Background: Patients with adult congenital heart disease (ACHD) are more prone to atrial arrhythmia, which increases their morbidity and mortality and risk of hospital admissions when compared with the same population where atrial arrhythmias are absent.
Objective: Compare the use of OCTARAY™ to PENTARAY™ for atrial tachycardia mapping in a patient with ACHD to understand the utility of this novel mapping catheter in mapping complex substrate.
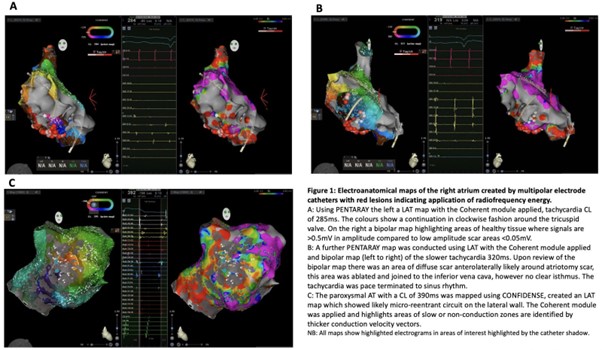
Methods: We describe the case of a 54-year-old female with tetralogy of Fallot, who underwent full surgical repair in 1972 with implantation of an endocardial pacemaker in 1997 for complete heart block. The patient was first reviewed in our emergency ACHD clinic following hospital admission with worsening symptoms associated with tachycardia. Device interrogation confirmed atrial tachycardia (AT) with a cycle length (CL) 280–285 ms. The patient was admitted for percutaneous catheter ablation in July 2020. A fixed curve decapolar catheter was placed in the right atrial appendage and entrainment confirmed cavotricuspid isthmus (CTI) dependent tachycardia CL 270 ms. Electroanatomical mapping was performed using CARTO and CONFIDENSE filtering with a PENTARAY catheter. Bipolar scar thresholds and noise level were set to 0.02 Mv. 6,374 points were collected over 16 minutes (Figure 1A). Radiofrequency (RF) ablation was performed between 30–40 W and slowed tachycardia to 320 ms, but did not terminate and therefore remapped. A low voltage region was identified anterolaterally likely involving atriotomy scar and 5,380 points were collected over 18 minutes (Figure 1B). This area was ablated and joined to the inferior vena cava. The patient remained arrhythmia-free until May 2022 with recurrence of paroxysmal AT, CL 380–400 ms. A delectable decapolar catheter was placed in the RAA and burst pacing induced tachycardia CL 380 ms. Activation mapping was performed using the OCTARAY catheter and CONFIDENSE filtering. Bipolar scar threshold and bipolar noise level set at 0.03 Mv and 0.02 Mv; 16,863 LAT points were collected in 12 minutes (Figure 1C). LAT and coherent maps highlighted a micro reentrant circuit on the lateral wall, at the atriotomy site with a potential gap in the intercaval line. RF ablation at 35 W in this area terminated tachycardia in 4 seconds. The patient remains arrhythmia-free 10 months later.
Results: Upon review of these two procedures, we saw reduced mapping time and greater point density with the Octaray mapping catheter. Another distinct benefit is the smaller electrode size and tighter spacing for better delineation of heterogeneous scar on bipolar maps. Moreover, the Octaray provided wide coverage of the enlarged atrial surface to help make immediate diagnoses of activation patterns and identification of critical isthmus, when placed at the area of interest. The Octaray catheter also allows the use of TRUEref, this technology uses a unipolar electrode to reduce the impact of far-field signals. Consequently, aiding the identification of gaps and improving the characterization of the lesion sets, homing in on the critical isthmus with less ablation necessary to terminate arrhythmia.
Conclusion: The OCTARAY™ catheter provides excellent signal quality and identification of critical isthmus with quick mapping time, making it an attractive option in the ACHD population where arrhythmias are often non-sustained or not tolerated. ❑
Figure 1: Electroanatomical maps of the right atrium created by multipolar electrode catheters with red lesions indicating application of radiofrequency energy