Introduction: Brugada syndrome (BrS) is an important cause of sudden cardiac death but diagnosis can be challenging. Body surface ECG changes in BrS are dynamic, and elicitation by sodium channel blockade carries a risk of death. The epicardial substrate of the overt Type 1 BrS ECG is known but not always spontaneously present in cardiac arrest survivors with confirmed drug-induced BrS. Traditional markers of risk in Brugada syndrome (spontaneous Type 1 ECG and syncope) are often absent in cardiac arrest survivors.
Methods: A total of 21 BrS cardiac arrest survivors (BrS VF), 20 BrS patients without a history of potentially lethal arrhythmia and 11 asymptomatic relatives of BrS patients proven not to have the condition by negative Ajmaline test were recruited. The 252 lead body surface ECG was combined with a 3D torso and cardiac model to reconstruct epicardial electrograms (ECG imaging; CardioInsight, Medtronic, USA) following maximal Bruce protocol exertion and into full recovery (~10 min). Local activation (LAT) and repolarization times (LRT) were measured by fully automated software and used to calculate measures of delay, dispersion and gradients for AT and RT.
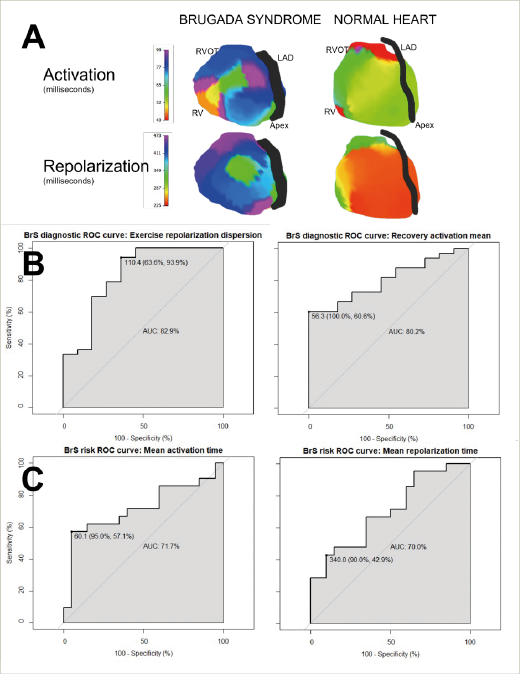
Results: Patients with concealed BrS had longer mean whole heart AT (57.6 vs 52.5 ms; p=0.0022), and more dispersed RTs (central 95% range 136 vs 116 ms; p=0.0094) in recovery, as well as more dispersed RTs (central 95% range 139 vs 112 ms; p=0.0007) and steeper RT gradients immediately after exercise (1.7 vs 1.4 ms/mm; p=0.029). Figure 1A demonstrates visual differences in epicardial activation and repolarization maps between BrS and normal hearts. Mean AT in recovery and dispersed RT in exercise were good differentiators of concealed BrS patients from their unaffected relatives (AUC 0.83 and 0.80 respectively, specificity and sensitivity analysis by Youden’s method in Figure 1B). ECG imaging measures were then compared between the BrS VF and BrS patients. The BrS VF group had longer mean whole heart AT (56.8 vs 52.5 ms; p=0.004) and RT (153.8 vs 133.7 ms; p=0.049) than the BrS group. Mean AT and RT provided reasonable differentiation of BrS VF survivors (AUC 0.71, 0.70 respectively, specificity and sensitivity analysis by Youden’s method in Figure 1C). In contrast, traditional risk markers were evenly distributed between groups: 5 BrS VF survivors and 3 BrS patients had previous spontaneous Type 1 ECG. Three patients in each group had suffered syncope (prior to their sentinel event in the VF survivors).
Conclusion: Measures of epicardial electrophysiology by ECG imaging at rest and immediately following peak exercise could form a role in both diagnosis – possibly reducing the need for sodium channel blocker challenge – and risk stratification in the Brugada syndrome. Further study would be required to determine the clinical effectiveness of such a tool in a consecutive population. ❑