Introduction: A fundamental treatment decision in the management of patients with atrial fibrillation (AF) is whether to adopt a rate or rhythm control strategy. Randomised, controlled trials broadly suggest that mortality is unaffected by this decision. However, there are groups of patients who may benefit from rhythm control for symptom relief, heart failure management or to reduce hospitalisations. We sought to describe the use of anti-arrhythmic drugs (AADs) and atrial ablation over the past 20 years in England as a surrogate for the rhythm control approach.
Methods: We conducted a retrospective study using data from the Prescription Cost Analysis system, which holds information on every prescription dispensed in the community in England. We obtained data from 1998 to 2019 for all Class Ia, Ic and III AADs. In addition, we used data from the Quality and Outcomes Framework and The National Institute for Cardiovascular Outcomes Research to describe annually the number of patients with AF and total number of ablations, respectively.
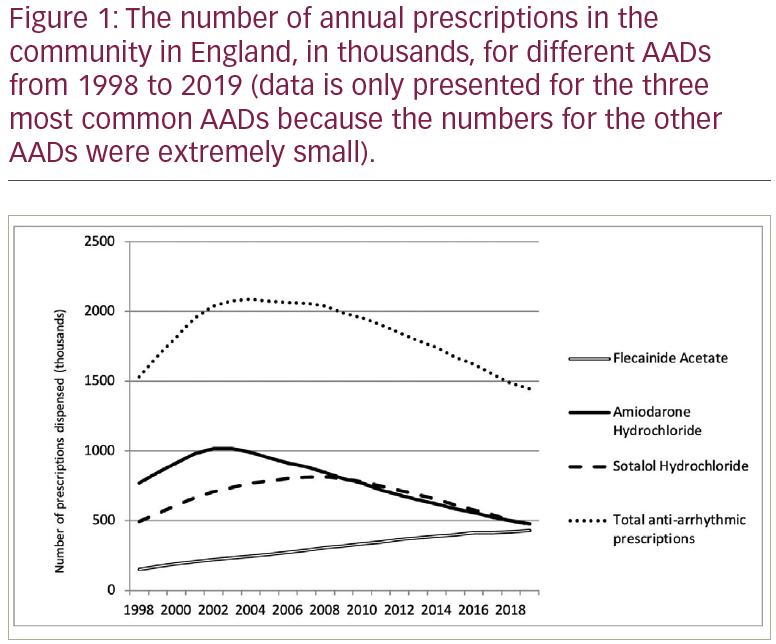
Results: The number of prescriptions for AADs is displayed in Figure 1 and demonstrates an initial increase in prescriptions for all AADs from 1998 to 2002 but an overall decline from 2002 to 2019. The exception to this is that flecainide prescriptions increased linearly throughout this period. There has been a linear increase in the number of patients with atrial fibrillation from 692,054 in 2007 to 1,174,959 in 2019. The total number of atrial ablations has increased from 2,726 in 2008, to 9,450 in 2019.
Conclusions: There has been an overall reduction in AAD prescriptions since 2002 despite an increase in the number of patients with AF. This suggests a shift in practice from rhythm to rate control. The increased use of flecainde and atrial ablation suggests that these are the strategies employed for those patients selected for rhythm control. The total number of ablations is still very low and around half that performed in other European countries.