Background: Remote monitoring (RM) has routinely not been provided to patients with low-energy devices; there are limited data on the service burden, volume of and type of alerts received and their management.
Objective: Collect and analyse data on alert type, service burden and management of alerts in low-voltage devices over 12 months of RM.
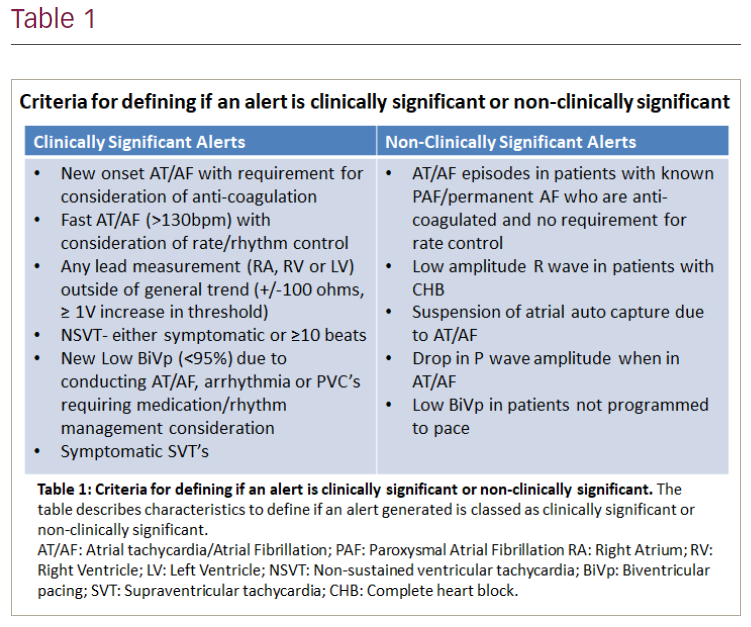
Methods: All patients implanted (Group 1) or with a scheduled follow-up (Group 2) with a pacemaker (PPM) or cardiac resynchronisation therapy pacemaker (CRTP) from April to November 2020, were prospectively enrolled. These were followed from the first transmission for 12 months. Patients transferred to another centre were excluded. Alerts were categorised (Table 1) and subsequent intervention assessed.
Results: A total of 263 patients were enrolled; 28% males, mean age 75 (SD 14) years, 201 PPM, 62 CRTP, 63% Group 1 and 37% Group 2. Manufacturers included Abbott (27%), Boston Scientific (53%), Medtronic (20%) and Biotronik (1%). Over 12 months 1,566 alerts were received from 109 patients (41%) of the cohort. This resulted in 160 reports with 41 requiring escalation and clinical action (2.6% of all alerts). There was a median (IQR) of 4 (2–7.5) alerts and 2 (1–3) reports per patient. Alerts were split into clinically significant 893 (57%) and non-clinically significant 673 (43%). Alert breakdown: atrial arrhythmia 43.4%, ventricular arrhythmia 41%, low biventricular pacing 11.9%, intrinsic amplitude 2.5%, threshold 1.1% and impedance 0.2%. Overall Group 1 generated significantly more alerts than Group 2 (1007 vs 559; p<0.001). Clinically significant alerts were also greater in Group 1 (731 vs 162; p<0.001) and resulted in significantly more reports (124 vs 36; p<0.001). Thirty-four patients were escalated with 5 patients escalated more than once. Of these, 30 (73%) came from Group 1; 20 for urgent consideration of anti-coagulation or arrhythmia management (12 and 8, respectively), 4 non-urgent outpatient review and 6 for review in device clinic. The remaining 11 escalations from Group 2 included 4 urgent medical reviews (3 arrhythmia management vs 1 anti-coagulation), 4 non-urgent medical reviews and 3 for device clinic. Of the non-clinically significant alerts, the largest proportion were for atrial arrhythmia duration and/or burden (63.8%) for patients with management plans in place. Inappropriate low biventricular pacing (BiVp) alerts triggered 62% (109) times in asymptomatic, known low BiVp patients or those who were not programmed to pace. 13.3% were for non-sustained ventricular arrhythmias (<10 beats in duration). Finally, 5% were for out-of-range lead measurements in patients with known complete heart block or those with suspension of automatic atrial thresholds in the presence of known atrial arrhythmia.
Conclusion: Home monitoring in patients with low-voltage devices generate a moderate number of alerts over 12 months, with the largest proportion of alerts seen in those with new implants. Low numbers of alerts require clinical escalation. Nearly half of all alerts were inappropriate and non-actionable or were repeat alerts of the same finding. Development of strategies to tailor alerts from implants, or once an alert received is actioned and no longer relevant, is essential to reduce the overall burden of alerts. ❑