Background: On the 23rd March 2020 the UK went into lockdown due to COVID-19 with vulnerable patients advised to shield at home. Patients with implantable devices still required battery changes and other interventions during this period, both clinically urgent and routine. A new strategy for identifying those needing urgent procedures was introduced at a tertiary cardiac centre to balance the risks of delaying procedures vs coming out of shielding.
Method: In normal circumstances, we perform 20-30 device re-intervention procedures per month including box changes, lead revisions, device upgrades and wound revisions. Patients are referred via device clinic or directly by a Consultant. Routinely we aim to box change patients at the time elective replacement indicator (ERI) is triggered. Most elective work was cancelled and patients requiring procedures were identified and booked in first. Working closely with Electrophysiology (EP) Consultants we developed new groups to sort patients (Table 1). An earlier referral threshold of 6 months till ERI was set to plan procedures in advance. Legacy device patients were sent remote monitors (RM) to maintain safety and delay procedures. Regular downloads for patients approaching ERI allowed them to isolate as long as possible.
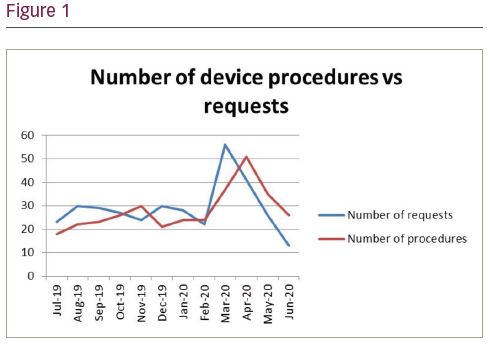
Results: During the months of March-May 2020 the number of requests increased from 25 to 56 requests (Figure 1). A peak in April 2020 of 50 device re-intervention procedures. Five patients hit ERI and had to be upgraded from Urgent to Very Urgent. Three of these had been delayed due to patient/family preference. One Fortify advisory had to be admitted due to prematurely triggering ERI. Three patients had their procedures done locally instead. Ten further patients have been referred for re-intervention locally. Three patients died on the waiting list, all sadly due to contracting COVID-19 in community. Two patients required input from the trust’s safeguarding team due to lack of contact with patient at predicted ERI and non-compliance with RM. From Jan-July 2020 the average referral to treatment time (RTTT) constantly averaged at 50 days.
Discussion: Adaptations to this service involved multiple teams working together to maintain patient safety. This involved scheduling, pre admissions and Cardiac Scientists. We also transitioned to a Cardiac Scientist led service empowering the team to risk stratify patients.
A further challenge presented itself: a subgroup of patients declined procedures. We compromised with some patients; three patients had procedures at a local centre to avoid travelling into London. Linked trusts referrals to our centre increased during this period, likely due similar measures of lowering thresholds. Linked trusts did not have access to RM, requiring them to directly refer for box changes rather than having the luxury of delaying procedures. Some legacy patients had devices that were incompatible with RM or declined a RM. Since lowering the referral threshold, a rise in referrals was expected, however, the results suggest that a back log of referrals, as the RTTT was indifferent. Collaborating with colleagues internally, local centres and enrolling on RM maintained shielding and device safety towards end of battery. This exemplifies solidarity across cardiac services during the COVID pandemic.