Background: QT-RR hysteresis describes the lag of the QT interval adaptation to heart rate changes. This phenomenon is typically observed during exercise when, for the same RR interval, the QT interval is longer while heart rate increases during exercise and shorter when heart rate decreases during recovery. Experimental studies have shown that parasympathetic blockade reverses this expected QT-RR hysteresis that would be due to directional changes in the RR interval, suggesting that differential parasympathetic inputs during exercise and recovery are responsible in large part for this phenomenon. Importantly, reduced heart rate recovery from exercise is a predictor of all-cause and cardiovascular (CV) mortality and is considered to reflect impaired parasympathetic tone. Given that parasympathetic effects on the sinus node may differ from their effects on ventricular repolarisation and that repolarisation may be more directly linked to the ventricular pathophysiology, we hypothesised that reversed QT-RR hysteresis could provide prognostic information for CV outcome in the general population.
Methods: QT-RR plots were derived from exercise ECGs of 25,228 individuals without a history of CV events from the UK Biobank study (general population) aged 40–76 years. The QT-RR interval plots for exercise and recovery were modelled by linear regression analysis after which we could compute the hysteresis area as the area between the two modelled curves. Normal hysteresis was defined as a positive area (i.e. the line for recovery would be below the line for exercise), and reversed hysteresis was defined as a negative area (the recovery line is above the exercise line). We evaluated the prognostic value for (1) CV death or hospitalisation and (2) all-cause mortality (ACM). Kaplan-Meier curves were generated for each endpoint and we computed hazard ratios (HR) using univariate and multivariate Cox regression analyses. Variables with P<0.1 in the univariate were entered in the multivariate analysis in which we adjusted for the following potential cofounding variables: age, sex, diabetes, smoking, systolic blood pressure, resting heart rate, heart rate changes during exercise and recovery, and prolonged QTc (QTc > 450 ms (men) or 460 ms (women). The median follow-up time was 6.9 years.
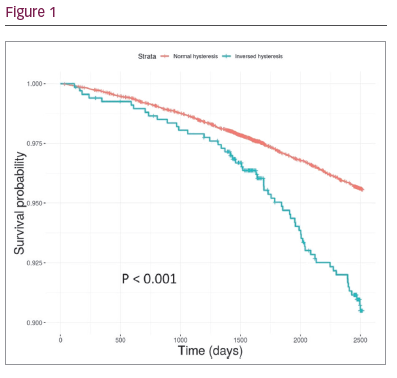
Results: CV death or hospitalisation occurred in 1,087 individuals (4.3%) and 454 (1.8%) died from all-cause mortality. Reversed hysteresis occurred in 669 individuals (2.6%) and was associated with higher incidence of CV events (p=2.1 x 10–7) and ACM (p=1.6 x 10–3). Kaplan-Meier estimators for individuals with normal and reversed hysteresis were significantly different for CV events (Figure 1) and ACM. In the univariate Cox regression analyse, reversed hysteresis was associated with increased risk for CV events (HR = 2.1 (CI: 1.6–2.8), p = 1.5 x 10–8) and ACM (HR = 2.1 (1.4–3.1), p = 4.9 x 10–4). Reversed hysteresis remained significant after adjusting for covariates in the multivariate analyses, HR = 2.0, (1.5–2.6) for CV events (p = 7.4 x 10–7) and HR = 1.7, (1.1–2.6, p = 9.0 x 10–3) for ACM.
Conclusions: Reversed QT-RR hysteresis is an independent risk predictor for CV events and ACM in the general population. Our findings support the hypothesis that the effect of impairment to increase parasympathetic activity rapidly on ventricular electrophysiology provides additional prognostic information regarding CV outcome and mortality.