Introduction: Covid 19-drove healthcare services to adapt in order to keep patients and staff safe from the virus. As a Cardiac Scientist (CS) manager, I was charged with developing a strategy for the Cardiac Device Follow-up service across a tertiary cardiac centre with satellite sites. We routinely performed face-to-face follow-up for 100 patients per day and over 40 via remote follow-up. Patients with high-voltage devices and implantable loop recorders were traditionally enrolled onto remote monitoring (RM) at implant. Pacemakers were typically not. These patients made up a large portion of the daily face-to-face attendees. Of the 18,000 patients within the clinic, 80% were in the high-risk category, according to Public Health England and therefore should not be attending hospital unless necessary.
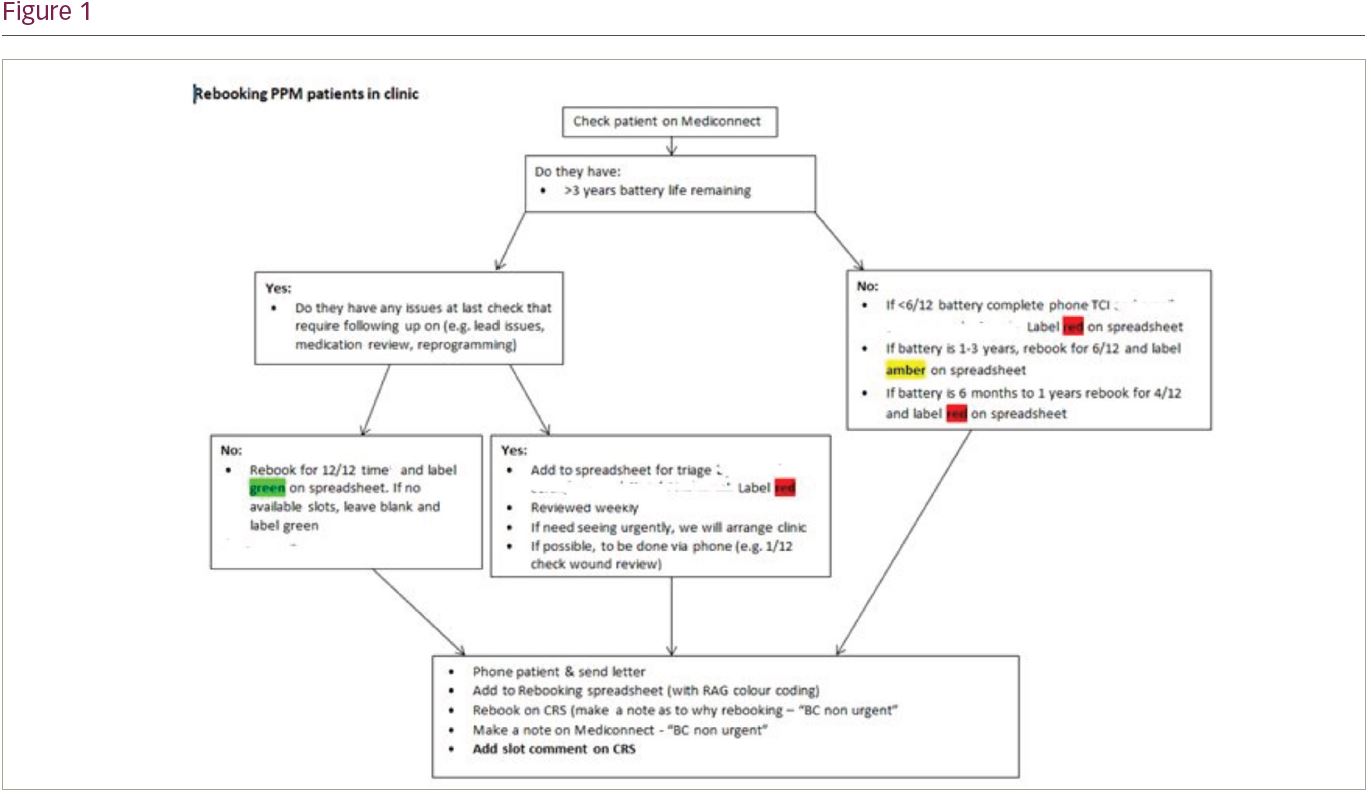
Methods: Considerations for what would be necessary attend hospital and the pathway to attend the hospital were required, along with options to provide care outside of the hospital, either remotely or locality. Working with Consultant Cardiologists and Senior CS we developed a rescheduling protocol and changes in practice (Fig 1). Routine follow-up, CS called patients after triaging to explain their new schedule and advised if attendance was needed. If a device check was required, RM was considered, discussed and sent out to the patient. The GDPR aspects were documented, and verbal consent was considered sufficient by the MDT. New implants, all patients received RM. Patients were educated and set up with RM prior to discharge. This, combined with automatic testing, facilitated a virtual 1-month review with wound photos being emailed or video consultations.
Results: On 16th March, 1-week pre-lockdown, the strategy was started. Over the last three months, approximately 5,130 face-to-face appointments were rescheduled, limiting face-to-face appointments to 5 per day, these were for wound reviews or programming changes.
Discussion:
Our successes: With these service changes, we have captured displaced leads earlier, expedited wound reviews and avoided unnecessary exposure to the virus for thousands of patients.
Due to reduced outpatient visits I was able to facilitate CS working from home, performing RM via VDI connections to hospital. This aided social distancing on site, resilience within staffing, and improved efficiency to combat the increased workload from our rescheduling protocol.
Our challenges: Implementing the rescheduling protocol with no admin support; the team had to balance this workload and the increased RM workload.
Contacting patients was a challenge. Often telephone calls were unanswered or the patient not available. This delayed the appointment change being relayed to the patient and had to be repeated. We were challenged with patients suffering mental health issues and anxiety, either brought on by the pandemic or exacerbated by it. Some patients refused to attend despite needing urgent box change and some safeguarding issues were raised.
A significant challenge pre-pandemic was the amount of disconnected home monitors. The team worked with industry providers to contact patients and support them to improve connectivity significantly.
Conclusion: At the onset of the pandemic the delivery of cardiac device management required fluidity, the team had to adapt quickly to changes in service delivery. With many challenges this has developed a new way of working for CS that can protect both patients and staff in the future.