Introduction: Radiofrequency catheter ablation (RFA) is 1st line treatment in symptomatic adult patients with Wolff–Parkinson–White syndrome (WPW). Patients with WPW are often quoted a high success rate for RFA but does this reflect reality? There is a paucity of recent literature, and ongoing service developments in the UK may have affect outcome. Recent significant expansion of departments in the UK means individual operator experience of such cases is reduced. On the other hand, technological developments (such as 3D mapping, steerable sheaths, etc.) may have a positive impact on success rates. We retrospectively assessed the outcome of catheter ablation of WPW at a large UK tertiary cardiology centre over a 13-year period to determine if success rates in this ‘real-life’ setting were in keeping with the reported literature, and if they had changed over time.
Methods: We collected data on all patients with WPW scheduled for first time RFA between January 2006 and December 2018. All patients undergoing re-do RFA during this time were excluded. For comparison, we divided this time frame into three periods: 2006–2009, 2010–2013 and 2014–2018.
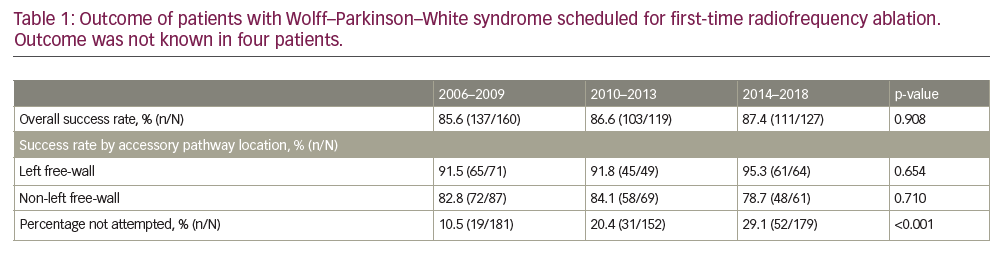
Results: Of the 512 patients, the mean age was 38.6 years and 59.1% (243/512) of patients were male. The outcome of patients undergoing RFA is listed in the Table 1. The number of patients scheduled for RFA remained relatively constant; the number of patients scheduled per consultant reduced. The overall success rate was 86.5% and this figure remained constant throughout the 13-year period. The most common accessory pathway location was left free-wall (LFW) pathway, accounting for 44.9% (184/410) of all pathways ablated. The success rate is significantly higher for LFW pathways compared to non-LFW pathways. Significant complications occurred in 1.17% of cases. 19.9% of patients scheduled for an ablation had no ablation attempted for various reasons (‘safe’ pathway, proximity to AV node, etc.). There was a significant increase in percentage of cases where ablation was not attempted over the period (p<0.001).
Discussions and conclusions: The number of adult cases of WPW scheduled for RFA year-on-year remains constant. The complication rate is in line with published literature. The RFA success rate is lower than that reported in an Isareli study (p<0.001). When divided by pathway location, the success rate of LFW pathways is not significant different from that reported (p=0.061), whereas that of non-LFW pathways is significant lower (p<0.001). This could potentially be explained by the lack of availability of 3D mapping for routine cases at our centre. 3D mapping was previously only used in complex, re-do ablations. With our findings, it has been decided that 3D mapping will become routinely available for patients with WPW undergoing RFA at our centre. Further, 1 in 5 cases scheduled for ablation did not proceed to ablation. This highlights an area where realistic expectation setting for patients is needed.







