Introduction: Successful pulmonary vein isolation (PVI) requires the creation of continuous and durable transmural ablation lesions encircling the pulmonary veins (PV). During contact force (CF) radiofrequency (RF) delivery, catheter stability is clearly an important determinant of lesion creation. However, the precise extent to which cardiac and respiratory motion influence site-specific RF effects is presently unknown. Therefore, we aim to determine whether the mode of ventilation – volume-controlled intermittent positive pressure (IPPV) versus high frequency jet ventilation (HFJV) – influences RF lesion creation during PVI.
Methods: Consecutive, unselected adult patients underwent single-operator CF PVI using CARTO® and VISITAG Module guidance (Biosense Webster). IPPV was at 6-8ml/kg, 14-16 breaths/minute guided by end-tidal CO2. During HFJV, GA was induced and maintained with total intravenous anaesthesia using depth of anaesthesia monitoring (BISTM, Medtronic Inc.). A Monsoon III ventilator (Acutronic Medical Systems AG) delivered jet ventilation at 150jets/min using 60% inspired oxygen concentration (titrated to maintain saturations 95%); driving pressure 1.0 bar, 1:1 inspiration to expiration ratio. RF was delivered using Agilis sheath support and during coronary sinus pacing at 600ms; force-over-time 100% min 1g and 2mm position stability (ACCURESP off). 30W was delivered to all sites during IPPV, whereas 20W was delivered to left-sided left atrial posterior wall (LAPW) sites during HFJV. Time to pure R unipolar electrogram (UE) morphology change and impedance drop (ImpD – both total and maximum rate) were measured at the first-ablated LAPW sites using exported VISITAG Module data.
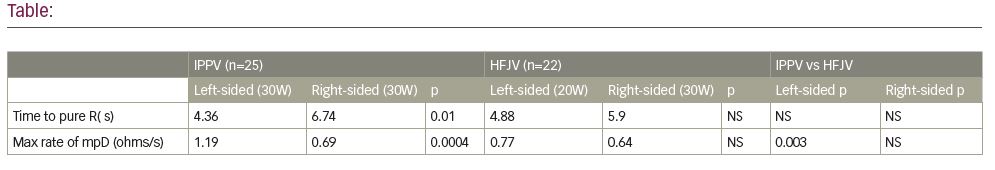
Results: 25 and 22 patients were ventilated using IPPV and HFJV respectively. During IPPV and using 30W, time to pure R UE morphology change was significantly shorter at left-sided sites (p=0.01). However, during HFJV there was no significant difference between left (20W) and right-sided (30W) LAPW sites. There was no significant difference in time to pure R between IPPV and JV when comparing left and right-sided LAPW sites (table). There was a significant difference (p=0.003) in rate of impedance drop between IPPV and HFJV in only LAPW sites, with a greater rate of impedance drop when using IPPV. The rate of impedance drop was also greater in LAPW sites than right-sided sites during IPPV (p = 0.0004), but there was no significant difference in rate of impedance drop at LAPW and right-sided sites during HFJV.
Conclusions: Extending the findings of previous studies, we have demonstrated a significantly greater rate of impedance drop at left versus right-sided LAPW sites during CF PVI under GA. However, compared to IPPV, HFJV was without effect on the rate of impedance drop at right-sided LAPW sites, indicating that cardiac contraction-induced motion is the main determinant of catheter-tissue instability at right-sided sites under these conditions. Finally, as the rate of impedance drop did not differ between left-sided (at 20W) and right-sided (at 30W) LAPW sites during HFJV, this approach may be used to achieve equivalent RF effects using a fixed RF duration protocol.