Aims: Palpitations are a distressing symptom for patients and present a difficult diagnostic challenge in primary care. Patients with benign palpitations are often referred onto secondary care services out of fear of missing more sinister conditions. Local guidelines have been provided to referrers to improve service delivery. We analysed the adherence to these.
Methods: We conducted a clinical audit for patients referred by primary care to a cardiology clinic at our trust in 2018. New patients referred directly from primary care services with a primary presenting complaint of palpitations were included. Referrals were assessed by gauging adherence to local guidance through the evaluation of clinical letters and were split as appropriately or inappropriately referred. We also reviewed the investigations and final diagnosis for each patient. A two-sample t-test with equal variance assumed was used to assess number of investigations. Chi-squared test was used to assess variation between cardiac memo and MRI use in the two groups as these were deemed as investigations that are requested only in patients requiring higher clinical attention.
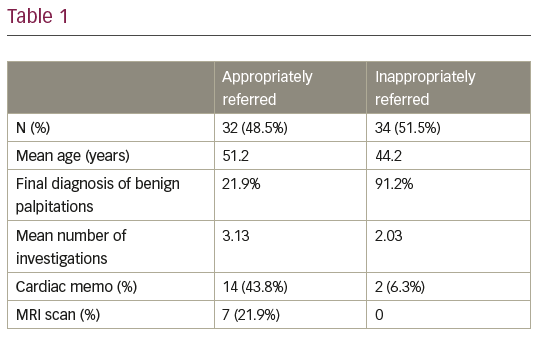
Results: A total of 565 patients were referred to one outpatient clinic by primary care. Of these, 11.7% (n=66) were for palpitations and met our inclusion criteria. Mean age was 47.8 years and 56.1% (n=37) were female. Mean time between referral and first appointment was 103.6 days. 48.5% (n=32) of patients were referred appropriately. Mean age was 51.21 and 44.21 in appropriately and inappropriately referred patients respectively. Final diagnosis of benign conditions such as benign ectopic beats were found in 21.9% and 91.2% of the appropriately and inappropriately referred groups respectively. Mean
number of investigations for appropriately referred patients was 3.13 compared to 2.03 in those inappropriately referred, this difference was statistically significant (mean difference of 1.10 [CI: 0.60–1.59]). Both cardiac memo (p<0.05) and MRI (p<0.05) were statistically more likely to be used in the appropriate group.
Conclusions: The results from our audit indicate that palpitations contribute a significant proportion of referrals from primary care. A large number of these patients are being referred inappropriately and not in accordance with guidance, suggesting that there are barriers to implementing these guidelines in practice that require further investigation. Inappropriately referred patients are less likely to require higher level investigations and are more likely to have benign
diagnosis suggesting that these patients could be managed in primary care. Adherence to guidelines may prevent unnecessary referrals in patients that could be managed in primary care.