Introduction: Clinical pharmacists are a new workforce in Primary Care Networks (PCNs) who play a vital role in medication optimisation and high-risk drug monitoring. With the popularity of DOACs growing and increasing treatment options becoming available to patients and clinicians, there is also an increased risk of prescribing errors. Thus, it is important to ensure that oral anticoagulants are prescribed safely and optimised for individual patients, to reduce the risk of stroke and minimise risk of bleeding. The aim of this project was to implement the PERFECT pathway to ensure safe and effective prescribing of DOACs. In particular, the focus was to review if patients were prescribed the correct DOAC dose and were monitored appropriately in accordance with national and local guidelines.1,2
Method: A search was conducted on EMIS clinical system in all three practices in the Crouch End PCN, to identify all patients currently prescribed a DOAC. In-house training was provided to clinical pharmacists by the anticoagulation specialist to support upskilling. The pharmacists conducted clinical virtual reviews for patients prescribed DOACs and reviewed indication, dose, renal function, weight, blood monitoring (FBC, LFTs, U&Es) and potential drug interactions. For cases where a pharmacist intervention was required, this was discussed with the patient’s named GP and/or their anticoagulation clinician. Respective changes were made to patient’s treatment plans, following appropriate discussions with the patient.
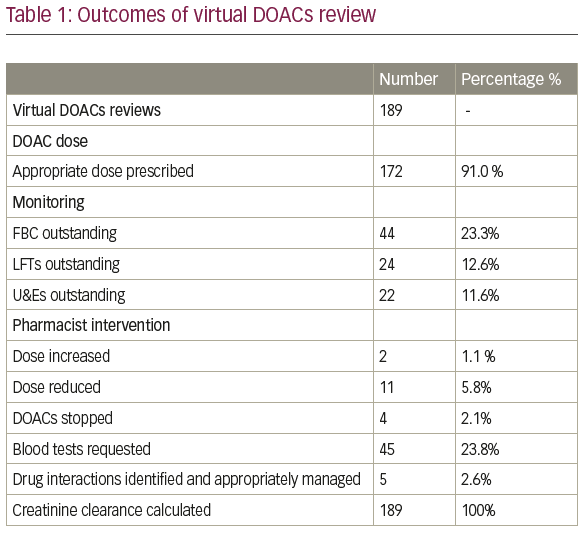
Results: Table 1
Discussion: In total, 189 patients were reviewed across 3 practices. The creatinine clearance was calculated for all patients to review dose. Of these reviews, 2 patients required an increased dose, 11 required dose reductions (either due to age or impaired renal function), and 4 patients whose DOAC treatment duration had elapsed had their prescriptions stopped. Interacting anti-epileptics were co-prescribed for 4 patients requiring further specialist input and secondary care referral. The emergence of the COVID-19 pandemic may also have been a possible reason for outstanding blood tests due to restricted pathology services and patient’s refusal to attend blood test appointments.
Conclusion: The addition of clinical pharmacists in the PCN has led to an improvement in the quality and safety of anticoagulant prescribing and monitoring. Pharmacists can play a crucial role in reducing prescribing errors through routine high-risk drug monitoring, implementation of improvement strategies and share learning with the multidisciplinary team to ensure sustainability of outcomes. The pharmacy workforce will continue to support the delivery of the NHS Long-Term Plan ambition, principally through secondary prevention.
References:
- NCL JFC DOAC prescribing support for NCL AF and VTE, December 2018.
- EHRA Practical Guide on the Use of Non-Vitamin K Antagonist Oral Anticoagulants in Patients with Atrial Fibrillation, April 2021.