The global prevalence of aortic stenosis (AS) has steadily increased over the past several decades.1 In high-income countries, degenerative calcific aortic valve disease is the primary aetiology for AS, whereas chronic rheumatic valve disease and infective endocarditis remain more common causes worldwide.2 Population-wide trends in developed countries suggest a strong relationship between advanced age and incidence of AS.3 Increased prevalence of atherosclerotic risk factors has also been attributed to the growing burden of AS.4 With the advent of novel strategies to treat this ageing population, aortic valve disease is expected to impact public health and healthcare resources further.
The severity of AS is commonly defined based on echocardiographic parameters. However, 5–10% of patients with severe AS do not meet the normal defining criteria.5 Patients with low-flow, low-gradient (LFLG) severe AS are a subset of this population who have severe valvular stenosis but do not meet the classical echocardiographic criteria due to their inability to eject sufficient flow across the aortic valve.
LFLG AS can be further categorized as classical in patients with low left ventricular (LV) ejection fraction (EF), or paradoxical in those with preserved LV function. Identifying these patients poses a unique clinical challenge and remains an important objective, as individuals with true severe AS derive long-term benefit from aortic valve replacement (AVR).
Defining the severity of aortic stenosis
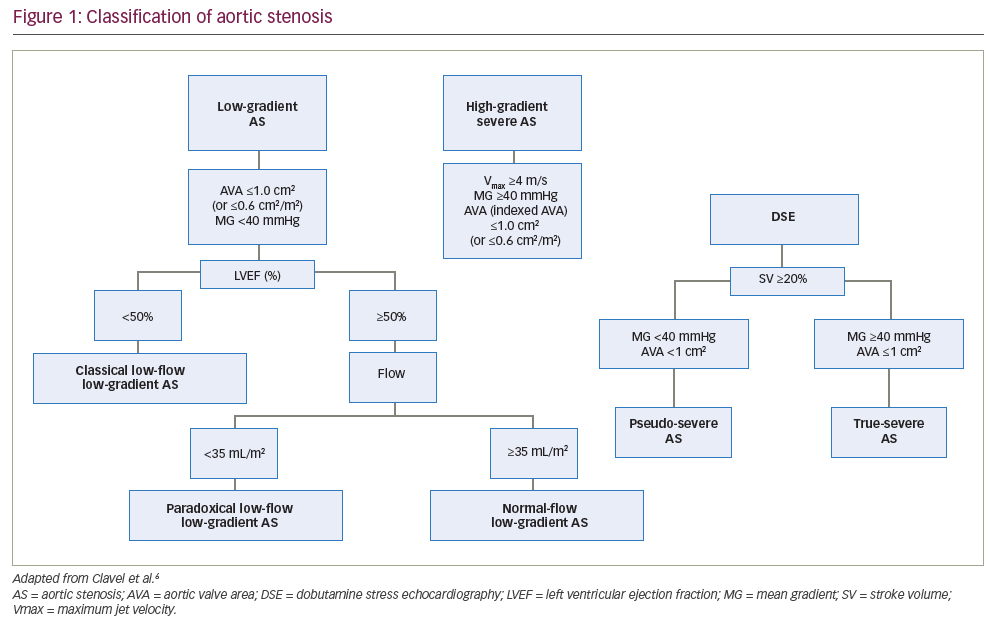
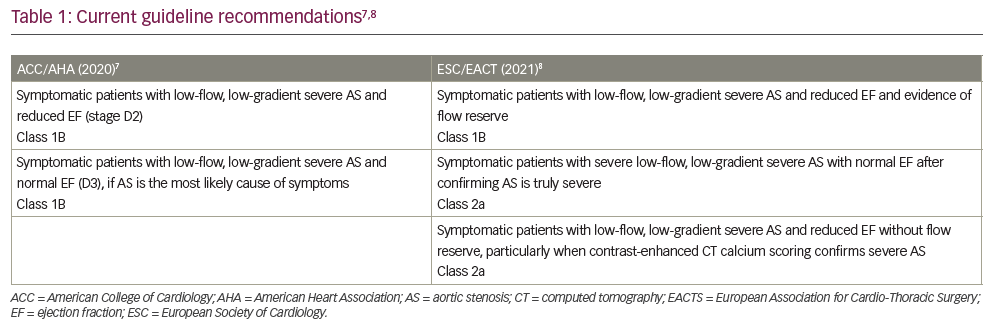
A maximum jet velocity (Vmax) of ≥4.0 m/s, mean gradient of ≥40 mmHg or calculated aortic valve area (AVA) of ≤1.0 cm2 on echocardiography suggest severe AS (Figure 1).6 Current guidelines recommend AVR for high-gradient severe AS in the setting of LV systolic dysfunction, clinical symptoms or in patients who are undergoing cardiac surgery for another indication (Table 1).7,8 In a low-flow state, discordance between the AVA and mean gradient can occur in up to 30% of patients in this subset, as the latter is highly flow dependent. This, in turn, poses clinical challenges to the assessment of stenosis severity and therapeutic decision-making.
When assessing this patient population subset, the echocardiographic measurements used to assess valve area and gradient should be reviewed for measurement errors. For instance, the mean gradient relies on the accurate alignment of the continuous-wave Doppler in the direction of the aortic valve jet. The AVA is derived from the continuity equation and is, therefore, not a direct measurement. This calculation, in turn, relies on an accurate measurement of the LV outflow tract (LVOT) diameter, LVOT time-velocity integral and aortic time-velocity integral. Furthermore, the equation assumes that the LVOT is spherical when it may be elliptical or eccentric. In addition, the LVOT measurement is dynamic and changes as a function of patient age. These limitations are important to recognize, as they can lead to an underestimation of the LVOT area by as much as 17%.9 Current guidelines recognize these technical challenges, which are reflected in the recommendations for ensuring accuracy and standardization.7,8
Classical low-flow, low-gradient aortic stenosis
Classical LFLG AS is defined as an AVA of ≤1 cm2, mean gradient of <40 mmHg, Vmax of <4.0 m/s and an LVEF of <50%.10 At the time of diagnosis, patients who fit this definition typically have larger LV and left atrial cavity sizes, higher LV mass index, higher estimated right ventricular systolic pressures, and greater severity of mitral and tricuspid valve regurgitation.10 The reduced systolic function may be secondary to an ischaemic/non-ischaemic cardiomyopathy, afterload mismatch from long-standing severe AS, or a combination of these conditions.11
The diagnostic assessment of these patients includes measures to rule out pseudo-severe AS. The low-flow state in pseudo-severe AS is attributed to underlying cardiomyopathy, which creates a false pattern that resembles the haemodynamic parameters of severe AS. This results in an overestimation of AS severity due to incomplete leaflet opening during systole.
Dobutamine stress echocardiography
Dobutamine stress echocardiography (DSE) can help identify patients with true LFLG AS and reduced systolic function. For instance, a significant increase in mean gradient to an absolute value of ≥40 mmHg indicates true severe AS.12 Alternatively, a persistently low mean gradient (<40 mmHg) despite a significant increase in stroke volume (≥20%) may suggest pseudo-severe AS. This test also identifies the presence of a flow reserve, which is defined as a relative increase in stroke volume of >20%.
The use of mean gradient at peak stress and AVA as predictors of outcomes is controversial. Annabi et al. found that the combination of peak stress mean gradient >40 mmHg and AVA <1 cm2 correctly classified AS severity in only 47% of patients.12
Peak stress mean gradient and AVA are highly dependent on the transvalvular flow response to dobutamine. Persistent discordance in AS severity based on peak mean gradient and AVA is likely explained by the inability to achieve normal flow during DSE. The use of projected AVA is useful, as it estimates valve area at a standardized flow rate (250 mL/s). One study suggested that projected AVA has greater accuracy than DSE measurements and is a better predictor of mortality in patients treated conservatively.13 Annabi et al. prospectively analysed DSE criteria in 186 patients with LFLG AS and reduced LV systolic function.14 The authors found that the sensitivity for the identification of true severe AS was higher with projected AVA (86%) than with standard DSE criteria (63%). Furthermore, low projected AVA was better at predicting 4-year mortality than higher projected AVA (adjusted hazard ratio [HR] 3.78, 95% confidence interval [CI] 1.90–7.50; p<0.0001).14 Sato et al. also demonstrated improved AVR survival outcomes in patients with true severe AS by projected AVA compared with standard echocardiographic criteria.15
The use of flow reserve also needs close examination. Earlier studies demonstrated that patients with flow reserve had relatively lower operative mortality, ranging between 5% and 7%.16 Further support for the use of flow reserve had been provided by an earlier French multicentre study, which demonstrated operative mortality of 32% for patients undergoing AVR in classical LFLG AS in the absence of flow reserve.17 This parameter, however, did not predict recovery of LVEF, improvement in functional class or long-term outcomes following surgical AVR (SAVR). More contemporary studies do not show an association between flow reserve and outcomes across treatment groups, whether the patient receives conservative therapy, transcatheter AVR (TAVR) or SAVR.14,18 This change may be explained by overall improved surgical outcomes, lower incidence of patient prosthesis mismatch and the introduction of TAVR as a less invasive therapeutic option.
Computed tomography
In some cases, discordant measurements on echocardiography can present diagnostic challenges. Computed tomography (CT) aortic valve calcium scoring has been shown to be a valuable complementary test for facilitating clinical decision-making. As such, its use is recommended in certain clinical scenarios.
The degree of aortic valve calcification (AVC) is a well-established predictor of death and adverse events in patients with AS regardless of haemodynamic severity.19 AVC can also be used to identify patients who are at risk of a rapid progression of AS. This test also has the added benefit of being independent of loading conditions and haemodynamic effects, which are often difficult to standardize.
There are, however, sex-related discrepancies between AVC and the severity of AS.20 This is partly explained by a higher fibrosis–calcium ratio in women compared with men. A similar trend has been identified in patients with bicuspid aortic valve. The 2020 guidelines from the American College of Cardiology and the American Heart Association suggest the sex-specific Agatston unit (AU) thresholds for the diagnosis of severe AS to be 1,300 for women and 2,000 for men.7
As CT AVC scoring cannot quantify the degree of fibrosis, there may be diagnostic challenges in patients with severe AS. A contrast-enhanced CT assessment of the aortic valve calcific and non-calcific volumes (i.e. fibrosis) has shown a correlation with AS severity and may be a useful diagnostic test in such patients when the usual measurements of severity are inconclusive.20 In a multicentre international registry, Pawade et al. demonstrated consistency and reproducibility for sex-specific CT AVC thresholds among patients with severe AS of varying demographics.21 A threshold of 1,377 AU for women and 2,062 AU for men assisted in the diagnosis of severe AS, particularly when other diagnostic tests and parameters were inconclusive. In addition, scores above these thresholds were a strong predictor of adverse clinical events among patients with discordant echocardiographic parameters. This study requires no contrast and low radiation exposure and, as such, should be ordered as the next test in such patients.
Paradoxical low-flow, low-gradient aortic stenosis
Paradoxical LFLG AS is defined as having an AVA of ≤1 cm2 (or indexed AVA <0.6 cm2/m2), mean gradient of <40 mmHg, stroke volume index (SVI) of <35 mL/m2 and LVEF of >50%.12 The low-flow state is attributed to impaired LV filling secondary to concentric remodelling and reduced systolic global longitudinal strain (GLS).12 The reduction in stroke volume has also been explained by factors that affect the loading conditions on the LV, such as atrial fibrillation, mitral regurgitation, tricuspid regurgitation or mitral stenosis.12
Independent markers of operative mortality include LV concentric remodelling/hypertrophy, moderate-to-severe diastolic dysfunction, decreased longitudinal strain and SVI. Many of these parameters improved following AVR, which may explain the improved survival rates in the long-term follow-up data compared with classical LFLG cohorts.12
Normal-flow, low-gradient aortic stenosis
Normal-flow, low-gradient (NFLG) AS is defined as an AVA of <1 cm2, mean gradient of <40 mmHg, SVI of >35 mL/m2 and LVEF of ≥50%. The presence of a low gradient despite a normal SVI poses unique challenges, as this pattern implies non-severe AS according to the guidelines.7,8 As such, many clinicians opt for conservative management.
The low gradient may also be explained by a lower transvalvular flow rate, which can occur in patients who are bradycardic and experience prolonged LV ejection time. Other factors that affect the gradient include uncontrolled systemic hypertension and reduced arterial compliance.22,23
A recent study suggested that this cohort represents up to 30% of all cases of severe AS with preserved LV function. These patients are predominantly older women with low body surface area.24 When compared with other forms of severe AS, data suggest that these patients do not have as significant concentric LV hypertrophy, left atrial dilation or impairment in systolic longitudinal function.24,25 This may suggest that the majority of these patients can be managed medically. Chadha et al. showed that patients with NFLG severe AS have comparable outcomes to patients with moderate AS both under medical and surgical management.26 AVR was, however, performed earlier in patients with NFLG severe AS, which suggests that this population subset needs close clinical follow-up.26
Aortic valve intervention
Patients with LFLG severe AS continue to have poor long-term survival when treated with optimal medical therapy alone. Aortic valve intervention can potentially improve the survival for these patients.15 Expert consultation is beneficial for identifying appropriate patients for valvular intervention. Once patients meet the indications for AVR, it is important to review all potential risks and benefits of therapeutic options with the Heart Team. While many studies have demonstrated improvements in morbidity and mortality with aortic valve intervention, it is important to note that patients with LFLG severe AS were largely excluded from landmark trials, which further adds to the complexity of managing these patients.
The use of a frailty index in addition to traditional scoring systems may improve clinical decision-making. Investigators for a single-centre study from Switzerland developed their own frailty index, which included an assessment of cognition, mobility, nutrition and basic activities of daily living.27 The investigators found improved prediction of 1-year mortality when their frailty index was combined with the Society of Thoracic Surgeons (STS) score or the European System for Cardiac Operative Risk Evaluation (EuroSCORE).27 Although frailty is an important consideration for the Heart Team, more validated scoring systems are needed to accurately predict outcomes for this high-risk group.
Preoperative risk assessment
An integrative model has been used when evaluating candidacy for SAVR. The STS risk score is a tool that calculates the impact of clinical risk factors on operative mortality. It has demonstrated good predictive value in assessing long-term outcomes following AVR and is used in large clinical trials, which helps standardize operative risk.27 Risk models, however, do not incorporate specific risk factors associated with poor outcomes in patients with LFLG severe AS. These include patients with very low preoperative gradients, absence of flow reserve and reduced GLS. As such, this subset of patients needs to be assessed beyond the use of classical risk stratification tools.
Independent clinical markers have been described in the literature and can help identify high-risk patients. For instance, GLS was shown to be associated with mortality in patients with low LV function (GLS <9%).28 Levy et al. published a large multicentre series in which operative risk was stratified, and observed a 10% decrease in perioperative mortality over a 15-year period.29 The authors identified predictors of outcomes, which included high EuroSCORE, low mean gradient, low EF, a New York Heart Association classification of class III, history of congestive heart failure and multi-vessel coronary artery disease.29
Aortic valve replacement versus medical therapy
Conservative management of patients with LFLG severe AS results in poor outcomes. Results from the post hoc analysis of the PARTNER trial (Placement of AoRTic TraNscathetER Valve Trial; ClinicalTrials.gov Identifier: NCT00530894) showed a 2-year mortality of 76% with medical management alone.30 In addition, there was a statistically significant benefit in mortality seen in patients who were deemed inoperable and were offered TAVR.30
Similarly, a meta-analysis from Dayan et al. demonstrated higher overall mortality in patients with paradoxical LFLG severe AS compared with patients with high-gradient severe AS who were conservatively managed (HR 1.67, 95% CI 1.16–2.39).31 In addition, mortality was reduced by 56% with AVR compared with conservative management (HR 0.44, 95% CI 0.25–0.77).31 These patients typically have more comorbidities and delayed referral for AVR assessment, which may contribute to the higher mortality rates.
Despite the observed benefit of AVR, the perioperative risk remains high, with a mortality risk of up to 22%.16–18,29 As such, selecting the most appropriate management strategy for this patient population can be challenging. Despite the poor prognosis, AVR is associated with an observed survival benefit compared with conservative management.17,32,33 This was further supported by a recent meta-analysis from Ueyama et al. demonstrating a significant decrease in all-cause mortality in patients receiving AVR (TAVR or SAVR) compared with those receiving conservative therapy.34 This was consistent among all subclasses of low gradient AS.34
Surgical versus transcatheter aortic valve replacement
Compared with LFLG AS, patients with high gradient severe AS have better outcomes following AVR. A recent meta-analysis by Osman et al. demonstrated better outcomes following TAVR in high-gradient AS versus LFLG AS, with less 30-day, mid-term all-cause, and cardiovascular mortality post implant (6.0% versus 7.5%, 21.0% versus 29.0%, and 12.6% versus 18.7%, respectively).35 Notably, there was a non-significant trend towards worse outcomes in patients with classical versus paradoxical LFLG AS. This would support prior studies demonstrating worse 30-day mortality in patients with reduced EF.29
Few studies have directly compared SAVR and TAVR. Ribeiro et al. conducted the first registry to assess outcomes in patients with classical LFLG AS following TAVR.36 The 30-day mortality rate following implant was 3.8%, which is lower than the conventional surgical risk score and comparable to other TAVR studies.36 There was, however, a high mortality rate at the 2-year follow-up (39.0%). The study investigators identified independent risk factors for poor outcomes, including lower haemoglobin level, chronic obstructive pulmonary disease, and moderate or severe residual aortic regurgitation.36
Annabi et al. found that early AVR (≤3 months) was associated with improved survival in both patients with classical and paradoxical LFLG severe AS when compared with conservative management or delayed AVR.37 When adjusted for patients’ baseline risk profile, there was a signal towards the superiority of transfemoral TAVR. A similar result was found in the post hoc analysis of the PARTNER trial, which found no difference between TAVR versus SAVR in this high-risk cohort.30 It is important to note that patients with no-flow reserve and very-low EF were excluded from the PARTNER-I trial.
Conclusions
LFLG severe AS represents a complex, heterogeneous subset of patients. Identifying these patients can be challenging, and different diagnostic tests may be required to confirm the diagnosis. Current data suggest that patients with those undergoing true aortic valve stenosis derive benefit from early intervention compared with conservative management. The Heart Team should provide a comprehensive preoperative risk assessment incorporating additional risk factors that are not reflected in standard risk tools. The decision to proceed with AVR should be individualized and aligned with patient preference. There are limited data to suggest a preference for SAVR versus TAVR, and, as such, future randomized controlled trials are needed.