Identifier: NCT01623180).30–32 In this study 2,466 patients considered to be at high bleeding risk and undergoing PCI were followed for 390 days after being randomized to receive PCI with a BioFreedom polymer-free umirolimus-coated stent (Biolimus A9™ drug-coated stent; Biosensors Europe SA, Morges, Switzerland) versus Gazelle bare-metal stent (BMS; Biosensors Europe SA, Morges, Switzerland), followed by 1 month of DAPT therapy. The primary endpoint evaluated was a composite of cardiac death, MI or definite or probable stent thrombosis at 390 days. The efficacy endpoint of clinically driven target lesion revascularization was also evaluated in these patients. At the end of the study, the incidence of the primary endpoint was observed in 9.4% of patients in the drug-coated stent group and 12.9% in the BMS group (HR 0.71; 95% CI 0.56–0.91; p<0.001 for non-inferiority and p=0.005 for superiority). The incidence of clinically driven target lesion revascularization was also noted to be statistically lower in patients treated with the drug-coated stent versus those who received the BMS (5.1% versus 9.8%; HR 0.50; 95% CI 0.37–0.69; p=0.001).30 The incidence of minor and major bleeding was not statistically significant between the two treatment groups. Based on the results of this trial, it can be concluded that, for the treatment of patients deemed to have high bleeding risk who need to undergo PCI, placement of a drug-coated stent combined with 1 month of DAPT can be considered a suitable alternative to standard DAPT.
Researchers in the SENIOR trial (Efficacy and Safety of New Generation Drug Eluting Stents Associated With an Ultra Short Duration of Dual Antiplatelet Therapy. Design of the Short Duration of Dual antiplatElet Therapy With SyNergy II Stent in Patients Older Than 75 Years Undergoing Percutaneous Coronary Revascularization; ClinicalTrials.gov Identifier: NCT02099617) sought to compare a shorter duration of DAPT in elderly patients aged >75 years receiving a DES or BMS.31,33 In this study, 1,200 patients aged >75 years with stable angina, silent ischaemia or ACS that were candidates for PCI were randomized to receive either DES or BMS and followed for 1 year. The duration of DAPT was determined by the patient’s presentation prior to randomization, where those with a stable presentation were given 1 month of DAPT, whereas those with an unstable presentation were given 6 months of DAPT therapy. The primary endpoint was a composite of all-cause mortality, MI, ischaemia-driven target lesion revascularization or stroke. The primary endpoint was observed in 12% of the patients in the DES arm versus 16% in the BMS arm (RR 0.71; 95% CI 0.52–0.94; p=0.02). The incidence of bleeding complications was observed to be similar between the two treatment groups, and occurred in 26 patients versus 29 patients (RR 0.90; 95% CI 0.51–1.54; p=0.68). The rate of stent thrombosis was found to be slightly higher in the BMS group, but was not statistically significant (three versus eight patients; RR 0.38; 95% CI 0.00–1.48; p=0.13).31 As a result, it can be inferred from this study that in elderly patients with high bleeding risk, a shorter duration of DAPT with a BMS can be a suitable alternative to standard DAPT of 1 year without significantly increasing the risk of major adverse cardiac events, while at the same time decreasing the incidence of potential bleeding.
The EVOLVE Short DAPT study (ClinicalTrials.gov Identifier: NCT02605447) also evaluated a shorter duration of DAPT in patients considered to be at high risk of bleeding, requiring PCI.34,35 In this prospective, single-arm study, 2,009 patients aged ≥75 years that had considerable risk of major bleeding with prolonged DAPT and were candidates for PCI, were treated with the SYNERGY™ everolimus-eluting platinum chromium coronary stent (Boston Scientific, Marlborough, MA, USA), and subsequently treated with 3 months of ASA in combination with a P2Y12 inhibitor. At the end of the 3 months, the P2Y12 inhibitor was discontinued, and the patients were continued on ASA for another 15 months. The primary endpoint was the incidence of death or MI, with the secondary endpoint of adjusted BARC 2–5 bleeding between 3 and 15 months. When compared with a historical control of patients that received standard duration of DAPT, placement of a Synergy DES and subsequent DAPT for 3 months showed a similar incidence of death and MI (5.6% versus 5.7%). The study also aimed to show superiority in the incidents of BARC 2–5 bleeding with 3-month DAPT; however, the study failed to meet that respective endpoint.34
In a similar study, the XIENCE 90 trial (XIENCE 90: A Safety Evaluation of 3-month DAPT After XIENCE Implantation for HBR Patients; ClinicalTrials.gov Identifier: NCT03218787), investigated 2,047 patients aged >75 years that were considered to be at high risk for bleeding. In the prospective, single-arm non-randomized trial, patients received 3 months of DAPT after placement of a XIENCE stent (XIENCE Xpedition Everolimus Eluting Coronary Stent System [EECSS], XIENCE Alpine EECSS, XIENCE PRO^X EECSS [rebrand of the XIENCE Xpedition Stent System only available outside of the USA], XIENCE PRO^A EECSS [rebrand of the XIENCE Alpine Stent System and only available outside of the USA] and XIENCE Sierra EECSS of coronary DES; Abbott Laboratories, Abbott Park, IL, USA).36,37 The primary endpoint was all-cause death or MI, plus secondary endpoints of BARC 2–5 bleeding and definite or probable stent thrombosis, which was also considered the performance goal. Patients in the study were treated with DAPT for 3 months, which consisted of ASA and a P2Y12 inhibitor, and if taking an oral anticoagulant at the time of stent placement, treatment with the oral anticoagulant and a P2Y12 could be considered for the 3 months. After this time, the P2Y12 inhibitor was discontinued. When compared to the historical control group from the XIENCE V USA study (XIENCE V® Everolimus Eluting Coronary Stent System USA Post-Approval Study [XIENCE V® USA-Phase 1] [XVU-Phase 1]; ClinicalTrials.gov Identifier: NCT00676520) that received DAPT for 12 months, there was no significant difference observed in the primary endpoint of all-cause death or MI (5.4% versus 5.4%; p=0.0005 for non-inferiority).38,39 The incidence of BARC 2–5 bleeding between the treatment group and historical control group observed at the end of the study period was found to be similar (5.1% versus 7.0%; p=0.06687 for superiority). However, when major bleeding (BARC 3–5) was considered, the incidence was found to be lower and statistically significant between both groups (2.2% versus 6.3%; p<0.0001 for superiority). The incidence of definite or probable stent thrombosis was also found to be lower at 0.20% (p<0.0001), which met the performance goal for the XIENCE stent.36 Thus patients considered to be at high bleeding risk that need PCI may be considered for 3-month DAPT after placement of a XIENCE DES, with comparable rates of ischaemic events compared to standard 12-month DAPT and a lower incidence of major bleeding.
The data discussed thus far show that DAPT with clopidogrel and ASA has a significant mortality benefit and a protective effect against ischaemic complications in patients with ACS, regardless of the presence of ST elevation, without increasing the incidence of major or fatal bleeding. As a result, it is presently recommended that all patients with suspected ACS be treated with DAPT consisting of ASA and a P2Y12 inhibitor, regardless of whether reperfusion is undertaken or not.3
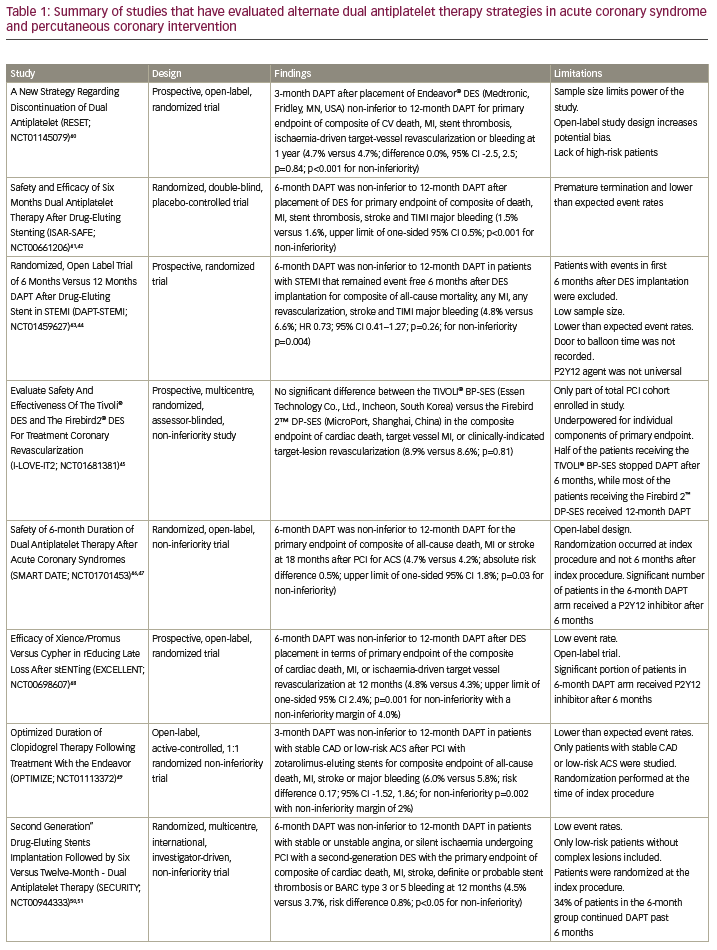
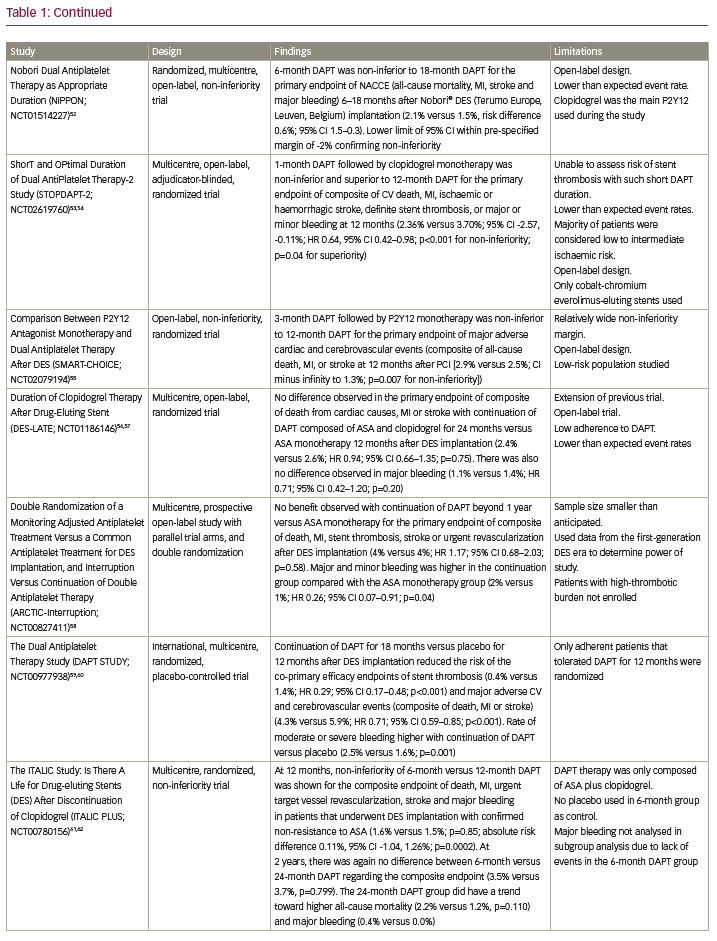
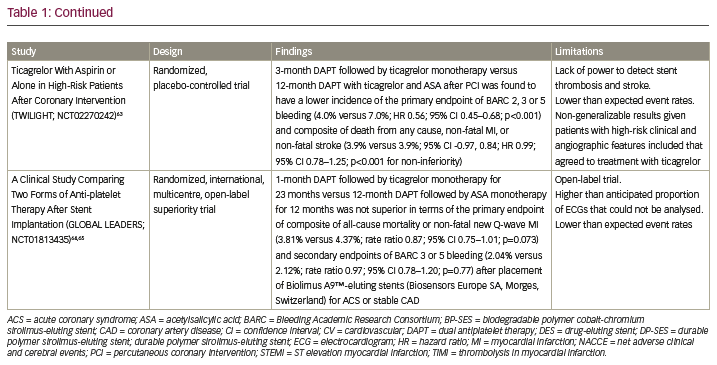
Currently, data regarding the topic of optimal DAPT duration are extensive, with multiple studies showing a potential benefit of shorter DAPT duration than that currently recommended in the American College of Cardiology (ACC)/AHA guidelines. Table 1 includes a summary of multiple studies that have evaluated alternate DAPT strategies in certain clinical scenarios.40–65 Although extensive, the list of studies included is not by any means comprehensive, but shows the heterogeneity of the data that are currently available.
Dual antiplatelet therapy in primary prevention
The data demonstrating the clinical benefit of DAPT in the setting of ACS are substantial. However, patients presenting with ACS only represent a fraction of patients with CAD, and the question of whether DAPT is beneficial in patients with CAD as primary prevention has also been extensively evaluated. In the CHARISMA (Clopidogrel for High Atherothrombotic Risk and Ischaemic Stabilization, Management and Avoidance) trial (ClinicalTrials.gov Identifier: NCT00050817), the use of DAPT was evaluated in a population of patients with known CVD in the form of CAD, cerebrovascular or peripheral arterial disease or multiple risk factors for CVD, such as diabetes with or without nephropathy, hypertension and hyperlipidaemia, to determine if the incidence of thrombotic events would be reduced.66,67 In the group of 12,153 patients who had symptomatic CVD, DAPT with ASA and clopidogrel versus ASA alone was shown to reduce the rate of MI, stroke or CV death (6.9% versus 7.9%; p=0.046). In the asymptomatic cohort of 3,284 patients, use of DAPT was associated with an increased incidence of 20% in the primary endpoints of MI, stroke or CV death, compared with ASA alone (6.6% versus 5.5%; p=0.20), as well as an increased rate of all-cause mortality (5.4% versus 3.8%; p=0.04) and death from CV causes (3.9% versus 2.2%; p=0.01). In terms of bleeding complications, the use of DAPT in symptomatic patients was associated with a higher rate of bleeding (1.6% versus 1.4%; p=0.39), and although not statistically significant, an even higher rate of bleeding was observed in the asymptomatic cohort that received DAPT (2.0% versus 1.2%; p=0.07).67 As a result, the CHARISMA trial demonstrated that the use of DAPT for primary prevention in patients with symptomatic CVD had a mortality benefit as well as protection from thrombotic events. However, in patients with risk factors for CVD who are asymptomatic, the use of DAPT for primary prevention may be detrimental.
Guidelines for dual antiplatelet therapy in the USA
In 2016, the ACC and AHA released a focused update on the use of DAPT in patients with CAD.3 Previously, the DAPT guidelines were a small section in the main guidelines detailing the management of patients with STEMI, NSTEMI and stable CAD, and patients undergoing myocardial revascularization or non-cardiac surgery. However, with the large influx of data and evidence generated in the past decade, a focused update dedicated to DAPT was deemed necessary. The ACC/AHA focused update centred on major areas relating to DAPT, which included risk stratification, type and initial timing of the P2Y12 inhibitor, and the duration of DAPT in different scenarios.68 Due to the scope of this review article, only the major categories of the focused update will be discussed.
Risk stratification for ischaemic and bleeding events
It is widely recognized that a significant portion of patients with CAD may be at high risk for both ischaemic and bleeding complications.3 In the ACC/AHA focused update, the DAPT score is recommended as a risk stratification tool to determine the risk versus benefit of prolonging DAPT therapy beyond 12 months.59 The DAPT score was developed from the DAPT trial, and risk stratifies patients according to the presence of certain risk factors.59 DAPT therapy beyond 12 months is recommended in patients with a DAPT score of 2 or more, as prolonged DAPT therapy will decrease the rate of ischaemic events without increasing the rate of bleeding events in these patients.69 However, the ACC/AHA focused update did not recommend any specific predictive models when it came to assessing bleeding risk and instead focused on treating bleeding risk factors in a qualitative way.
Type and initial timing of P2Y12 inhibitor
When it comes to choosing a particular P2Y12 inhibitor, the ACC/AHA guidelines based their recommendations on the clinical scenario at hand. In patients who present with NSTEMI or STEMI and who have no contraindications to DAPT therapy, the ACC/AHA update recommends starting ASA in combination with either ticagrelor or prasugrel over clopidogrel, with a class of recommendation (COR) IIa and level of evidence (LOE) B. However, in terms of initiation of DAPT therapy in patients with ACS, the ACC/AHA update recommends a loading dose of P2Y12 inhibitor in patients with NSTEMI undergoing PCI, with stent placement with COR I and LOE A, and as early as possible in patients presenting with STEMI with COR I and LOE B, which was unchanged from the previously published guidelines.3
Dual antiplatelet therapy duration
The topic of DAPT duration is still an area of great debate. For patients with stable CAD that were undergoing PCI, the ACC/AHA update based their recommendations on 11 trials centred on this particular question. Currently, the ACC/AHA recommends lifelong ASA therapy with COR I and LOE B, clopidogrel for 1 month if a BMS is placed with COR I and LOE A, and 6 months if a DES is placed with COR I and LOE B. The patients who tolerate DAPT for that period of time and are not considered high risk for bleeding complications are candidates for prolonged DAPT therapy with COR IIb and LOE A; however, the recommended duration was unspecified. On the other hand, patients treated with DES who are considered high-risk for bleeding or develop significant bleeding can discontinue DAPT after at least 3 months with COR I and LOE C.3
Patients undergoing percutaneous coronary intervention for acute coronary syndrome
The ACC/AHA focused update recommends ASA therapy with COR I and LOE B in combination with a P2Y12 inhibitor for at least 12 months, regardless of the type of stent implanted. If no significant contraindications exist, ticagrelor or prasugrel should be the P2Y12 of choice for maintenance therapy with COR IIa and LOE B. If the patient tolerated DAPT without any significant bleeding complications, therapy can be extended beyond 12 months (COR IIa, LOE A). If the patient does develop major bleeding, or the bleeding risk is significant, then DAPT therapy may be discontinued after 6 months (COR IIb, LOE C).3
Dual antiplatelet therapy for patients undergoing coronary artery bypass graft surgery
The topic of DAPT in the perioperative period was covered in the 2016 ACC/AHA focused update to provide management guidance to clinicians. It is recommended that DAPT be restarted as soon as the bleeding risk is acceptable after CABG surgery for patients with ACS, or those that have had stent placement with continuation of DAPT for the 12-month period previously recommended with COR I and LOE B. DAPT for 12 months should also be considered in patients undergoing CABG for stable CAD to better improve the patency of vein grafts, with recommendations COR II and LOE B.28 Recommendations regarding withholding DAPT prior to surgery has been a matter of great debate. In the 2016 focused update, it was recommended that clopidogrel and ticagrelor should be discontinued at least 5 days prior (COR I and LOE B), and prasugrel discontinued at least 7 days prior to CABG (COR I and LOE C), to minimize intra-operative and post-operative bleeding complications. If CABG surgery is determined to be urgent, CABG can be performed if clopidogrel or ticagrelor are withheld less than 5 days and prasugrel for less than 7 days before surgery (with COR IIb and LOE C), but should not be performed if the P2Y12 inhibitors have been withheld for less than 1 day (COR I and LOE B).3
Medically managed patients
The 2016 ACC/AHA focused update based their recommendations on DAPT in patients managed with a non-invasive approach from evidence provided by the CURE, TRILOGY ACS and PLATO trials.15,21,23,26,27 As a result of the data provided by these trials, it is recommended that patients with ACS are treated medically with DAPT and ASA, and either clopidogrel or ticagrelor for at least 12 months; this is supported by COR I with LOE A. If the patient’s bleeding risk is acceptable, ticagrelor is preferred over clopidogrel with COR I, LOE B, and prolongation of DAPT beyond 12 months can be considered (COR IIb, LOE A).3
European guidelines
Risk stratification for ischaemic and bleeding events
Much like the ACC/AHA update on DAPT, the ESC guidelines recommend prolonging DAPT therapy beyond 12 months in patients with a DAPT score of ≥2, as the risk for ischaemic events is thought to be greater in these patients and DAPT will not significantly increase bleeding risk.70 However, since the ESC guidelines were published in 2017, the results of the Predicting Bleeding Complication in Patients Undergoing Stent Implantation and Subsequent Dual Antiplatelet Therapy (PRECISE-DAPT) study were able to be incorporated into the guidelines.71 As such, the ESC guidelines recommend using the PRECISE-DAPT score to assess bleeding risk, which consists of age, creatinine clearance, haemoglobin, white blood cell count and prior spontaneous bleeding, to predict the potential for bleeding complications.71 Therefore, concurrent use of the DAPT and PRECISE-DAPT scores may be reasonable to better risk-stratify patients who would potentially benefit from prolonged DAPT, while at the same time taking into account potential bleeding risk in a quantitative manner.70
Type and initial timing of P2Y12 inhibitor
In patients presenting to the hospital with NSTEMI or STEMI and no contraindications, ASA therapy is recommended by the ESC in combination with ticagrelor or prasugrel with LOE B and COR I, due to the emphasis of evidence provided by two large clinical trials.24,72 With regard to pre-treatment with a P2Y12 inhibitor, the ESC guidelines provided more detail than the ACC/AHA focused update on DAPT. In the ESC guidelines, in patients with NSTEMI, pre-treatment with ticagrelor or clopidogrel should be considered early, irrespective of whether an invasive or conservative approach will be undertaken, and given COR IIa and LOE C. Prasugrel, on the other hand, is reserved for patients being managed with an invasive approach with PCI when the coronary anatomy is known; otherwise its use in ACS is not recommended with COR III and LOE B. Patients that were treated with thrombolysis are a special consideration covered in the ESC guidelines; in these patients, the recommended P2Y12 is clopidogrel, with COR I and LOE A recommendations, as these patients were excluded in the ticagrelor and prasugrel trials. Furthermore, the ESC guidelines also covered DAPT therapy in patients with stable CAD undergoing PCI, with the recommended agent being clopidogrel with COR I and LOE A.70
Dual antiplatelet therapy duration
In the ESC guidelines, DAPT duration recommendations vary more than the ACC/AHA focused update on DAPT therapy. In patients with stable CAD who undergo PCI with stent placement, the ESC guidelines recommend at least 6 months of DAPT therapy, regardless of the type of stent placed with COR I and LOE A. One notable difference between the USA guidelines and the ESC guidelines pertains to patients in Europe treated with drug-coated balloons – a treatment that is not performed in the USA.3 The ESC recommends 6 months of DAPT for patients treated with drug-coated balloons, with COR IIa and LOE B. For patients who tolerated DAPT for 6 months and who are considered to have low bleeding risk but are at high risk for thrombotic complications, prolongation of DAPT beyond 6 months and up to 30 months can be considered, with COR IIb and LOE B. However, those patients who demonstrate a high risk for bleeding can potentially discontinue DAPT after 3 months with COR IIa and LOE B, or even after 1 month with COR IIb and LOE C if the bleeding risk is substantial enough.70
Patients undergoing percutaneous coronary intervention for acute coronary syndrome
The ESC guidelines are similar to the ACC/AHA focused update recommendations when it comes to patients undergoing PCI for ACS. In the ESC guidelines, DAPT for at least 12 months is recommended in patients with ACS who undergo PCI (COR I and LOE A). DAPT duration can also be extended beyond 12 months in patients who tolerated DAPT without any major bleeding complications (COR IIb, LOE A); however, discontinuation after 6 months of DAPT can be considered in patients at high risk of bleeding complications (COR IIa, LOE B). If DAPT therapy is extended beyond 1 year, the ESC guidelines recommend ticagrelor as the P2Y12 inhibitor of choice over clopidogrel (COR IIb and LOE B).70
Dual antiplatelet therapy for patients undergoing coronary artery bypass graft
The 2017 ESC guidelines take a slightly different approach when it comes to the recommendations regarding DAPT prior to CABG. The ESC guidelines recommend a heart team determines the optimal timing of surgery, as well as appropriate DAPT during the peri-operative period, and assign this recommendation COR I and LOE C. The ESC guidelines recommend continuing ASA therapy throughout the peri-operative period (COR I and LOE C), with resumption of a P2Y12 inhibitor as soon as the bleeding risk is acceptable in those patients that had PCI with stent placement prior to CABG (COR I and LOE C). In those patients who have significant bleeding risk as determined by the heart team, DAPT therapy is recommended for 6 months (COR IIa and LOE C), but should be continued for at least 12 months and up to 36 months in patients who have had prior MI and a low risk of bleeding complications (COR IIb and LOE C).70
Medically managed patients
Much like the 2016 ACC/AHA focused update, the 2017 ESC guidelines on DAPT based their recommendations regarding DAPT management in patients with ACS on results from the CURE, TRILOGY ACS and PLATO trials.15,21,23,26,27 The ESC guidelines recommend DAPT for at least 12 months with ASA and clopidogrel or ticagrelor (with COR I and LOE A), with ticagrelor preferred if the patient does not have increased bleeding risk (COR I, LOE B). In patients considered to be high risk for bleeding complications, DAPT can be stopped after 1 month, with COR IIa and LOE C. Prasugrel use in DAPT for patients with ACS managed non-invasively was given COR III and LOE B.70
The ESC guidelines also made recommendations regarding discontinuation of a P2Y12 inhibitor prior to surgery. Ticagrelor can be discontinued 3 days before surgery, clopidogrel 5 days before and prasugrel at least 7 days before, as long as there are no other relative contraindications to halting the P2Y12 inhibitor. The ESC guidelines also recommend that patients at high risk for surgical bleeding who have had PCI with stent placement within the previous month should be bridged with an intravenous antiplatelet agent after discontinuation of DAPT as they have a shorter half-life (COR IIb and LOE C).68
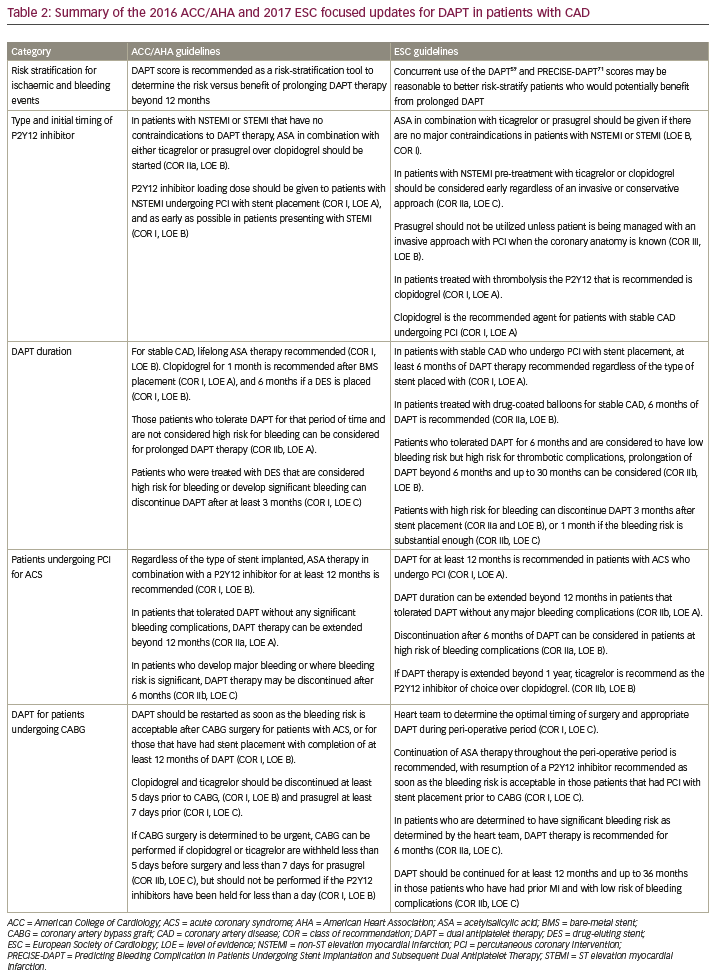
In general, both the ACC/AHA and ESC guidelines, summarized in Table 2, recommend more potent agents, prasugrel and ticagrelor, for those at higher risk of ischaemic events after ACS, and mention the DAPT score as a tool for assessing the risk:benefit ratio of >12 months DAPT after PCI.59,71 The ESC update was published a year later and was able to include the PRECISE-DAPT score, which uses five patient-derived variables (haemoglobin, white blood cell count, age, creatinine clearance and prior bleeding) to help decide whether shorter (3–6 months) or standard/longer (12–24 months) DAPT may be appropriate after PCI, based on bleeding risk.
Clinical implications and guidance
Optimal management of DAPT in patients with high risk for CVD is a challenging and, at times, daunting task. There are a multitude of factors that need to be considered and, more often than not, clinicians find themselves making decisions in relatively grey areas, as patients seldom fit into a particular set of recommendations. Clinicians must weigh multiple factors when making these decisions; however, with the large collection of data and guidelines currently available, plus new data and evidence constantly being reported, clinicians need to make individualized decisions that maximize their ischaemic benefits while minimizing bleeding. In general, for most patients at high risk for CVD, the net clinical benefit favours the use of DAPT. A helpful framework is using the DAPT and the PRECISE-DAPT scores as tools for assessing the risk:benefit ratio of prolonged versus shorter duration DAPT during a candid discussion with the patient.