Introduction: Temporary cardiac pacing is commonly required following cardiac surgery. Suboptimal programming of temporary pacemakers is associated with an increased risk of atrial and ventricular arrhythmia, reduced cardiac output and prolonged Critical Care Unit stay. Our centre has not hitherto had a standard operating policy (SOP) for temporary pacing post-cardiac surgery. This audit was undertaken to assess current practice in order to inform the development of an SOP and training programme.
Methods: Post-surgical patients admitted to Critical Care with active epicardial temporary pacing were enrolled systematically between January and May 2019. Patients with temporary pacing turned off or alternative methods of pacing were excluded. Device parameters were grouped into four categories: atrial lead assessment, ventricular lead assessment, assessment of mode and other, with the number of patients and changes required for each category being recorded. Appropriateness of programming was defined as applying a twofold safety margin for both output and sensitivity thresholds. Mode selection was assessed in accordance to the 2013 European Society of Cardiology (ESC) guidelines on cardiac pacing. Any safety concerns regarding inappropriate setup of the temporary pacemaker were escalated appropriately and recorded in the patients’ notes.
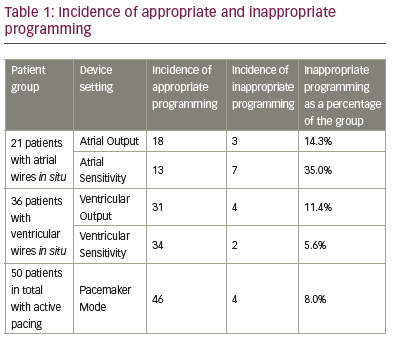
Results: Fifty patients were included in the audit (70% male, age 69.5 ± 12.3 years). Five (10%) patients had documented proof of daily device checks having been performed. The remaining 45 had programmed settings recorded but lacked evidence of daily checks. Nineteen (38%) patients required at least one element of programming to be changed, 3 of whom required more than one. Of the 22 patients with atrial wires in situ, eight (38.1%) required an increase in output, sensitivity or both (1, 5 and 2 patients respectively). One patient did not have underlying P wave thus sensitivity could not be assessed. Of the 37 patients who had a ventricular wire in situ, 5 (13.9%) required an increase in output, sensitivity or both (3, 1 and 1 respectively). One patient became hemodynamically unstable and therefore threshold could not be obtained. Of the 50 patients reviewed, a change of pacemaker mode was required in 4 patients (8%) and the battery replaced in 2 (4%). The frequency of errors in programming is shown in Table 1.
Conclusion/implications: The preliminary results of this ongoing audit suggest that the management of post-surgical patients with epicardial pacing in situ is suboptimal. In a centre without a physiologist-led temporary pacing service, increased education of the technical aspects of temporary pacing for existing ITU medical/nursing staff may be of benefit. Further research is planned to assess the impact of such an educational program and its impact on patient outcomes.