Introduction: Irrigated catheters are the standard tool for radiofrequency (RF) ablation in the left atrium and ventricles. However, pathological studies of irrigated RF lesions show a “tear-drop” shape, with the widest diameter some depth below the endocardial surface and relative endocardial sparing. This results in the need for overlap of lesions to achieve contiguity at the endocardial surface. There has been very little investigation into the effect of altering irrigation rate on lesion shape and volume. We hypothesised that varying the irrigation rate would optimise lesion shape by minimising endocardial sparing while maintaining lesion depth.
Methods: In an ex vivo animal heart model, irrigated ablation lesions were performed in porcine ventricular tissue using an Intellatip MiFi OI catheter with 5 different irrigation protocols: A. fixed rate (30 ml/min); B. continuous reduction (30–2 ml/min over 30 s); C. continuous increase (2–30 ml/min over 30 s); D. stepwise reduction (30 ml/min (10 s) to 16 ml/min (10 s) to 2 ml/min (10 s)); E. stepwise increase (2 ml/min (10 s) to 16 ml/min (10 s) to 30 ml/min (10 s). Other parameters such as contact force (10 g), power (30 W), and total ablation duration (30 s) were constant. Any occurrence of steam pops during ablation were recorded. Tissue sections were stained with triphenyltetrazolium chloride (TTC) after ablation to clarify lesion boundaries, allowing accurate measurement. Surface diameter, lesion depth, maximum diameter, and depth at maximum diameter were then measured using Vernier Calipers to calculate lesion volume. Pictures of lesions were taken and analysed further by ImageJ software to measure the degree of endocardial sparing and lesion area.
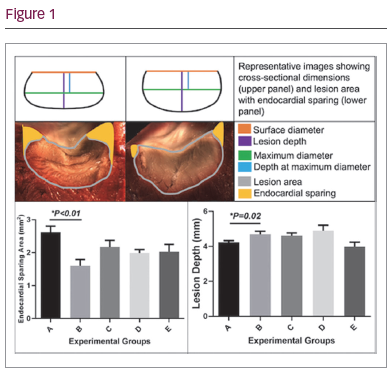
Results: 10–20 lesions were performed for each irrigation protocol. Of the four experimental protocols, continuous reduction in irrigation rate from 30 to 2ml/min (protocol B) resulted in the most optimal lesion shape (Figure 1). With this protocol, endocardial sparing area was significantly reduced compared to fixed-rate irrigation (1.60 versus 2.62 mm2, p<0.01), with a trend towards an increase in surface diameter (9.41 versus 8.57, p=0.08). Lesion depth was also significantly greater (4.70 versus 4.24 mm, p=0.02), with no significant difference in lesion volume (378 versus 333 mm3, p=0.38) or maximum diameter (10.3 versus 10.6 mm, p=0.53).
Steam pop occurred in 1 of 20 (5%) lesions in each of the fixed-rate and continuous reduction protocol groups.
Conclusions: Continuous reduction in irrigation flow rate from 30 to 2 ml/min during irrigated RF ablation applications results in reduced endocardial sparing, with greater (rather than reduced) lesion depth and similar lesion volume. Further assessment of this protocol is planned in an in vivo large animal model in order to assess the potential for improved irrigated RF ablation efficiency.