Background: Catheter ablation of atrial arrhythmias in patients with congenital heart disease present significant challenges. Advances in electroanatomical mapping advocate an anatomical approach for ablation with linear lesions to connect low-voltage areas or annuli. However, long linear lesions with prolonged energy applications might be unnecessary or even proarrhythmic. We report our experience of the Rhythmia mapping system in the ablation of complex atrial arrhythmias using a minimal lesion set as defined by a combination of anatomical and electrophysiological techniques.
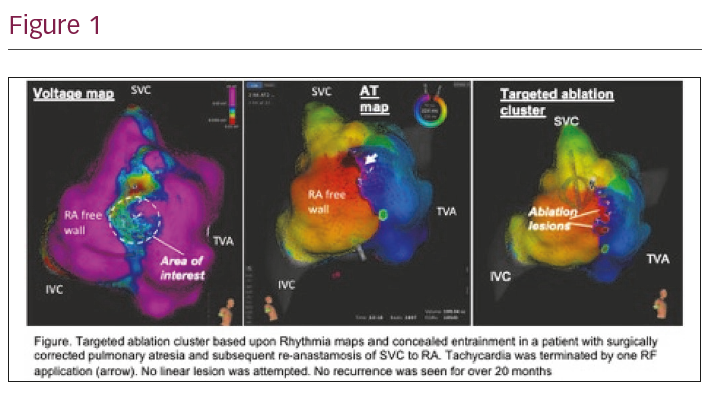
Methods: TACT Methodology: An Orion and a duodecapolar linear mapping catheter were inserted into the chamber of interest. Overdrive pacing was performed for entrainment of all sustained regular tachycardias at a site of the narrowest and slowest conduction of the circuit as determined by activation and voltage maps. Focal or small cluster lesions with irrigated RF were performed at the presumed protected isthmus or focus during tachycardia (Figure 1). Empirical linear lesions were avoided except for ablation of the cavotricuspid isthmus (CTI) or unmappable tachycardias. Lesions were not further extended after reaching the endpoints of bidirectional block with differential pacing across a re-entry isthmus or noninduciblity of a focal tachycardia.
Results: From September 2016 to April 2019, a total of 64 atrial tachycardias were ablated in 43 procedures for 37 consecutive congenital patients using this technique guided by the Rhythmia mapping system in our centre. Eighteen, 19 and 6 procedures were performed for severe, moderate and mild forms (2014 PACES/HRS classification) of congenital heart disease respectively. After a mean follow up of 15 (1–31) months, 32 (86%) patients were free of symptoms or documented tachycardia with a further 2 (5%) patients with a significant reduction in symptom burden. Single procedure success rate for any ablated arrhythmia was 90%. Six patients required repeat procedures. 22 (34%) of all tachycardias were CTI dependent. In 20/42 (48%) non-CTI tachycardias, the presence of narrow protected isthmus or focal source was demonstrated to be the mechanism as evident by tachycardia termination with 1–2 RF applications and/or localised catheter contact at the successful ablation site. The median RF ablation time for all cases was 6.7 (2–35) mins.
Conclusions: High density mapping with the Rhythmia system accurately defined highly localised, mechanistically critical, ablation targets in this large cohort of congenital atrial arrhythmias. For non-CTI tachycardias, the TACT approach to ablation lesions with limited energy applications can achieve favourable long-term success without the need for empirical anatomical lines.