Background: There are increasing numbers of patients referred with suspected dysautonomia to electrophysiology clinics. Many referrals come from the internet, with one Californian website registering over 2,200 patients with POTS alone. Time constraints, unclear reimbursement and provider preferences have left many of these vulnerable patients without a cardiologist with interest or expertise in dysautonomias, or even worse without anybody to take their symptoms seriously. We report our cumulative experience on how in a busy interventional cardiology practice, these patients can be effectively cared for with improved clinical outcomes.
Methods: We compiled a longitudinal series of patients under the dysautonomia clinic at Good Samaritan Hospital, a tertiary referral centre in Los Angeles, CA, USA. Patients were seen by physicians and nurse practitioners with expertise in the diagnosis and management of these conditions. The diagnostic categories were: postural orthostatic tachycardia syndrome severe (associated with presyncope, POTS – S), postural orthostatic tachycardia syndrome non-severe (POTS – NS), orthostatic hypotension (ortho), vasodepressor (VDP), and mixed. Patients were also investigated for mast cell disease (MCD), with overlap between diagnostic categories. Patient demographics, medication response, device implantation rates and concomitant use of analgesia and anti-depressants were recorded.
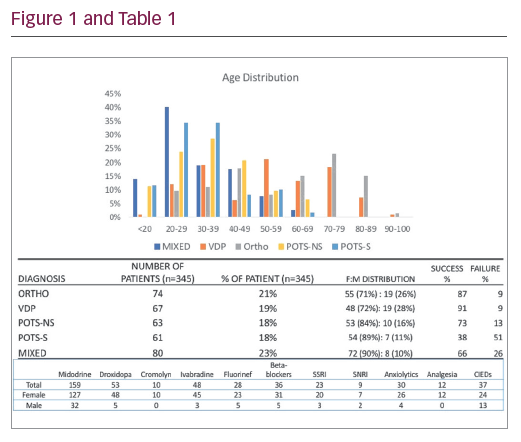
Results: In total 345 patients were assessed in the dysautonomia office. There was no significant difference in diagnostic frequency between the five categories (Table 1), but a clear female preponderance (82%). There were 62 patients with mast cell disease, of which 52 also had severe POTS. Figure 1 shows the trends across subdivided ages, with orthostatic hypotension peaking much later than mixed or severe POTS, which peak early. The treatment success with medication varied between the subgroups, with vasodepressor syncope having the best success rate of 91% and POTS (severe) having the worst success rate at 38%. Midodrine, droxidopa and ivabradine were the most commonly prescribed medications (Table 2). In 37 patients, a cardiac implantable electronic device (CIED) was implanted.
Conclusions: Dysautonomia patients represent a challenge for modern cardiology outpatients, as they require longer consultation times, dedicated staff and continuity of care to build trust. Despite these issues, we have demonstrated that in a high-volume tertiary referral centre it is possible to obtain clinical successes in a wide range of these patients, adopting a patient centred multidisciplinary approach. Patient word of mouth and online ratings substantially help to build a referral base, and we have a waiting list of over 100 new patients for assessment. Ongoing studies are focussing on how to improve success rates in the most severe forms of dysautonomia and how to relate treatment to underlying pathophysiological processes.