Background: Internal cardioverter defibrillator (ICD) and cardiac resynchronisation defibrillator (CRTD) implantation rates have increased significantly. As these escalate, and patient survival improves, so has the need for generator change (GC), which carries important inherent risk.
Objective: To assess the effect of GC on mortality in patients with ICD and CRTD.
Methods: Consecutive patients implanted in a single centre between January 2007 and September 2017 with an ICD or CRTD were included. Data was retrospectively collated from electronic records. Patients were divided into no generator change (NGC) and ≥1 generator change (GC+) groups. Overall mortality between groups, device type and reasons for GC were assessed.
Results: 746 patients with a median age 73 (63–81) and follow up 77 months (58–98) were included. GC+ included 330 patients.
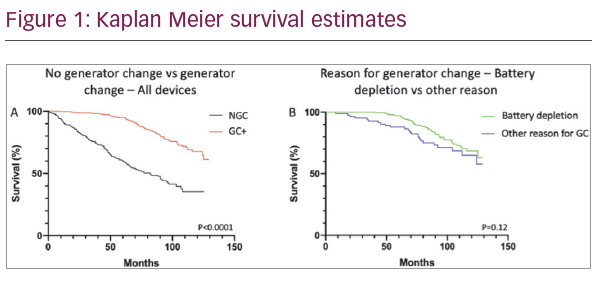
No differences in age, sex, ejection fraction, disease aetiology, NYHA class between groups were seen. CRTD numbers (39% versus 57%, p<0.0001) and pacing dependency (15% versus 2%, p<0.0001) was greater in GC+. GC Indications included; battery depletion 75%, upgrade 15%, infection 2% and recall 1%. GC+ survival was better (HR 0.28 CI 0.22–0.36, p<0.0001) (Figure 1A), regardless of device (ICD; HR 0.22 95% CI 0.15–0.31 p<0.0001, CRTD; HR 0.27 95% CI 0.19–0.39, p <0.0001). Within GC+ group a trend towards improved mortality in those with battery depletion was seen however, overall there was no difference (HR 0.69, 95% CI 0.4–1.2, p=0.12) (Figure 1B).
Conclusion: Patients undergoing GC have higher survival estimates regardless of device implanted. GC for reasons other than battery depletion may confer a worse outcome initially but over time this difference diminishes.
A) comparison between patients who undergo generator change and those who do not. B) A comparison of those who undergo generator change for battery depletion and those who undergo for alternative reasons. Key: NGC (no generator change)., GC+ >1 generator change, CG generator change.