Individuals with aortic stenosis frequently have coronary artery disease (CAD).1 Both conditions share a common pathophysiology involving low‐density lipoprotein-mediated inflammatory response, resulting in an accelerated atherosclerotic process.2 They also share similar risk factors, such as age, smoking, hypertension, diabetes mellitus, hyperlipidaemia and chronic kidney disease.3,4 More than 50% of patients with severe aortic stenosis undergoing treatment with surgical aortic valve replacement or transcatheter aortic valve replacement (TAVR) have concomitant CAD.5–7 Due to a lack of randomised controlled trials (RCTs) and exclusion of significant CAD in TAVR trials, the optimal method of revascularisation of CAD in patients undergoing TAVR remains controversial, with several observational studies and meta-analyses showing conflicting results.6,8–15 Nevertheless, current guidelines give a class IIa recommendation for percutaneous coronary intervention (PCI) in patients undergoing TAVR with significant CAD involving >70% diameter stenosis in a major coronary artery, or >50% diameter stenosis in left main coronary artery.16,17
Prevalence of coronary artery disease in transcatheter aortic valve replacement population
The prevalence of CAD in patients with TAVR varies from 30–80%.18–25 Based on varying definitions of significant CAD, about 50–70% of patients with aortic stenosis have concomitant significant CAD,6,8,26,27 with 50% having multivessel CAD.10,26,28–30 In the FRANCE 2 (French Aortic National CoreValve and Edwards 2) registry of 3,195 patients that underwent TAVR, 48% had CAD, 16% had history of myocardial infarction, and 18% had prior surgical coronary revascularisation.31
Impact of coronary artery disease on transcatheter aortic valve replacement outcomes
Studies evaluating outcomes of patients undergoing TAVR who also have concomitant CAD have shown conflicting results. Dewey et al. showed significantly higher 30-day and 1-year mortality in patients with history of coronary artery bypass grafting or PCI undergoing TAVR.20 A meta-analysis by Sankaramangalam et al., which included 15 studies with 8,013 patients, demonstrated that patients with CAD had no difference in 30-day all‐cause mortality (odds ratio [OR] 1.07; 95% confidence interval [CI] 0.82–1.40; p=0.62) but a significant increase in 1-year all‐cause mortality (OR 1.21; 95% CI 1.07–1.36; p=0.002) post-TAVR, compared to those without CAD.32 In contrast, multiple studies have shown no difference in outcomes in patients with or without CAD undergoing TAVR.10,27,33–5 In particular, a study by Khawaja et al. showed no difference in 30-day or 1-year mortality in patients with significant CAD who underwent TAVR.10 However, patients with a Synergy Between Percutaneous Coronary Intervention with Taxus and Cardiac Surgery (SYNTAX) score >9 at the time of TAVR had greater 30-day and 1-year mortality compared to those with a score <9.10 Among patients who underwent TAVR, Masson et al. reported no difference in 30-day mortality, 1-year mortality or left ventricular systolic function recovery between those with and without CAD, classified by Duke Myocardial Jeopardy Score (DMJS).34 Chauhan et al. showed, in patients with CAD undergoing TAVR, there was no significant association between SYNTAX or DMJS and primary composite endpoint of postoperative coronary revascularisation, all‐cause mortality and major adverse cardiovascular and cerebrovascular events (MACCE).33 A meta-analysis by D’Ascenzo et al., which included data from seven observational studies, showed no difference in all-cause mortality in patients with and without CAD undergoing TAVR.35
Impact of coronary revascularisation on transcatheter aortic valve replacement outcomes
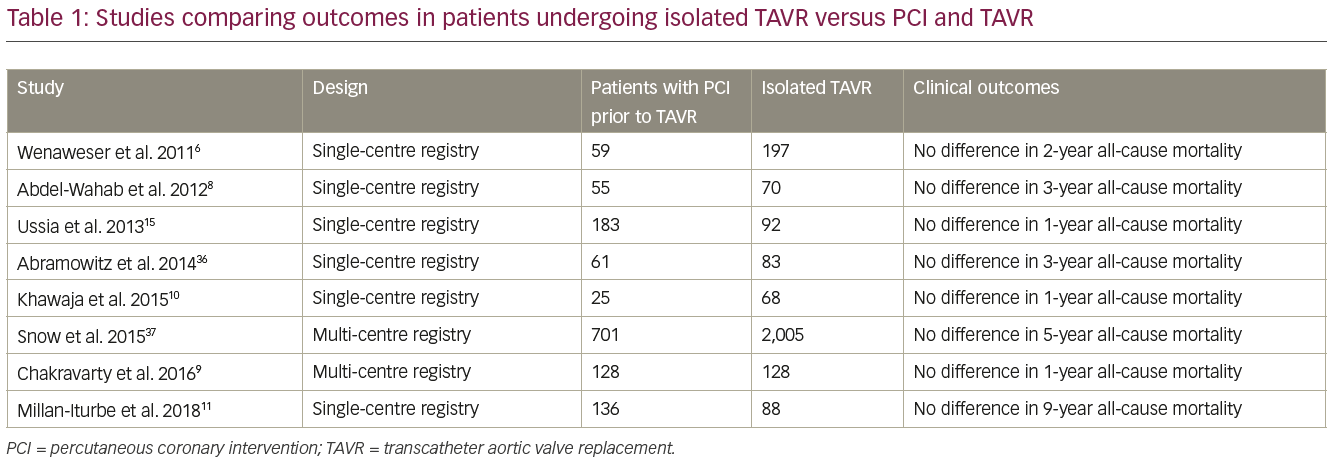
The RCTs of TAVR excluded patients with severe CAD.18,20–5 There are no RCTs evaluating outcomes of coronary revascularisation before or during TAVR in patients with concomitant CAD, and several observational studies and meta-analyses have reported conflicting results.6,8–15,30,36,37 Multiple single-centre registries showed no difference in mortality in follow-up up to 5 years in patients that underwent PCI prior to TAVR versus TAVR alone (Table 1).6,8–11,15,36,37
A meta-analysis by Kotronias et al., including nine studies with 3,858 patients, showed that patients with CAD who underwent revascularisation prior to TAVR had a higher rate of vascular complications (OR 1.86; 95% CI 1.33–2.60; p=0.0003) and all-cause mortality (OR 1.42; 95% CI 1.08–1.87; p=0.01) at 30 days with no difference in cardiovascular mortality, myocardial infarction, acute kidney injury or 1-year mortality.26 A more recent meta-analysis by Lateef et al., including 11 studies with 5,580 patients, found no difference in 30-day all-cause mortality (OR 1.30; 95% CI 0.85–1.98; p=0.22), stroke (OR 0.7; 95% CI 0.36–1.45; p=0.36), myocardial infarction (OR 2.71; 95% CI 0.55–12.23; p=0.22), acute kidney injury (OR 0.7; 95% CI 0.46–1.06; p=0.08) or 1-year all-cause mortality (OR 1.19; 95% CI 0.92–1.52; p=0.18) in patients who underwent TAVR with and without PCI.38 Overall, the impact of coronary revascularisation in patients with concomitant severe aortic stenosis is a subject of ongoing debate.
Ischaemia evaluation in patients with concomitant coronary artery disease and aortic stenosis
Non-invasive stress testing
In patients with severe aortic stenosis and concomitant CAD, the identification of ischaemia secondary to CAD can be challenging as aortic stenosis causes myocardial ischaemia on stress testing in the absence of angiographically significant CAD, which generally tends to disappear after valve replacement.39 Hence, non-invasive stress testing has lower sensitivity and specificity for detecting CAD in severe aortic stenosis patients.39,40 There are no data to support the use of non-invasive assessment to guide revascularisation in patients undergoing TAVR. However, non-invasive stress testing can be helpful if the area of ischaemic myocardium matches the territory subtended by the stenosed coronary artery.
Invasive coronary functional assessment
Although fractional flow reserve (FFR) and instantaneous wave-free ratio (iFR) are standard methods of invasive physiologic assessment of CAD, there is significant ambiguity interpreting these results in patients with severe aortic stenosis.41 This is due to the unequal changes on proximal pressure waveforms caused by stenosed aortic valve, the haemodynamic effect of the uncoupling of aortic valve closure from a decrease in left ventricular pressure, and the effect of left ventricular hypertrophy on microvascular function.42 However, a recent study by Ahmad et al. showed iFR values did not change pre- and post-TAVR (p=0.73), whereas FFR decreased significantly post-TAVR compared with pre-TAVR (p=0.001) indicating iFR may be reliable in identifying significant CAD.43
Impact of extent of revascularisation on transcatheter aortic valve replacement outcomes
Though there are no RCTs in this sphere, there are several observational studies and meta-analyses that evaluated the effect of completeness of revascularisation on post-TAVR outcomes. The residual SYNTAX score (rSS) is an objective measure of the degree and complexity of residual CAD after PCI, and is a powerful indicator of 5-year mortality.44 Recent single-centre registry data12–4,30 showed that patients who underwent PCI prior to TAVR and had low rSS, ranging from 0–14, had a lower incidence of MACCE over 5 years of follow-up when compared with high rSS.12–4,30 A meta-analysis by D’Ascenzo et al., which included 13 studies and 8,334 patients, showed mere presence of CAD had no effect on 30-day or 1-year mortality in patients who underwent TAVR, but those patients with CAD and SYNTAX score >22 had higher 1-year mortality (OR 1.71; 95% CI 1.24–2.36) and those with a rSS <8 post-PCI had lower 1-year mortality (OR 0.34; 95% CI 0.012–0.93).28 Witberg et al. showed that patients with a SYNTAX score >22 had higher MACCE up to 2 years after TAVR, and patients with rSS <8 had similar MACCE compared with patients without CAD.45 In another study, Witberg et al. compared the effect of severity of CAD and complete versus incomplete revascularisation (rSS >8) on TAVR outcomes, and showed higher all-cause mortality at 1.9 years in patients with SYNTAX score >22 (hazard ratio [HR] 2.091; p=0.017) and incomplete revascularisation (rSS >8) (HR 1.720; p=0.031).30
A meta-analysis by Witberg et al. including 3,107 patients from six studies with 0.7–3.0 years of follow-up showed that in patients with SYNTAX score >22, incomplete revascularisation with rSS >8 was associated with an increased risk for mortality when compared to patients with no CAD (OR 1.85; 1.42–2.40; p<0.01) or those with revascularisation and rSS <8 (OR 1.69; 1.26–2.28; p<0.001), or to both groups combined (OR 1.71; 1.36–2.16; p<0.001).46 Table 2 summarises studies evaluating impact of post-PCI rSS on TAVR outcomes.
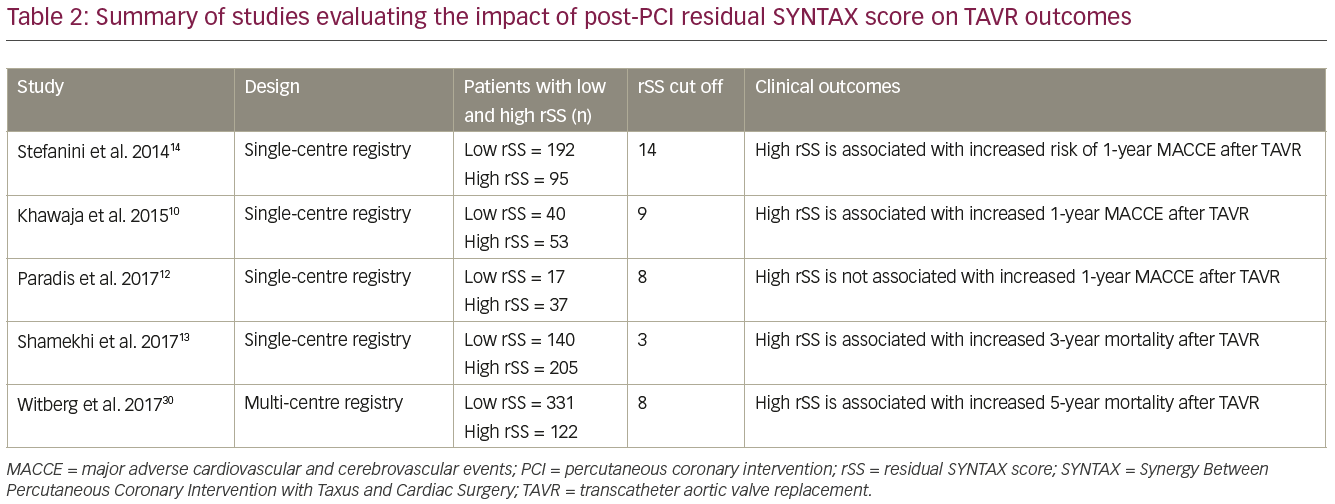
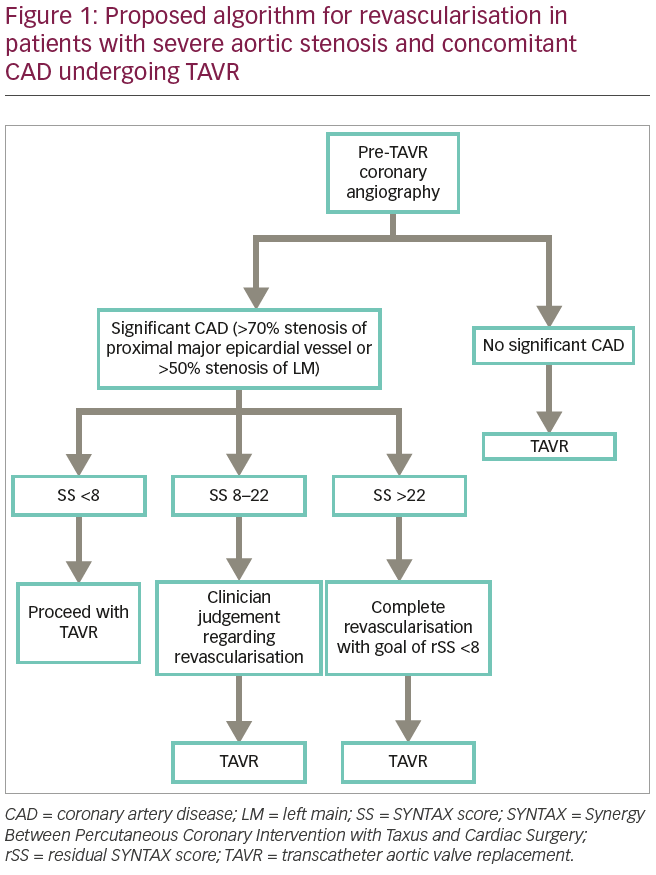
Thus, SYNTAX score could be used as a tool to help guide revascularisation prior to TAVR, and one may aim to achieve an rSS <8 with revascularisation for best outcomes post-TAVR. However, the findings of observational studies related to the effect of SYNTAX score and rSS on TAVR outcomes need to be confirmed in RCTs for their use to be incorporated into guidelines and routine practice. Figure 1 depicts our proposed algorithm for revascularisation in patients undergoing TAVR.
Timing of coronary revascularisation in transcatheter aortic valve replacement
The optimal timing of coronary revascularisation in relation to TAVR is unknown due to conflicting findings of observational studies and lack of RCTs. Although revascularisation prior to TAVR is a widely practiced approach, combining TAVR and revascularisation as a single procedure has been previously studied.
Conradi et al. showed the feasibility of performing revascularisation and TAVR as a combined procedure.47 Among 28 patients who were deemed not candidates for surgery, 21 patients underwent a two-stage approach of revascularisation prior to TAVR and the remaining seven patients underwent revascularisation followed by TAVR in a single-stage procedure. Thirty-day mortality (4.8 % versus 14.3%), fluoroscopy time and contrast volume were higher with a single-stage procedure compared to a two-stage approach with no occurrence of peri-procedural myocardial infarction or stroke in either group.47 Wenaweser et al. compared outcomes among patients who underwent revascularisation and TAVR as concomitant procedures, revascularisation prior to TAVR in a two stage procedure, or TAVR alone, and noted no significant difference in 30-day mortality between concomitant TAVR and revascularisation compared to the other two groups (11.1%, 8.7% and 5.6 %, respectively; p=0.24).6 A study by Pasic et al. showed combining TAVR and revascularisation as a single procedure had a 30-day mortality of 4.3% with no increased risk of renal failure, although lack of control arm was a limitation in this study.48
Although there are potential benefits of combining TAVR and revascularisation as a single procedure, such as fewer vascular access procedures and reduction in ischaemic burden during TAVR, there is a potential increased risk of contrast-induced nephropathy as well as increased operator and patient radiation exposure. Thus, there is a need for RCTs to better understand the optimal timing for revascularisation in relation to TAVR. A more widely practiced strategy is performing revascularisation prior to TAVR. The potential benefits of this approach include easier coronary access in the absence of a valvular prosthesis, lower ischaemic burden and related haemodynamic instability during TAVR, and lower contrast volume and radiation exposure time during each individual procedure. The potential risks include a higher risk of bleeding as these patients are on uninterrupted dual antiplatelet therapy during TAVR and increased risk of haemodynamic instability during revascularisation in the presence of severe aortic stenosis. Abdel-Wahab et al. compared the outcomes of revascularisation followed by TAVR (55 patients) versus isolated TAVR (70 patients).7 The median duration from revascularisation to TAVR was 10 days (0–90), and this small study showed a trend toward lower 30-day mortality with revascularisation prior to TAVR versus TAVR alone (2% versus 6% respectively, p=0.27) that did not reach statistical significance.7
Revascularisation in patients with left ventricular dysfunction and severe aortic stenosis is challenging as there is risk of haemodynamic instability during the procedure. Goel et al. studied 254 patients with severe aortic stenosis who underwent PCI.29 The results concluded that patients with severe aortic stenosis and low ejection fraction ≤30% had a higher 30-day post-PCI mortality compared with those with an ejection fraction >30% (5.4% versus 1.2%, respectively; p<0.001). The study also concluded that a high Society of Thoracic Surgeons (STS) score ≥10 was associated with higher 30-day post-PCI mortality compared with an STS score <10 (10.4% versus 0%, respectively; p<0.001). Mechanical circulatory support with Impella (Abiomed, Danvers, MA, USA) in selected high-risk patients, such as cardiogenic shock or severely depressed ejection fraction, is a feasible option to maintain haemodynamic stability in patients with severe aortic stenosis undergoing PCI.49,50 A recent publication from the cVAD registry, including 116 patients (mean STS score 18.7 ± 18.3%, mean left ventricular ejection fraction 27 ± 16%, and mean aortic valve area 0.67 ± 0.29 cm2) who received high-risk PCI and Impella-assisted BAV, demonstrated that elective Impella support was associated with higher 1-year survival compared to rescue placement.50 However, RCT data are currently lacking and needed for identifying the best management option in these high-risk patients.
With conflicting results from observational studies and meta-analyses, the dilemma of whether to perform revascularisation plus TAVR or TAVR alone, remains. Three ongoing RCTs will help answer this question: the ACTIVATION trial (ISRCTN75836930) is a prospective RCT that compares PCI in coronary arteries with more than 70% stenosis followed by TAVR versus TAVR alone,51 NOTION-3 (ClinicalTrials.gov Identifier: NCT03058627) is a prospective RCT comparing TAVR alone versus FFR-guided PCI plus TAVR, and the FAITAVI trial (ClinicalTrials.gov Identifier: NCT03360591) is a prospective RCT comparing angiographic- versus FFR-guided PCI in patient undergoing TAVR.
Challenges of coronary revascularisation post transcatheter aortic valve replacement
Coronary access and PCI may be challenging in patients post-TAVR. It is important to understand the structure of each transcatheter aortic valve prosthesis for optimal success. Pre-procedure computed tomography analysis is critical for TAVR procedure planning, in order to avoid coronary obstruction.52,53 A large observational study by Zivelonghi et al. showed coronary re-access and PCI are possible after TAVR.54 The authors performed coronary angiograms after TAVR in 66 patients: 25 with CoreValve™ Evolut™ R valves (Medtronic, Dublin, Ireland) and 41 with SAPIEN 3 valves (Edwards Lifesciences, Irvine, CA, USA). They successfully performed diagnostic angiography with diagnostic catheters in 96% of vessels; 4% vessels required guide catheters while one artery could not be engaged due to the unfavourable positioning of an Evolut R valve.54 They were able to successfully perform PCI in all 17 intended patients: 6 with Evolut R and 11 with SAPIEN 3 valves.54
Coronary re-engagement may be especially challenging with self-expanding Evlout R valves, as the valve extends above the coronary ostia, unlike the balloon expandable SAPIEN 3.53 However, these challenges may be overcome with increased operator experience and down-sizing of the catheter. According to a study by Boukantar et al., among patients with Evolut R valves, post-TAVR PCI was associated with significantly higher contrast usage, fluoroscopy times and radiation dosage when compared with coronary angiography performed prior to TAVR.55 Aortic stenosis indications for TAVR have recently expanded to include a lower risk population, younger patients may undergo TAVR, necessitating more frequent post-TAVR coronary procedures. Moreover, a wide variety of TAVR valves have emerged into clinical practice, including the self-expanding JenaValve™ (JenaValve technology GMbH, Munich, Germany), the Portico™ Valve (St. Jude Medical, St. Jude Medical, MN, USA), the ACURATE neo™ Valve (Boston Scientific, Marlborough, MA, USA), the Lotus Valve (Boston Scientific), and the Allegra Valve (NVT AG, Muri, Switzerland), that necessitate interventional cardiologists to become proficient in post-TAVR angiography and PCI with each different valve.
Conclusion
In summary, in patients with CAD undergoing TAVR, the SYNTAX score can be a useful tool in deciding which patients may benefit from PCI prior to TAVR. In patients with high SYNTAX score (>22), we recommend performing PCI before TAVR to improve post-TAVR outcomes. In those with low SYNTAX score (<8), no additional coronary intervention is necessary and operators can proceed directly with TAVR. However, in those with intermediate SYNTAX score (8–22), the decision to perform PCI should be individualised based on the clinical risk factors in consultation with the Heart Team. Further large-scale RCTs are required to provide definitive answers regarding management of these complex group of patients.