Aims: The association between obstructive sleep apnoea (OSA) and atrial fibrillation (AF) is yet to be fully delineated. Although several observational studies have suggested an independent association between OSA and AF, subsequent randomised controlled trials have failed to demonstrate any benefit of OSA treatment on reducing AF incidence. Complicating the interpretation of the data on OSA and AF is the strong association of both these conditions with obesity, which may act as a confounder, and it is therefore unclear whether this association is mediated by shared co-morbidities such as obesity. We performed Mendelian randomisation (MR) to investigate the causal relationship between OSA, body mass index (BMI) and AF.
Methods: Mendelian randomisation utilises genetic variants in instrumental variable analysis to investigate relationships between modifiable risk factors and outcomes in observational data. Using genetic variants that are independently and randomly inherited as proxies for modifiable exposures enables causal inference concerning outcomes, overcoming limitations of classical observational epidemiology; namely, confounding and reverse causality. Single-nucleotide polymorphisms associated with OSA and BMI were selected as instrumental variables to estimate associations of BMI and OSA with AF among 55,114 cases with AF and 482,295 controls.
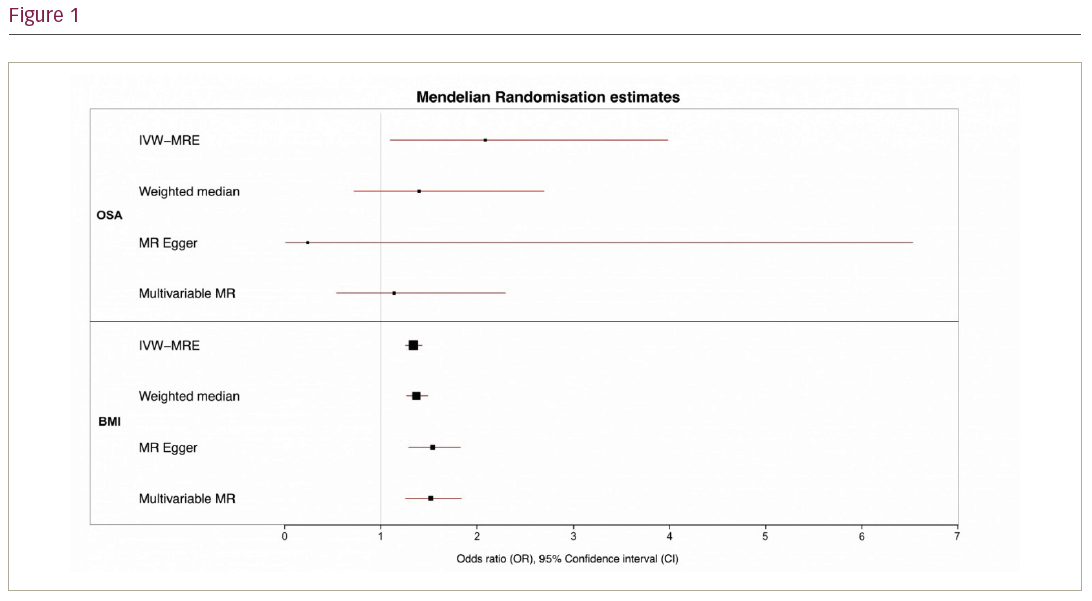
Results: Primary analysis was conducted using inverse-variance weighted MR. Genetically-predicted OSA and BMI were both significantly associated with increased odds of AF (per odds ratio unit increase in OSA: OR 2.09; 95% CI, 1.10–3.98; p=0.03; per kg/m2 increase BMI: OR 1.34; 95% CI, 1.26–1.43; p<0.001). However, the association between genetically-predicted OSA and AF was no longer observed in sensitivity analyses that are more robust to the presence of pleiotropy, whilst associations between genetically-predicted BMI and AF remained consistent. Similarly, in multivariable MR, genetically-predicted OSA was not associated with AF when adjusting for genetically-predicted BMI (OR unit increase for OSA 1.14; [95%CI, 0.54–2.30], p=0.86). Genetically predicted BMI remained associated with AF after adjusting for genetically predicted OSA (OR 1.52; [95% CI, 1.26–1.84] per kg/m2 increase; p=0.049) (Figure 1).
Conclusion: Our data suggest that OSA is not independently causal of AF and their association is attributable to mediation or confounding from obesity, while we confirm that obesity is causally associated with AF. Our results highlight a hierarchy of importance for the putative modifiable risk factors for AF, with evidence for obesity being stronger than that for OSA, suggesting that weight reduction treatments may be potentially more effective than OSA treatments in reducing AF burden.