Introduction: The HeartLogic (HL) index (Boston Scientific) is a novel multisensory approach in the monitoring of heart failure (HF) patients with ResonateTM cardiac defibrillator devices. Without a dedicated HF nurse team onsite at St Bartholomew’s Hospital, and the subsequent COVID-19 pandemic, it has been vital to liaise with patients’ local community care teams to reduce hospital attendances. Therefore, a hub-and-spoke model has evolved to initiate clinical reviews and medication changes for patients at risk of HF decompensation.
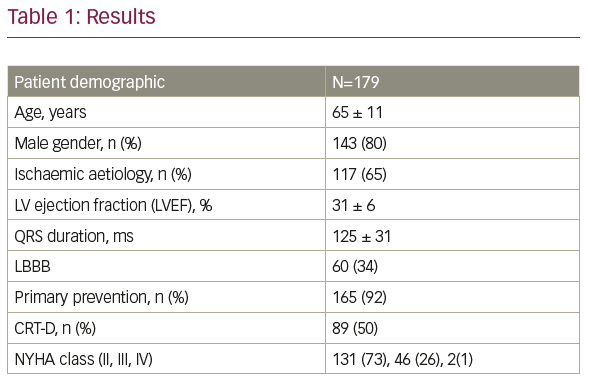
Methods: The local criteria for HL activation included a HF diagnosis and NYHA class II+; patients were activated in batches to stagger initial alerts. From December 2019 to February 2021, HL was activated for 179 patients (Table 1 shows the baseline clinical characteristics). The median follow-up duration (from activation to last follow up or death) was 16 months (25th–75th percentile: 8–17), a total of 161 patient years. A total of 9 patients died during follow up (5 due to COVID-19) and 5 were in alert state at the time. All active alerts were reviewed twice a week by a cardiac scientist, and the alert trend and contributing factors examined. If the alert had a sudden onset, the patient’s symptoms were assessed via a phone call using a locally developed questionnaire. If the alert had a gradual onset, a ‘watch and wait’ approach was adopted as patient symptoms may not have manifested yet and the call was undertaken a week later. Depending on the patient’s condition and alert duration, further monitoring or escalation to the local HF team for medication review was arranged.
Results: The HL index crossed the threshold value (16) 198 times (1.2 alerts/patient year) in 89 patients (up to 7 times per patient). The median alert duration was 48 days (25th–75th percentile: 14–99). Overall, the total time in alert state for the entire patient population was 26 years (16% of the total observation period). The maximum HL index value was 31 ± 12. The HL sensors detected changes in heart sound amplitude in 155 (78%) alerts; decreased thoracic impedance for 116 (59%) alerts; increased respiratory rate for 110 (56%) alerts; and increased night heart rate for 95 (48%) alerts. Kaplan–Meier plots of the time to the first HL alert, stratified by baseline characteristics, showed no significant differences between subgroups. However, Cox regression analysis showed that lower LVEF at time of implant was a predictor of HL alerts (p=0.002; hazard ratio 0.95; 95% CI, 0.92–0.98). Although, a sub-analysis of the MultiSENSE study (Gardner et al. 2018) demonstrated HL maintains its predictive value for HF events after correction for baseline variables, including LVEF.
Conclusions: The present analysis includes one of the largest patient populations managed with HL described to date and demonstrates that the clinic’s alert burden is comparable to that seen in the MultiSENSE trial (2 alerts per patient per year). Cardiac scientists leading this service have adapted the alert reporting and escalation process to ensure it is sustainable long term. This has brought together multidisciplinary professionals to coordinate care in line with the NHS Long-Term Plan for these high-risk heart failure patients.