Background: Atrial fibrillation (AF) hospital admissions represent significant national health and economic burden. In the year 2019–2020 our hospital reported 1,333 admissions with a primary diagnosis of AF, with a 10% annual increase. A virtual AF ward providing multidisciplinary care could reshape the future model of AF management.
Methods: An AF virtual ward was implemented at our UK tertiary centre, as a proof-of-concept model of care. Patients presenting primarily with AF or atrial flutter (AFL) who were haemodynamically stable, heart rate<140 bpm and with no other acute conditions, were rendered eligible for remote management. Patients were given access to a single-lead ECG recording device (AliveCor), a Bluetooth integrated blood pressure machine and pulse oximeter with instruction to record daily ECGs, blood pressure readings, oxygen saturations and fill an online AF symptom questionnaire via a smart phone or electronic tablet. Data were uploaded to an integrated digital platform (Dignio) for review by the clinical team who undertook twice daily virtual ward rounds. Medication adjustment was arranged through the hospital pharmacy. Data were collected prospectively for patients admitted to the AF virtual ward between 31 January and 19 April 2022. Outcomes included length of hospital stay, admission avoidance and re-admissions. Re-admission avoidance was assessed using the index admission criteria as parameter for re-admission likelihood. Patients’ satisfaction was assessed using the NHS family and friends’ test (FFT).
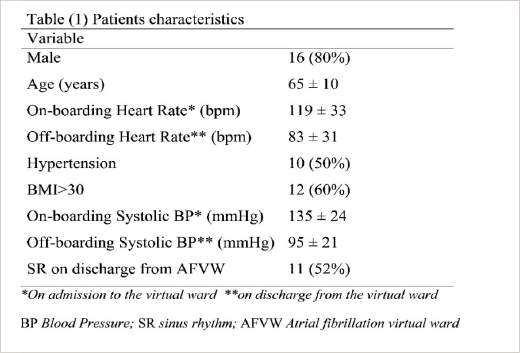
Results: A total of 20 patients were enrolled, generating 21 admissions. The age on admission was 64 ± 10 years (mean ± SD). The majority of admissions, 95% (n=20) were in AF or AFL, with only admission in sinus rhythm. Mean heart rate on admission and discharge was 119 ± 33 and 83 ± 31, respectively (Table 1). A rhythm control strategy was pursued in 76% (n=16), with half of the admissions 52% (n=11) in sinus rhythm on discharge. Initial hospital admission was completely avoided in 24% (n=5), with 10 re-admissions avoided. Two patients required hospital re-admission: one due to tachycardia requiring acute cardioversion and the other due to acute kidney injury requiring hospitalisation. The FFT yielded 100% positive responses among participants.
Conclusion: This model of care is a first real-world experience of a virtual ward for hospital patients with fast AF. It demonstrates the potential to reduce the financial and backlog pressures caused by AF admissions without compromising patient care or safety. Work is ongoing to further confirm the safety and cost-effectiveness upon further progress in a larger patient cohort. ❑
Table 1