Introduction: Catheter ablation is an effective first-line treatment for cavotricuspid isthmus (CTI) dependent atrial flutter (AFL). Conventional fluoroscopic (FLUO) method may involve significant radiation dose with bidirectional CTI block requiring extensive ablation. Contact force (CF) guided ablation has shown reduced fluoroscopy time, but no other differences. Local impedance (LI) technology has not previously been evaluated within the human right atrium. LI is a measure of catheter-tissue coupling, and significant LI reduction is predictive of lesion transmurality.
Methods: We conducted a preliminary prospective observational study in 17 patients undergoing first-time ablation for CTI-dependent AFL. Five patients underwent conventional, five CF-guided (CARTO, Biosense
Webster) and seven LI-guided (Rhythmia, Boston Scientific) ablation. All techniques used irrigated radiofrequency ablation with powers of 45–50 W. FLUO was guided by electrogram attenuation and generator
impedance drop with lesion duration of 30–60 s, CF was guided by force time integral or ablation index, LI was guided by local impedance drop. Measured outcomes included total ablation time, time from first ablation
to bidirectional block, number of lesions required to achieve block and mean local impedance drop (for the LI group). In the LI/Rhythmia group, if block was not achieved following the initial ablation line, ultra-high-resolution mapping was used to localise sites of breakthrough to identify ablation targets.
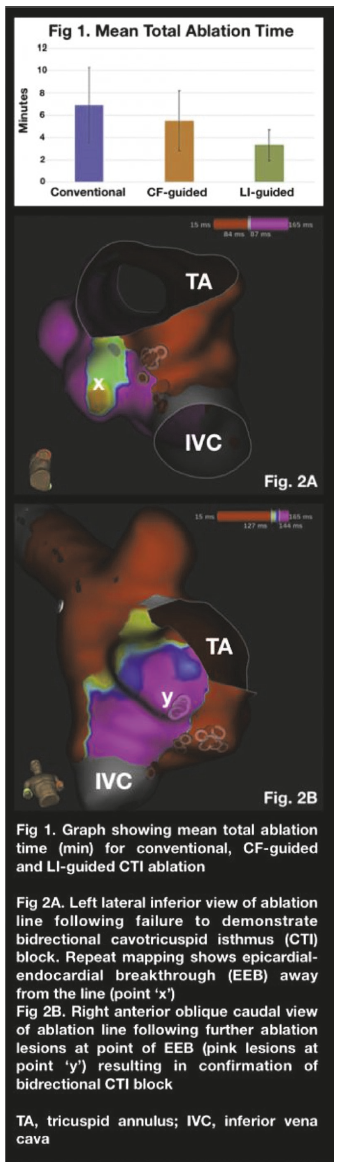
Results: There was 100% acute procedural success in all groups, and no major complications. Mean total ablation time was 6.9 minutes (± 3.4 m), 5.5 m (± 2.7 m) and 3.3 m (± 1.4 m) in the FLUO, CF and LI groups
respectively (Figure 1). The mean time from first ablation to confirmation of bidirectional CTI block was 27.7 m (± 16.1 m), 17.2 m (± 24.5 m) and 14.4 m (± 8.8 m) respectively. The total number of ablation lesions was 9 (± 3.39), 8.8 (± 6.14) and 7.9 (± 2.9).
The mean impedance drop in the LI cohort was 22.6 ohms (± 8.7 ohms). Of the seven patients, three failed to demonstrate bidirectional block at the first attempt and mapping identified breakthrough across the line in
two, and an epicardial-endocardial breakthrough (EEB) away from the line in the other (Figure 2). Block was achieved by further ablation at these points.
Discussion: In this preliminary study a number of trends are evident. LI-guided ablation reduced mean total ablation time versus FLUO and CF groups by 49% and 36% respectively, with 41% reduction in mean time from first ablation lesion to block compared with the FLUO, though similar to the CF-guided approach (6% reduction).
Further ultra-high-density mapping in three LI patients without block showed breakthrough, which rapidly identified targets for ablation. EEB was seen in one patient some distance from the line; this may have resulted in
treatment failure or prolonged ablation times without utilising mapping. The number of lesions required to achieve block was similar for all groups. This suggests that ablation delivery guided by LI change during lesion formation shortens the required duration of each lesion.
Conclusion: LI-guided ablation offers quick and effective ablation for CTI dependent AFL, and within our study has shown favourable metrics as compared with conventional and CF-guided ablation. A larger randomised
study is needed to determine statistically significant differences between the three approaches.