Background: Cath lab time allocation for patients with suspicion of supraventricular tachycardia (SVT) is a challenging task. In this study, we aimed to identify the predictors of a negative electrophysiology study (EPS) in order to help optimizing booking times.
Methods: We retrospectively included 282 patients booked for SVT ablation with a 2-hour slot at the Royal Papworth Hospital between January 2018 and January 2019. Patients with pre-excitation, prior positive EPS or SVT ablation were excluded. Symptoms, demographics and other data were collected retrospectively from the electronic medical records. Patients were classified in those requiring SVT ablation and those with a negative EPS not requiring intraprocedural SVT ablation which only required half of the booked time. Failure at 3 months was defined as booking for an SVT re-do ablation or EPS for SVT.
Results: 282 patients between 16 and 88 years old (average 51) were included. One-hundred-and-sixty-five (58.5%) were female.
One-hundred-and-ninety-three (68.4%) patients had a positive study for AVNRT, 30 for AVRT (10.6%). SVT ablation was performed in 223 (79.1%) patients. Overall ablation success was 97.3% (217/223), 98.5% (190/193) for AVNRT and 90% (27/30) for AVRT. One-hundred-and-sixty-seven Patients required further follow up, of these 89.7% (130/145) of AVNRT and 90.9% (20/22) AVRT ablations continued to be successful on follow up at 3 months.
Documented narrow complex tachycardia and previous use of adenosine are strongly associated with requiring SVT ablation when undergoing EP studies (F 15.4 p 0.00 when combined with t 4.77 p 0.00 and t 1.857 p 0.06 respectively). The former remains statistically significant when adjusted for all the variables in Table 1 (t 4.61 p 0.00). Chest palpitations become a statistically significant predictor (t 2.36 p 0.02) in the multivariate analysis.
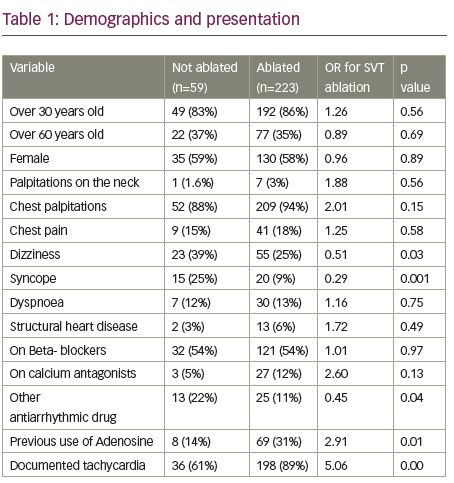
The use of antiarrhythmic drugs other than beta-blockers and calcium channel antagonists, prior syncopal episodes and dizziness seem to negatively predict the need of booking that extra time for intra-procedural SVT ablation (F 6.772 p0.00, t-3.094 p 0.002, t 2.331 – p 0.02 and t-1.834 p0.07). These first two associations remained statistically significant when adjusted for the rest of variables (t –2.29 p 0.02 and t –2.55 p 0.01 respectively).
Conclusion: Up to 21% of the patients with suspicion of SVT had a negative EPS result and did not require additional cath lab time for intraprocedural ablation. The immediate success rates were 98.5% for AVNRT ablation and 90% for AVRT ablation. The variables that predicted the need for SVT ablation were documented narrow complex tachycardia and previous use of adenosine. Syncope and use of other antiarrhythmic drugs other than beta-blockers and calcium channel antagonist were strongly associated with a negative EPS.







