Background: Identifying ”high-utilisers” of health care services and developing interventions that improve their outcomes and reduce costs is a priority for any health care system. The Canadian Institutes of Health Information (CIHI) recently identified a dynamic cohort of high-utilisers, defined as patients who accounted for the top 10% of acute care costs in Canada.
Objectives: To compare the demographic, clinical, and health care use of all comers with syncope with those of syncope patients identified in the high-utilisers cohort.
Methods: All patients aged ≥20 years presenting to an emergency department (ED) or were hospitalised with syncope (ICD10 code R55 in any diagnosis field) in the province of Alberta, Canada between 2011 and 2015 were included in the study (population cohort). A second group, consisting of a subset of syncope patients in Alberta who met the CIHI criteria for high-utilisers of health care resources was identified (high-users). The Elixhauser comorbidity score was calculated to assess the comorbidity burden.
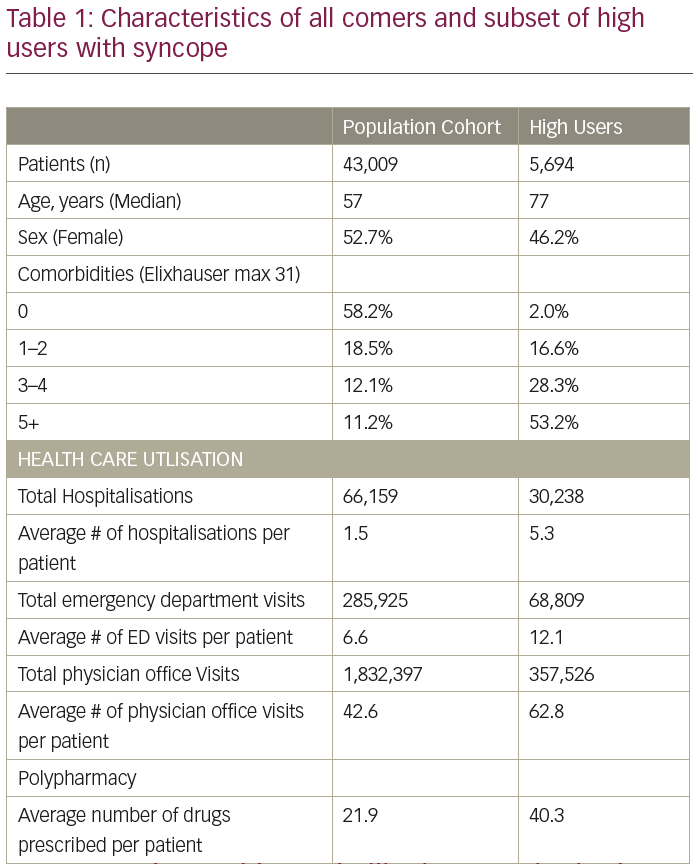
Results: Of 77,704 adult patients who met the CIHI definition for high utilisers, 5,694 (7.3%) had syncope. This high-users group accounted for 13.2% of all syncope patients in the province (population cohort, n=43,009). Compared to the population cohort, patients in the high-users group were significantly older and more likely to be men (Table 1). While the majority of the Population Cohort had no comorbidity (58.2%), 53.2% of the Higher Users group had more than five comorbidities. With respect to healthcare use, the High Users cohort represented 50% of all hospitalisations, 25% of all ED visits and 20% of physician office visits among syncope patients. The use of polypharmacy was also significantly higher among syncope patients in the high-users group.
Conclusion: In this population-based study, we found that a small fraction of syncope patients account for a disproportionately large proportion of health care resources. Multi-morbidity in syncope patients appears to be a major driver of costs and health care resource use.