Background: Some studies have shown that pre-implantation QRS area (QRSarea) predicts clinical outcomes after cardiac resynchronisation therapy (CRT).
Objective: To determine whether post-implantation changes in QRSarea predicts clinical outcomes after CRT.
Methods: In this retrospective study, QRSarea, derived from pre- and post-implantation vectorcardiography (VCG), were assessed in relation to the primary endpoint of cardiac mortality after CRT. Other endpoints included total mortality, total mortality or heart failure (HF) hospitalisation and total mortality or major adverse cardiac events (MACE).
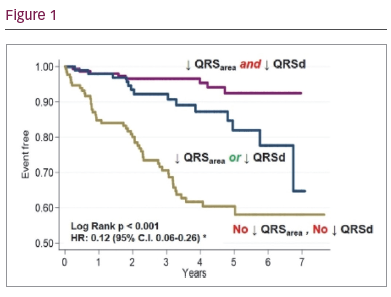
Results: In patients (n=380, age 72.0 ± 12.4 years, 68.7% male) undergoing CRT over 7.7 years (median follow-up: 3.8 years [interquartile range 2.3–5.3]), pre-implantation QRSarea ≥ 102 µVs predicted cardiac mortality (HR: 0.36; p < 0.001) as well as total mortality (0.58; p=0.001), total mortality or HF hospitalisation (HR: 0.53) and total mortality or MACE (HR: 0.52) (both p < 0.001). The association of QRSarea with cardiac mortality was independent of known confounders, including QRS duration (QRSd) and morphology (p<0.001). After CRT, a reduction in QRSarea ≥ 45 µVs or any reduction in QRSd predicted cardiac mortality (area under curve: 0.74 and 0.72, respectively; p = 0.425 for comparison). Concomitant reductions in QRSarea and QRSd were the best predictor of cardiac mortality (HR: 0.12; p <0.001 for interaction).
Conclusion: Pre-implantation QRSarea, derived from VCG, was superior to QRSd and LBBB in predicting cardiac mortality after CRT. A post-implant reduction in both QRSarea and QRSd was associated with the best outcomes.