Background: Atrial fibrillation termination to atrial tachycardia (AT) or atypical flutter (AFL) is increasingly common with ablation strategies targeting non-pulmonary vein drivers. These add a significant additional time and resource burden to procedural workflows. Currently, stable arrhythmia contact maps measure local activation times (LATs) across multiple cycles relative to a fiducial time reference. In order to collect a sufficient density of points for identification and ablation of these post-ablation ATs requires sequential localization of multi-electrode catheters to a zone of interest before interrupting the critical isthmus with ablation. We set out to demonstrate feasibility and efficiency of a novel mapping method that aligns multiple
non-contact (NC) catheter positions in stable arrhythmias.
Methods: In silico, a cellular automata model was used to simulate 10 cases of atrial tachycardias/flutters including contact (C) measurements from 1- and 16-pole catheters and NC measurements on a 48-pole NC catheter. NC and C measurements were simulated at 25 catheter positions, each measuring one cycle. In vivo NC and C measurements were also collected at multiple catheter positions in five PersAF patients who terminated via ablation to AT/AFL. All cycles were time aligned. A charge density inverse solution used accumulated NC CPs to create a series of multi-position NC LAT (MPNC-LAT) maps – each map used a larger number of CPs. Complementary sets of CLAT maps were also created. MPNC-LAT and C-LAT maps were compared using: Accuracy index = SA(1-LATerror/CL). LAT error was calculated as mean absolute error against the simulated LAT map (in silico)/final C-LAT map (in vivo).
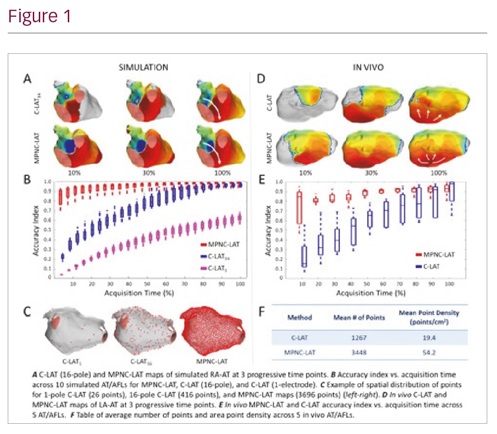
Results: As an overall cohort, MPNC-LAT method required 64% less time in silico (40% in vivo) than C-LAT to achieve AI of 0.9. MPNCLAT map has 7x denser points in silico (2–3x in vivo) compared to C-LAT (figure). MPNC electrograms compare favourably in morphology and timing to respective contact electrograms. In early preliminary data, these methods compare favourably to currently employed contact mapping algorithms using high definition catheters.
Conclusion: In this computational-clinical study, the MPNC-LAT method quickly produces ultra-high-density maps of in silico stable arrhythmias with high accuracy. This method allows more rapid mapping and treatment of stable atrial arrhythmias, particularly valuable at the end of a case where persistent AF terminates to AT/AFL. Preliminary data shows excellent performance when directly compared to contact mapping in patients brought to the electrophysiology laboratory with post-ablation atrial tachycardias and atypical flutters.