Premature ventricular complexes (PVCs) can cause significant left ventricular (LV) dysfunction leading to debilitating symptoms.1 Multiple single-centre studies have shown that the catheter ablation is effective in curing these PVCs.2,3 However, catheter ablation of ventricular arrhythmias (VAs) originating from papillary muscles can be challenging.2 This is because of the heterogenous electrophysiological substrate which is characteristically observed in papillary muscle VAs. The varied anatomy of papillary muscles, different sites of origin and exits of VAs, role of underlying structural heart disease and concomitant mitral valve involvement can lead to
diverse electrophysiological observations in papillary muscle VAs. In this article, we discuss the complex electrophysiological substrate in papillary muscle VAs including anatomical features, electrocardiogram (ECG) characteristics, potential pathophysiological substrates, typical electrophysiological observations and characteristics of catheter ablation.
Anatomical features of papillary muscles
Location and architecture
Papillary muscles are endocavitary structures located in the mid to the apical third of the ventricular cavity.3 The challenges for catheter ablation, in addition to the endocavitary location, are that the anatomy of the papillary muscles is considerably variable in shape, number and attachments. The LV papillary muscles include the posteromedial and anterolateral groups. The posteromedial papillary muscle is located between the ventricular septum and posterior LV free wall. The anterolateral papillary muscle lies on the anterolateral LV free wall.4 The anterolateral papillary muscle is usually single, unlike multiple groups of the posteromedial papillary muscles. Each papillary muscle can have multiple heads and can be either ‘tethered’ or ‘finger-like’. The tethered papillary muscles are attached to the LV free wall by means of numerous trabecular ridges. The finger-like papillary muscles are usually attached to the LV free wall over a broad base. The right ventricle (RV) papillary muscles include the anterolateral, posteromedial and septal muscle groups. LV posteromedial papillary muscles are a commoner source of papillary muscle VAs than those from LV anterolateral papillary muscles.5 Likewise, the RV septal papillary muscles are the commonest source of RV papillary muscles VAs.6
Activation and preferential conduction within the papillary muscles
The papillary muscles are embedded by a sub-endocardial layer of Purkinje network, which are more concentrated at the base and hence the papillary muscles get activated from the base to the tip.7,8 The site-of-origin of the papillary muscle VAs could be from the Purkinje–myocardial interface or deep within the myocardium anywhere along the length of the papillary muscle. These impulses eventually exit into the free walls of the ventricle. The architecture of the papillary muscles is complex with multiple intervening myocardial strands resulting in anisotropic conduction of the depolarising stimuli. Preferential conduction along the length of these strands and variable exit into the ventricular walls is responsible for the various morphologies of QRS observed at the baseline as well as during an ablation.5 Additionally, false tendons could connect the papillary muscles to other regions of the ventricle and may serve as conduits for conduction of impulses resulting in varied morphologies.9
Electrocardiogram characteristics of papillary muscle ventricular arrhythmias
Hallmark electrocardiogram features
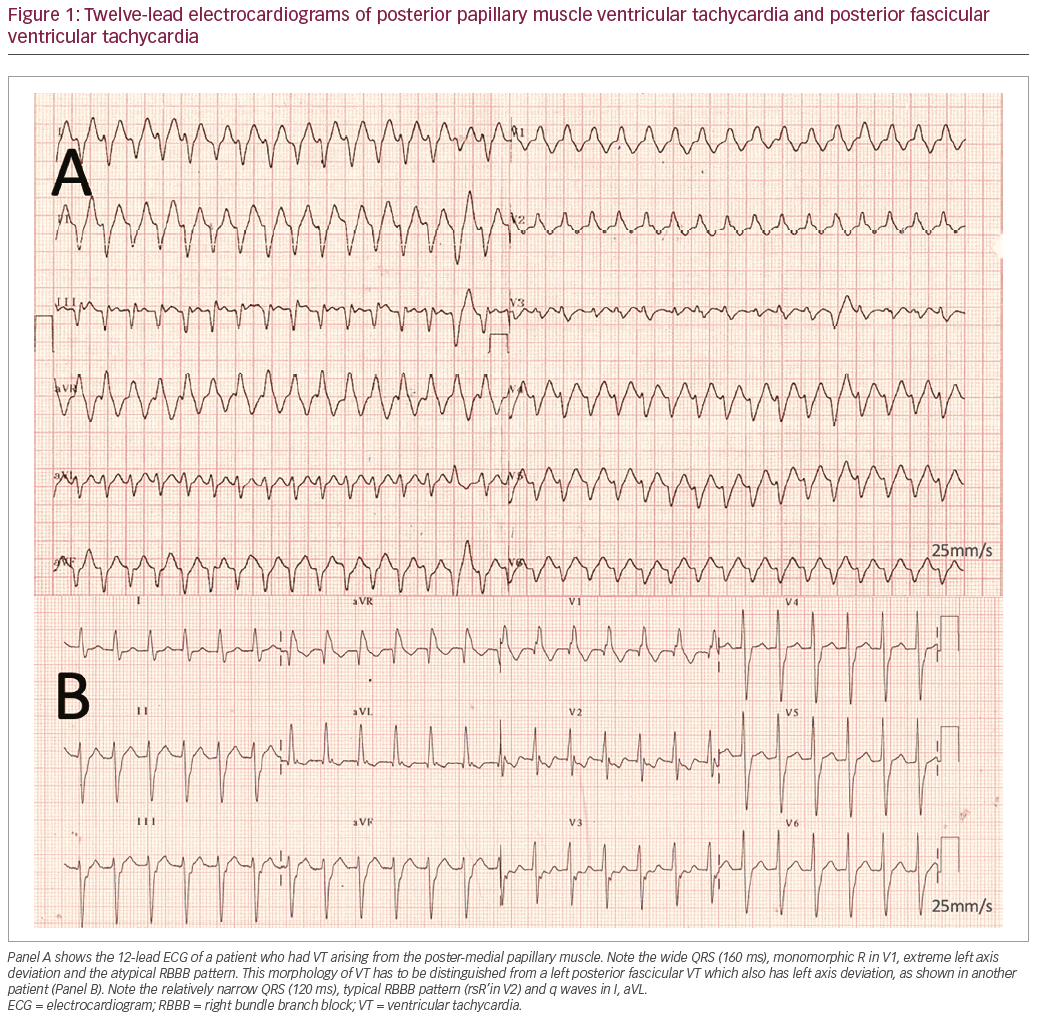
LV papillary muscle VAs have close resemblance to fascicular VAs exiting around the same regions in the ventricle. Papillary muscle VAs characteristically lack the typical right bundle branch block (RBBB) pattern (rsR’ pattern in V1/V2) and more often bear a qR or a monomorphic R pattern in V1 – the atypical RBBB pattern. Also, the discrete q waves characteristic of fascicular VAs, may not be seen in the inferior or lateral leads.10,11 QRS notching in the PVCs is more often a feature of papillary muscle VAs than the fascicular VAs. The delay in conduction of the impulses from the papillary muscle into the surrounding myocardium could explain both the notching and the wideness of the QRS in papillary muscle VAs. The presence of VA QRS ≤130 ms can differentiate fascicular VAs from papillary muscle VAs with 100% sensitivity and specificity (Figures 1 and 2). RBBB pattern of PVCs with ‘inferior limb discordance’ (defined as predominant negative QRS in lead II and positive in lead III) may suggest exit from LV anterolateral papillary muscle.12 The mitral annular VAs originate from the more basal free wall of the LV. A positive precordial lead concordance favours mitral annular VA over papillary muscle VAs.
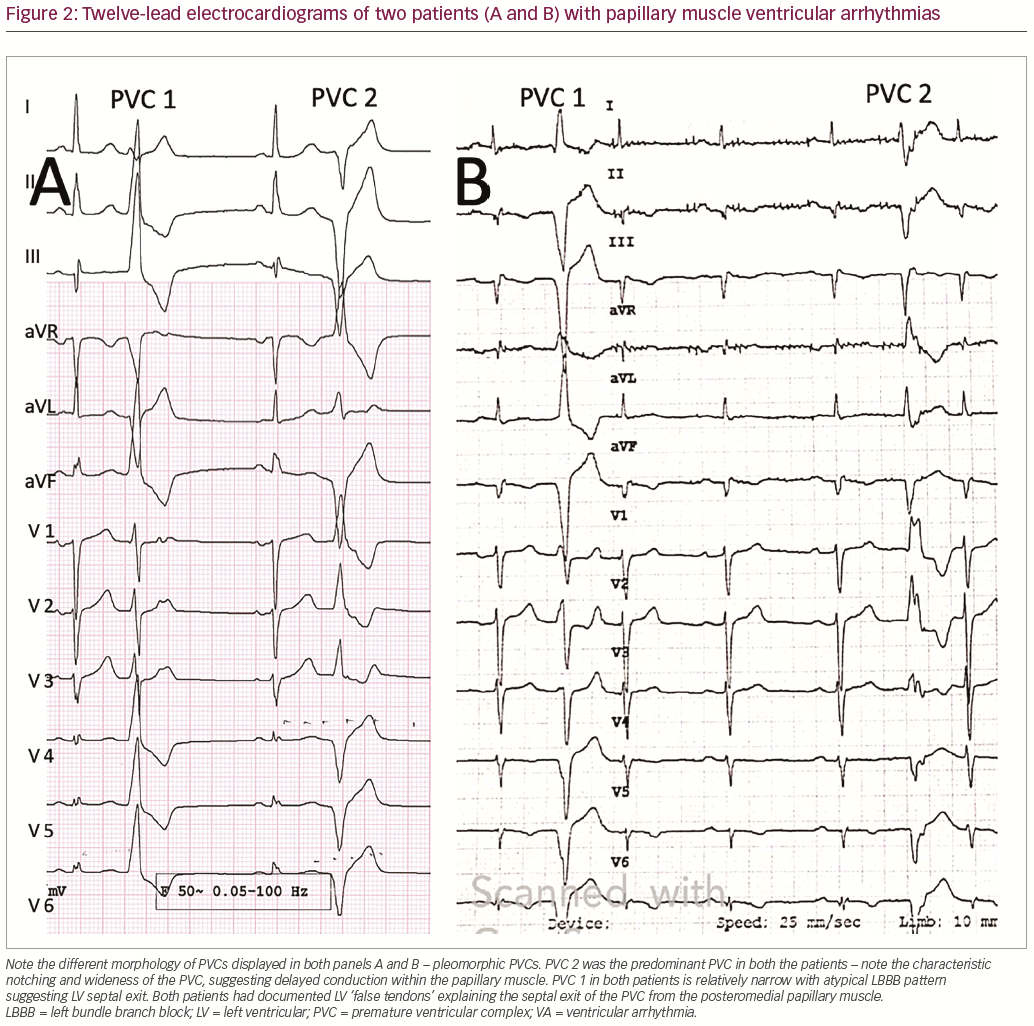
Pleomorphic premature ventricular complexes
Multiple morphologies of PVCs (pleomorphic PVCs) can be observed at the baseline (Figure 2). Presence of pleomorphic PVCs in a 12-lead ECG with atypical RBBB pattern should suggest possible origin from the LV papillary muscles. A number of mechanisms account for these multiple morphologies, such as varying origin within the papillary muscle, shifting exits due to preferential conduction and changing conduction delays due to the variable fiber orientation.13,14 A PVC burden ≥24% and presence of pleomorphic PVCs has been shown to be strongly associated with PVC-induced cardiomyopathy.15–7 Detection of pleomorphic PVCs from papillary muscles can also suggest poorer outcomes from ablation.18
Potential pathophysiological substrates
Precipitating factors
Papillary muscle VAs can occur in both structurally normal as well as diseased hearts.10 Papillary muscles are involved in a number of cardiac pathologies like ischaemia, infiltrative disorders and congenital malformations. They could be a part of a diffuse cardiomyopathy like in endocardial fibroelastosis, amyloidosis, sarcoidosis and ischaemic cardiomyopathy.19 Hypoxia, necrosis, fibrosis and calcification of the papillary muscles can be a potential source of malignant VAs. In patients with mitral valve prolapse (MVP) syndromes, a mechanical stretch-mediated injury to the papillary muscles is the likely trigger for automaticity observed with the papillary muscles.20 MVP results in fibrosis of the papillary muscles in the long term, which can in turn serve as a substrate for VAs.21
Papillary muscle premature ventricular complex-triggered ventricular fibrillation
Papillary muscles are under-recognised sites of triggers for PVC-induced ventricular fibrillation. A significant proportion of patients (nearly 25%) with documented PVC-induced ventricular fibrillation have triggers arising from the papillary muscle.22 Abnormal automaticity within the Purkinje system, more commonly in setting of ischaemic heart disease, can lead to exit into the Purkinje–papillary muscle interface leading to malignant papillary muscle VAs such as ventricular fibrillation/polymorphic ventricular tachycardia (VT).8
Electrophysiological characteristics and implications
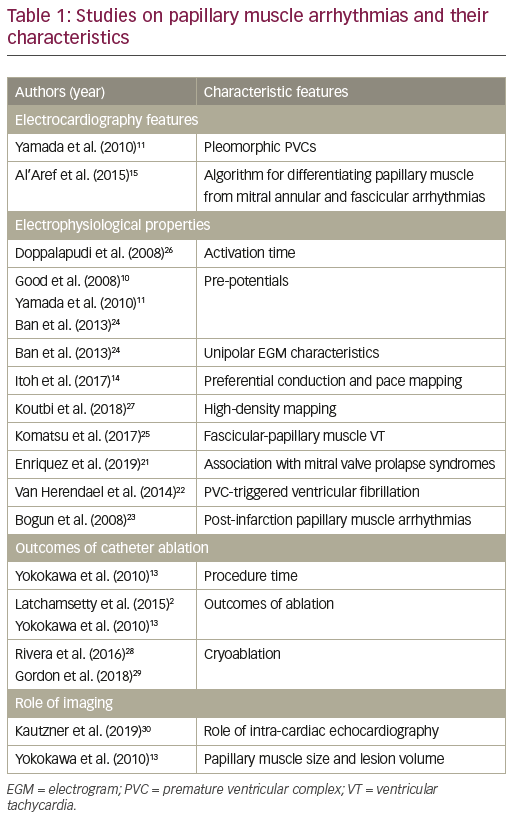
Table 1 enlists studies and their pertinent findings with respect to electrophysiological characteristics of papillary muscle arrhythmias.2,10,11,13–5,21–30
Induction and mechanisms of papillary muscle ventricular arrhythmias
Both automatic and re-entry mechanisms of arrhythmogenesis have been postulated in papillary muscle VAs depending on the substrate.3 The usual presentation of papillary muscle VAs due to automaticity is in the form of frequent PVCs or non-sustained VT. Presentation with sustained VT is possible and more so in the background of exertion and more often points to a re-entry circuit. A re-entry mechanism is more likely when there is heterogeneity in the refractoriness of the papillary muscle due to an underlying structural heart disease like a prior myocardial infarction.23,31 Also, a ‘source–sink hypothesis’ could be attributed to the triggering of VAs in the presence of a substrate within the papillary muscle – the depolarising current from the Purkinje network can unload into the papillary muscles and trigger an arrhythmia.7,8,24 Papillary muscle VAs arising in the zone of a prior myocardial infarction may also be sites of critical isthmus of the re-entry circuit of the VT.12 The Purkinje network surrounding the papillary muscles may serve as regions of slow conduction of a fascicular VT (FVT). This represents a distinct subtype of verapamil-sensitive FVTs.25 Not only do the 12-lead ECG characteristics of papillary muscle FVT resemble the usual FVTs, but also these re-entry circuits are sensitive to verapamil (prolong or terminate). FVTs can be reproducibly induced with programmed atrial/ventricular stimulation.25 As most of the papillary muscle VAs are catecholamine-sensitive, they can be induced with isoproterenol/epinephrine. In the presence of a substrate within the papillary muscle, where the mechanism is likely to be re-entry, the VAs can be induced with programmed atrial or ventricular pacing. Non-inducibility with atrial or ventricular pacing and suppression of the VA upon overdrive pacing without satisfying any criteria for entrainment suggest automaticity as the likely mechanism of papillary muscle VAs and is usually noted in structurally normal hearts.26
Mapping of abnormal potentials
Mapping for the earliest activation signals is the cornerstone for successful ablation of the papillary muscle VAs. Earliest activation signals of 34 ± 15 ms have shown to be effective for successful ablations.10 Recognition of ‘pre-potentials’ is an essential part of activation mapping. There have been frequent observations in the past that pre-potentials could be noted at the sites of successful ablation of papillary muscle VAs. These pre-potentials may be seen in 30–56% cases,10,26,31 and if noted, could predict successful outcomes of ablation (Figure 3).13 The genesis of these pre-potentials has been much debated. There have been three types of pre-potentials described: 1. high-frequency (sharp) potentials, 2. high amplitude low-frequency (rounded) potentials, and 3. low amplitude low-frequency (rounded) potentials. The high-frequency potentials are the Purkinje potentials and, when also found during the sinus rhythm, suggest a superficial origin of the VAs from the Purkinje–myocardial interface. These Purkinje potentials could be observed in up to 45% cases.10 When separated from the ventricular potential by an iso-electric line, these Purkinje potentials may suggest a delayed exit into the myocardium due to slow conduction.32 The low-frequency potentials are likely to be of myocardial origin (myo-potentials). These myo-potentials should suggest deeper origin of the VAs from the papillary muscle. The amplitude of these potentials should be able to suggest near-field (high amplitude) and the far-field (low amplitude). The far-field potentials suggest deep intra-mural origin or an epicardial exit of the VAs.
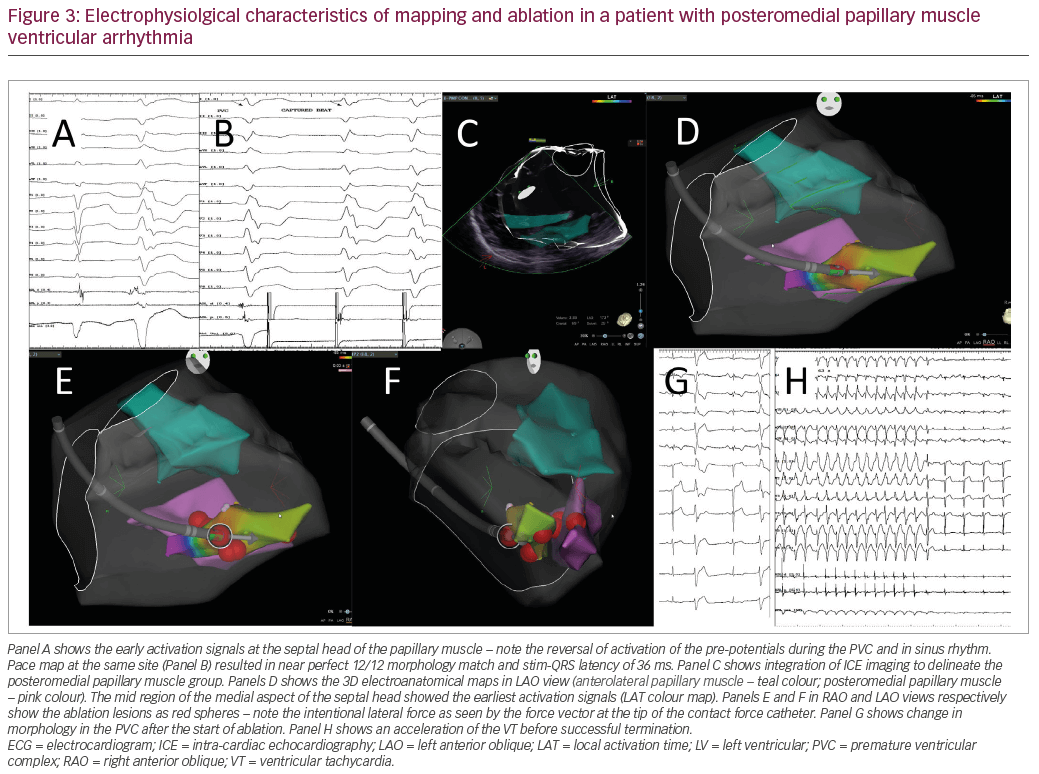
Detection of abnormal potentials like late systolic or early/late diastolic potentials at sites of early activation during sinus rhythm or during PVCs should suggest an abnormal substrate. The diastolic potentials found on the papillary muscles may serve as targets for ablation in patients with FVT. Mapping with multi-electrode catheters has not been much studied and it remains to be seen if they have better sensitivity than mapping with conventional quadripolar catheters in picking up the pre-potentials.27 Unipolar mapping is important to understand and differentiate the near-field and far-field early potentials.33 Presence of q waves coinciding with the onset of the early pre-potentials should suggest the subjacent source of the VAs to the mapping catheter. The slow downstroke of >50 ms of the q wave of the unipolar electrogram has been shown to predict success; however, this was studied only in a small cohort of patients.24
Pace mapping at the papillary muscles
Pace mapping at exit sites may not be representative of the site of origin. During pace mapping, the morphology of the QRS on the 12-lead ECG can vary depending on the pacing output, the amount of myocardium captured, and underlying scar, if any. Pace mapping should be at an output just above threshold to ensure capture of only the local myocardium. The 12-lead pace map should be interpreted with caution keeping in mind the property of preferential conduction
of the papillary muscle VAs.13,26 A good pace map, when associated with early activation signals, can define success in nearly 70% cases (Figure 3).34,35 However, a perfect pace map may be achieved only in 30–60% cases.10,34 Nevertheless, pace mapping can be a strategy for papillary muscle VA ablation and is especially useful when there are no inducible VAs or in haemodynamically unstable VAs precluding an activation map and when ablation at earliest activation sites fail. Good pace maps can be obtained at multiple sites remote to the earliest activation sites and ablation at these sites might be successful when VAs are not inducible.35
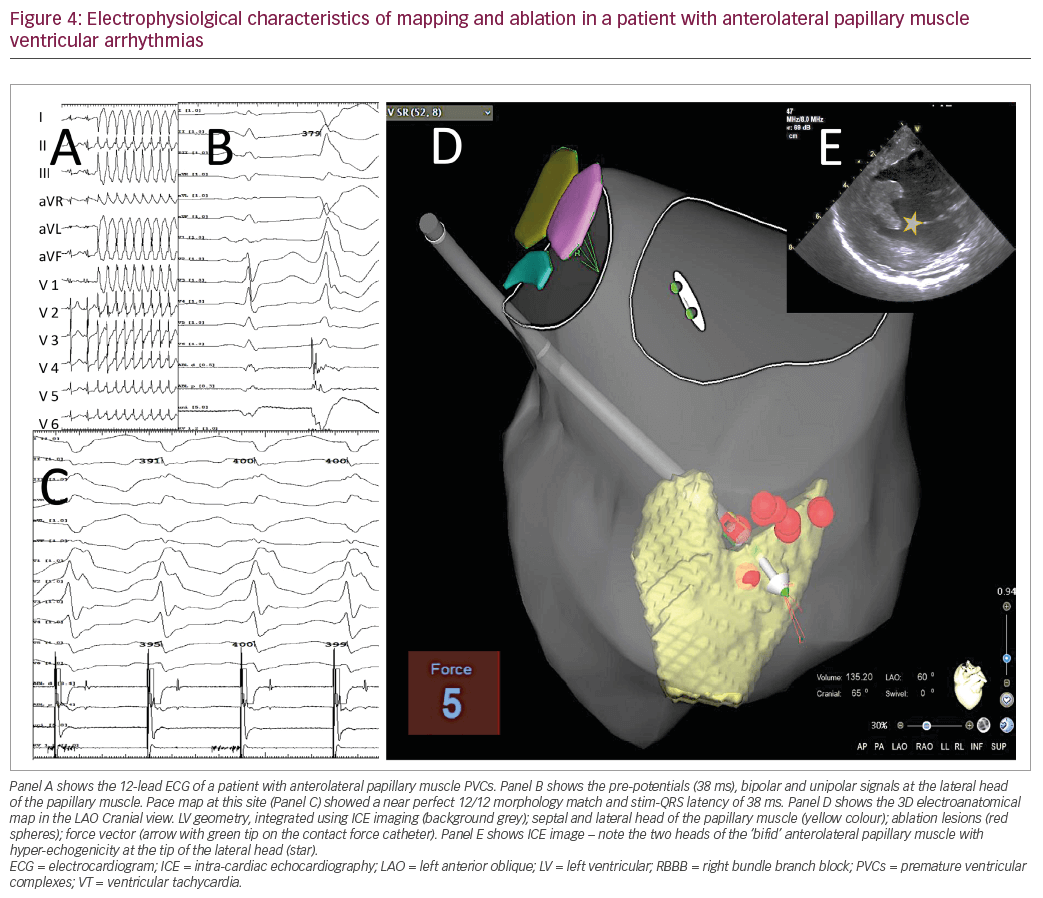
Understanding of the stimulus-QRS duration (latency) of the paced complex is important to understand the preferential conduction observed in papillary muscle VAs (Figures 3 and 4). It is possible that the paced QRS matches the morphology of the PVC, yet the site of pacing might be distal to the site of origin. Therefore, pace mapping of the papillary muscle VAs should consider not only the morphology match but also the latency of capture as it has been shown that ablation at these sites is successful when previous attempts have failed at the earliest activation sites.35
Characteristics of catheter ablation in papillary muscle ventricular arrhythmias
Short- and long-term success rates
The acute success rate of ablation varies from 60–100%, but the long-term success rate of these arrhythmias was found to be less promising (60%), as shown in a large multicentre study.2 The recurrence rates with respect to anterolateral and posteromedial papillary muscles has been noted to be 71% and 50%, respectively.34,36 The higher recurrence rates observed in the ablation of papillary muscle VAs are because the papillary muscles are very thick structures and arrhythmic foci of papillary muscle VAs are more often deeper from the endocardium. The depth of the radiofrequency lesion may not encompass the deep focus. Also, the close proximity of the heads of the papillary muscles and their vigorous contraction during systole can pose difficulties during catheter manipulation due to unstable catheter positions. Considering the deeper origin of the papillary muscle VAs, the choice of catheter is always an irrigation catheter to create a deeper and wider lesion. Ablation with conventional non-irrigation catheters has, in fact, been shown to have recurrences.26 Establishing contact with an endocavitary structure like the papillary muscle has been recognised as the most challenging aspect of the ablation. Therefore, use of contact-force catheters and adjunct imaging guidance like intra-cardiac echocardiography (ICE) can aid in improving success rates.37
Cryoablation is now established as an alternate modality in papillary muscle VA ablation especially when catheter contact is an issue or in cases with recurrences with radiofrequency ablation (RFA).28 The advantage of cryoablation is the catheter-tissue adherence at extremely
low temperatures increasing likelihood of a stable catheter position. The cryoablation catheter can also target multiple different surfaces of the papillary muscle. Acute success has been reported to be 100%.36 Excellent success rates (93.8%) have also been reported in cases of
failed papillary muscle VA ablation with RFA.29 The disadvantages of cryoablation are reduced manoeuverability due to bulky catheters, reduced lesion depth and inability to accurately project the catheter tip onto the electroanatomic map.
Sites of ablation
RFAs are usually carried out at the base of the papillary muscle, as ablating the head of the papillary muscle can potentially risk in damage to the chordae resulting in mitral valve dysfunction. ‘Circumferential’ ablation at the base of the papillar muscle can isolate the muscle and block all exits into the LV. Such a strategy has been shown to be effective in reducing recurrences.31 The number of RF lesions required for elimination of papillary muscle VAs is significantly higher than those for fascicular VAs.10,11 This is more related to the complex anatomy, difficulties in maintaining contact and deeper foci within the papillary muscles. The retrograde aortic approach to both the LV papillary muscles is helpful in most cases. Trans-septal access can be attained for better access to the postero-medial group of papillary muscles or the lateral heads of the anterolateral papillary muscles.
Role of multi-modality imaging
ICE imaging during ablation of papillary muscle PVCs enables visualisation of the head, body and base of the papillary muscles. More importantly ICE helps in establishing contact of the ablation catheter during RFA. ICE has been extensively used in ablation and has become the standard-of-care for ablation of VAs from endocavitary structures like the papillary muscles.30 Moreover, real-time integration of ICE imaging with 3D electro-anatomical mapping enables precise delineation of the geometry of the papillary muscles in relation to the cavity (Figures 3 and 4).37 ICE can also identify areas of high echogenicity which may correspond to areas of low bipolar voltage and scar.21,38 Ablation at the parietal region of the RV infundibular muscles have high recurrence rates and is technically challenging due to the location and ICE can play a crucial role in establishing contact with these structures.39 The 3D electro-anatomical mapping systems have advanced to enable integration of ICE, computed tomography (CT) and magnetic resonance imaging (MRI) to aid precise mapping of papillary muscles. Additionally, advanced tools such as automated pace mapping modules and integration of ICE, CT and MRI algorithms within the 3D electro-anatomical mapping systems can help in achieving better success rates during ablation of these complex structures in both the LV and the RV.6,40,41 A larger arrhythmogenic mass of the papillary muscles detected on cardiac MRI can also correlate with poorer outcomes from RFA.13
Observations during ablation
Morphology change can be observed during ablation of papillary muscle VAs in 47% cases.34 A morphology change observed during or after delivery of RFA burns suggests a shift in the preferential conduction along the length of the papillary muscle and exit of the PVC from a different site at the LV free wall, though the source continues to remain the same (Figure 3). The morphology of the newer PVC should be studied, and activation map has to be repeated for the same. More often, this may necessitate ablation on both sides of the papillary muscle to get rid of the PVCs.5,34 In patients with FVTs, a change in the 12-lead morphology of the tachycardia upon ablation at the routine target sites of ablation such as the posterior/anterior fascicular sites, along with a reproducible initiation of the tachycardia, should alert the operator to look for diastolic potentials in the papillary muscles as these structures are known to be involved in the circuits of FVTs. Successful ablation of these abnormal potentials may eliminate these tachycardias.25 Acceleration of PVCs or induction of VT is another frequently observed characteristic during the ablation of papillary muscle VAs.







