Introduction: Complex device therapy (CDT) [cardiac resynchronisation therapy pacemaker or defibrillator (CRTP or CRTD) and implantable cardioverter defibrillator (ICD)], is recommended in patients with heart failure (HF) with severe left ventricular systolic dysfunction if they are still symptomatic despite optimisation HF medication. Several patients however, will only tolerate optimal doses of these drugs after CDT, the latter protecting them from significant bradycardia or improving renal and haemodynamic function. Furthermore, post-implant follow up of CDT patients is variable in our centre, with patchy clinician review and technical follow up in the General Pacing Clinic (GPC) without the necessary time and technical expertise to optimise device function.
Methods: We set up a HF-Device clinic staffed by a HF nurse and a highly skilled pacing physiologist, supervised by a Consultant Cardiologist. The aims were to optimise device programming for HF symptoms and battery longevity; optimise HF medication and overall care; ensure community HF nurse care where appropriate; identify clinical issues such as occurrence of new atrial fibrillation (AF). Patients were invited to attend in person, although some opted for telephone appointments. If they did not attend, their remote CDT downloads were analysed and recommendations made for further optimisation of their HF care. Patient demographics, device and clinical findings, and device and clinical interventions were documented.
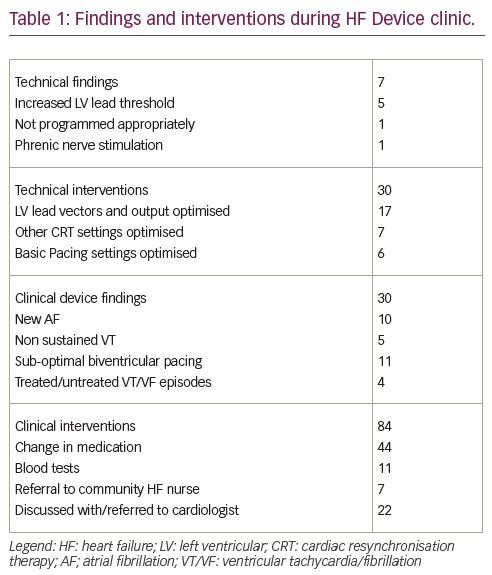
Results: Between 7th July 2020 and 6th April 2021, 65 clinic visits occurred involving 57 patients [mean age 73, ± 11.56 years; range 28-90); 40 (71%) male; 19(34%) ischaemic cardiomyopathy; 23 (41%) dilated cardiomyopathy; 15 (20%). Other cardiomyopathy; 28 [(50%) had AF]. Of the 65 clinic visits, 7 (11%) were for ICD; 33 (51%) for CRTD and 25 (38%) for CRTP; 47 (72%) were in-house and 18 (28%) were remote appointments. Sources of referral included 43 (77%) 6-week post implant checks, 6 (11%) 3-month post implant checks; 4 (7%) from GPC, and 3 (5%) from consultants. 16 (25%) visits were scheduled due to ongoing technical or clinical issues. Table 1 shows a summary of the technical and clinical findings and respective interventions.
Conclusion: During the course of 65 clinic visits, the HF-Device clinic identified a total of 37 technical and clinical abnormalities. 30 technical device interventions and 84 clinical interventions took place to address these, as well as to optimise patients’ clinical status and device settings. The HF-Device clinic has enabled us to strengthen and standardise the management of our HF device patients following CDT.