Introduction: Increasing numbers of patients receive implantable cardiac devices capable of home monitoring (HM). Whilst providing many advantages, HM can create an overwhelming data burden with a low signal to noise ratio. This has a significant impact on cardiac physiologists’ work patterns. The aim of this work was to assess the volume and causes of unscheduled HM downloads and the frequency with which these resulted in a change in patient management. We also compared Medtronic and Biotronik downloads.
Method: HM alerts for all devices were set up according to default manufacturer recommendations. All unscheduled downloads between 9/8/2021 and 13/8/2021 from cardiac pacemakers (PPM), implantable cardioverter defibrillators (ICD), cardiac resynchronization therapy defibrillators and pacemakers (CRTD and CRTP) were retrospectively reviewed. Data recorded were manufacturer, device type, primary reason for alert, whether data required escalation to a physician or changed clinical management. Queen Alexandra Hospital Portsmouth is a large district general hospital with approximately 4,000 patients on HM, 70% of which are PPMs and 30% ICD/CRT devices.
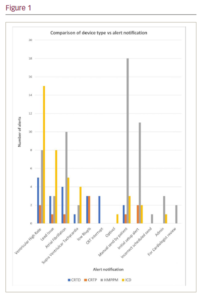
Results: A total of 122 unscheduled HM alerts were reviewed: 56 from PPMs, 39 from ICDs, 17 from CRTDs and 10 from CRTPs. Of the Medtronic downloads, 42% were manual patient sends, predominantly from PPM devices. A high volume of ventricular high rate (VHR) episodes and potential lead issues were seen from ICDs (Figure 1). ICD devices accounted for 10% of patients with HM but 32% of downloads. ICD downloads produced 50% of the total VHR alerts and 53% of total potential lead issues. Of the unscheduled alerts received, 54% came from Biotronik devices despite Biotronik devices only accounting for 16.5% of the total HM population. Furthermore, 80% of VHR and potential lead issue alerts were from Biotronik devices. Only two (1.6%) of the unscheduled alerts were escalated to a physician. Clinical management was not changed in a single patient.
Conclusions: Unscheduled downloads generate a significant volume of work for pacing clinics which needs to be taken into account when planning services. Although HM will occasionally pick up clinically important events, such as arrhythmias, the signal to noise ratio appears to be very low. In this sample, minimal physician input was needed and zero changes to patient management resulted from >100 HM alerts. This suggests that the thresholds for sending alerts are set too low. Furthermore, HM alerts from Biotronik and ICD devices were disproportionately high. Newer advances with Medtronic HM monitors and the phone app will help to reduce the burden of unscheduled downloads sent manually by patients. Patient education is a possible short-term interim solution. Collaborative working between centres following up cardiac devices and manufacturers to create bespoke HM templates for different patient groups, in particular ICDs, could be beneficial. Reviewing and implementing appropriate templates should be considered by all pacing clinics. Validated national standards and guidelines would facilitate effective use of HM while maintaining patient safety. ❑