Introduction: The Micra TPS, a leadless single-chamber ventricular pacemaker, is increasingly preferred over the transvenous system. Its significantly smaller profile and fewer reported adverse effects, without compromising the pacing efficacy, makes it an innovative pacing device. We report the first sequential 75 Micra insertion cases in Northampton General Hospital (NGH) and 6 months post insertion data to investigate implantation success, pacing thresholds, deployment attempts and adverse effects. The data gathered aims to provide insight into the safety of Micra implant service offered by the only UK District General Hospital with no on-site cardiac surgery backup. A protocol was agreed for emergency transfer to a surgical centre if required. Vascular access ultrasound, echocardiogram and pericardiocentesis kit were available in the lab. Implanters were trained and proctored by Medtronic.
Methods: All patients who had a Micra implant attempted in NGH were included. Implantation and 6-month pacing data were recorded. Results are presented in percentage and compared to the Micra Post Approval Registry (PAR).
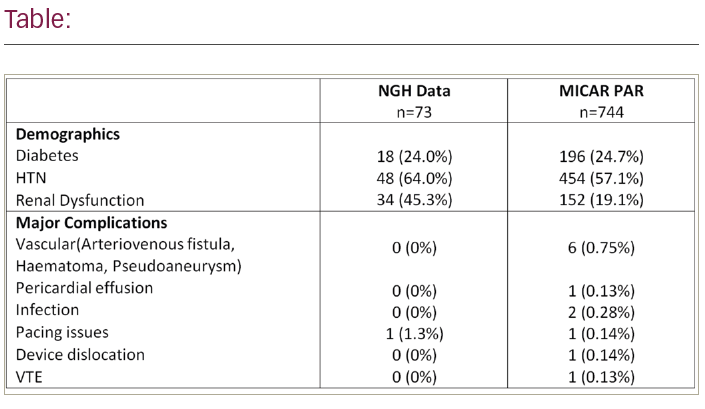
Results: There was successful implantation in 100% of the patients (age 76.58 ± 9.56), with 51 males (68%) (age 76.58 ± 9.56). 6 out of 75 patients are currently awaiting 6 month pacing interrogation. One patient died before the 6-month check, unrelated to the Micra implant. 97.0% (n=65) of patients had adequate pacing capture threshold (PCT) at the 6-month follow up meaning PCT ≤2 volts at 0.24 ms pulse width and the increase in PCT from implant to 6 months ≤1.5 volts. This correlates to the PAR study with 97% patients in this group. There were no long-term complications. There was only 1 major complication – a patient with a raised threshold immediately post-implant, settling to 1.88V at 6 months. There were no device infections, tamponade, major vascular complications, device dislocation or VTE. Pacing indications were AF with bradyarrhythmia (76.0%, n=57), Sinus or AV nodal disease (5.3%, n=4), infection (endocarditis, infected device removal) (8.0%, n=6), removal of conventional pacemaker for cancer radiotherapy (8.0%, n=6) and “twiddlers” syndrome (2.7%, n=2). There was reduction in fluoroscopy time (mean of 8.50 ± 1.03 min in first 10 cases to 4.80 ± 0.42 in the last 10) and our Micra deployment attempts (mean of 2.7 ± 0.83 in first 10 cases to 1.3 ± 0.15 in the last 10). In our initial 20 implants, we had 5 episodes of minor bleeding (25%) needing manual compression. We introduced double Z sutures technique with a resultant reduction to 1 episode of minor bleeding in the next 55 cases (1.8%).
Conclusion: We are the first non-surgical centre / District General Hospital in the UK and the second in Europe offering Micra implantation. Over the course of implants, both our fluoroscopy time and number of Micra deployments have improved. This study, with a low number of complications corresponding to the primary outcomes in the PAR study, indicates non-surgical centre Micra implant with proctoring and protocols, is both feasible and safe.