Background: During COVID-19, Royal Papworth Hospital (RPH) expanded remote follow-up (RFU) services for cardiac pacing device patients in line with recommendations by current guidelines. RFU allows for detection of adverse clinical events such as arrhythmias, battery depletion and lead damage via monitoring of associated parameters. Whilst RFU has not been shown to increase occurrence of major adverse events, it remains underutilised with contradictory literature around costs and changing workload. This project aimed to identify how RPH RFU provision changed due to COVID-19 and the impact on patients awaiting intervention.
Methods: A sample of 517 RPH device patients was retrospectively collected. Proportions of these patients on RFU were analysed, establishing proportions of those who were signed-on ‘pre-COVID’ and ‘during COVID’ (i.e. before or after 1 April 2020), and how proportions differed across device types (pacemakers, implanted cardioverter defibrillators [ICDs], and cardiac resynchronisation therapy [CRT] devices). A second sample of 180 patients who underwent elective unit replacement (EUR) intervention between 1 March 2019 – 30 April 2021 was collected. Proportions of these patients on RFU was analysed, and proportions of EUR indications identified by RFU or in-house were compared. Time from indication to intervention was compared between RFU and in-house as well as overall numbers of monitoring appointments during this time.
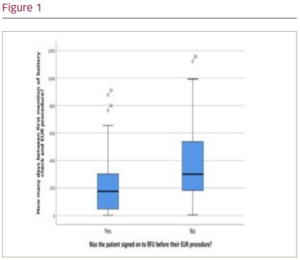
Results: From the first sample, 80% of patients overall were on RFU; 53% of patients were signed-on to RFU pre-COVID and 27% during COVID. However, when analysed by device type, there were significant differences both overall (p=0.000) and by pairwise comparison: pacemaker patients had lowest overall RFU sign-up, despite seeing the largest sign-on increase during COVID (p=0.000), and more CRTs than ICDs were signed-on during COVID (p=0.001). Analysis of the intervention patient sample highlighted that RFU significantly reduced the time from indication to EUR intervention (mean wait times: RFU=176 days, in-house=300 days; p=0.000). However, RFU did increase the mean number of monitoring appointments compared with in-house only follow-up (RFU=4, in-house only=3; p=0.044). Of the patients on RFU in this population, there was no difference in the number of first indications identified by RFU or in-house appointment.
Conclusions: Although RPH RFU services expanded during COVID-19, expansion was not equal across device types. For intervention patients, RFU significantly reduced the time from indication to EUR intervention, though monitoring workloads increased during this time. Future research may focus on alternative interventions to assess the impact of RFU in other device patient populations.