Introduction: Maintenance of sinus rhythm is challenging in patients with longstanding persistent atrial fibrillation (PeAF); outcomes from catheter ablation are suboptimal. We investigated whether combining minimally invasive surgical ablation with catheter ablation (‘Hybrid ablation’) improved outcomes versus catheter ablation alone.
Methods: Forty-three consecutive patients (mean age 68.6 ± 7.7 years, median LVEF 50%, mean left atrial diameter 47.4 ± 6.3 mm, mean 0.35 ± 0.48 previous catheter ablations) with longstanding PeAF (median duration 36 months) underwent subxiphoid endoscopic surgical ablation of the posterior left atrium followed by catheter ablation at a single UK centre from 2013–8. The primary outcome was AF-free survival at 12 months; secondary outcomes included change in EHRA class, procedural complications, echocardiographic data, freedom from anti-arrhythmic drugs (AADs) and long-term arrhythmia-free survival. Outcomes were compared with a propensity-matched group of 43 patients who underwent catheter ablation alone. Both groups underwent multiple catheter ablations as required.
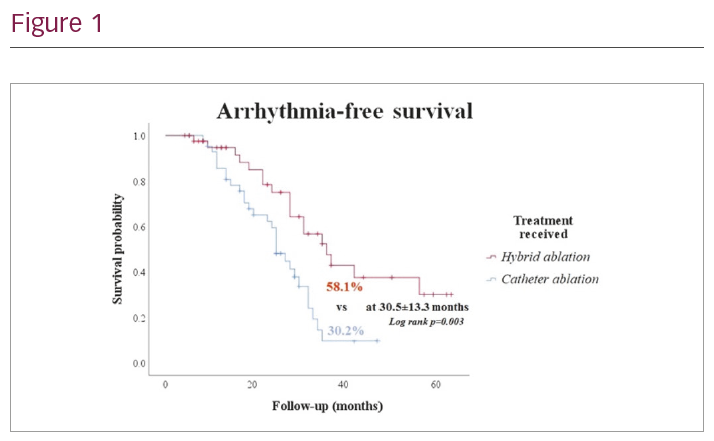
Results: Baseline characteristics were similar between groups. The Hybrid group underwent 43 surgical procedures and 60 catheter ablations, and the control group underwent 55 catheter ablations (103 versus 55 procedures, p<0.0001). Twelve months after a single procedure, hybrid ablation was associated with increased AF-free survival on AADs (60.5% versus 25.6%, p=0.002) and off AADs (37.2% versus 13.9%, p=0.025), when compared with catheter ablation. Allowing for multiple procedures, after 30.5 ± 13.3 months’ follow-up hybrid association was associated with increased arrhythmia-free survival on AADs (58.1% versus 30.2%, p=0.016) and off AADs (32.5% versus 11.6%, p=0.036) when compared with catheter ablation. EHRA class improved in the hybrid (2.59 ± 0.7 to 1.79 ± 1, p=0.0001) and control groups (2.7 ± 0.8 to 2.11 ± 0.93, p=0.01). There was a trend towards increased complications in the hybrid ablation group (11.6% versus 2.3%, p=0.2), which included two cardiac tamponades, one inferior vena cava perforation, one phrenic nerve palsy and one pericardial hernia in the hybrid group. Multivariate analysis identified only hybrid ablation (OR 3.06 (1.23–7.6), p=0.017) as predictive of arrhythmia-free survival long term.
Conclusions: In longstanding PeAF, hybrid surgical ablation is associated with improved arrhythmia-free survival versus catheter ablation alone. Complication rates are significant but have been shown to depreciate with experience.