Background: Cardiac fibrosis detected on late gadolinium enhancement (LGE) cardiovascular magnetic resonance (CMR) is associated with increased risk of ventricular arrhythmia and heart failure hospitalisation in ischaemic and non-ischaemic cardiomyopathy. Whilst left ventricular (LV) dysfunction is common in patients with pacemakers, the prevalence of cardiac fibrosis in this population has not been previously studied. The study aimed to evaluate the prevalence and location of cardiac fibrosis in patients with atrioventricular (AV) block undergoing pacemaker implantation.
Methods: Sixty-one patients with documented AV block due for pacemaker implantation and without a pre-existing clinical diagnosis of heart failure underwent CMR. The scan protocol included a short axis ventricular volume stack and LGE imaging. Volumetric and LGE quantification analysis (full width at half-maximum method) was performed using commercial software (CVI42, Circle Cardiovascular Imaging, Calgary, AB, Canada). The distribution of LGE was classified as being either and infarct (subendocardial) or non-infarct (midwall or subepicardial) pattern. The location of LGE was recorded according to the American Heart Association (AHA) 16 segment model.
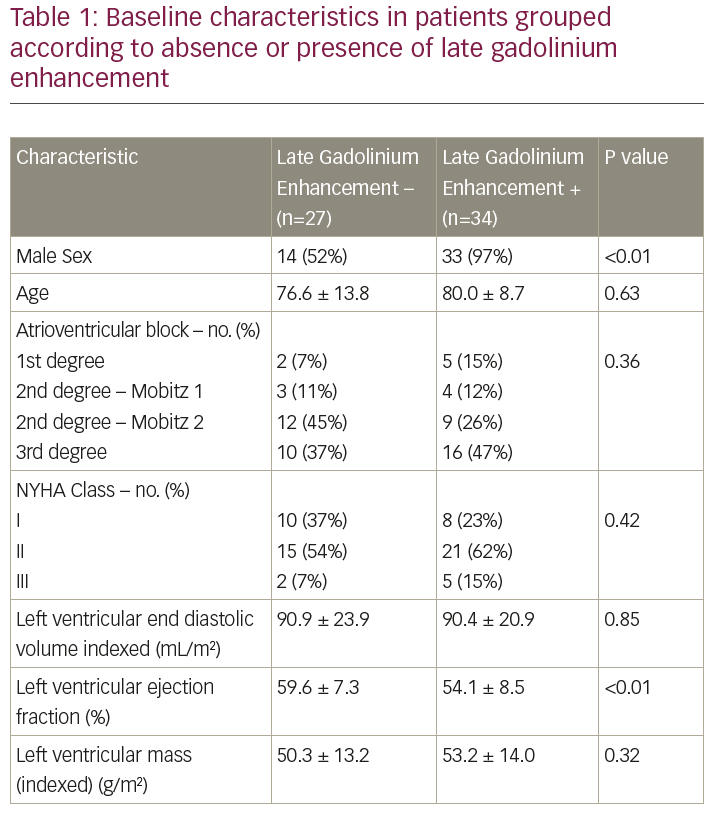
Results: Image acquisition was feasible in all patients despite bradycardia. Of the 61 patients, 34 (56%) had evidence of LGE. There were no significant differences in presenting rhythm, NYHA Class, LV end diastolic volume or mass between those with and without LGE (Table 1). However, patients with LGE had a significantly lower baseline LV ejection fraction (54.1% versus 59.6%; p<0.01). In patients with LGE there was an even split between infarct (n=17) and non-infarct (n=17) patterns. The distribution of LGE was predominantly in the basal to mid inferior and basal to mid inferolateral segments in patients with an infarct pattern and in the basal to mid inferoseptal and basal inferolateral segments in patients with a non-infarct pattern. LGE mass was significantly higher in those with an infarct pattern compared to a non-infarct pattern
(7.4 ± 5.2 g versus 4.5 ± 5.0 g; p=0.03).
Conclusion: Over half of patients had evidence of focal fibrosis which was evenly distributed between infarct and non-infarct patterns. Given the prevalence of LV dysfunction in the pacemaker population further research is needed to assess the interaction between focal fibrosis and the development of heart failure in the longer term, to better identify individuals that might benefit from upfront physiological pacing.