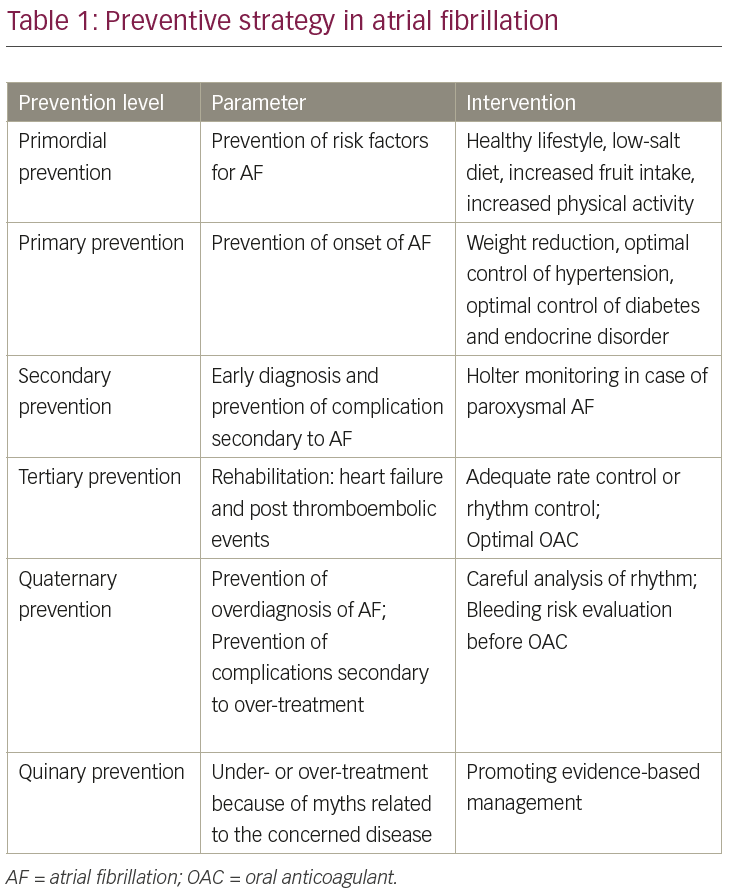
Long-term follow-up of patients with atrial fibrillation (AF) has confirmed a significant increase in cardiovascular events, long-term risk of stroke, heart failure and all-cause mortality (89% in those with AF compared to 27% in those without AF).1 Not only is AF associated with a five-fold increased risk of stroke, AF-related stroke is also likely to be more severe than non-AF-related stroke.2–3 AF is associated with a three-fold risk of heart failure4–6 and a two-fold increased risk of both dementia7 and mortality.8 Since AF is associated with multiple modifiable risk factors, prevention strategies should begin right from the primordial level. Stepwise strategies are discussed in this current review (Table 1).
Primordial prevention
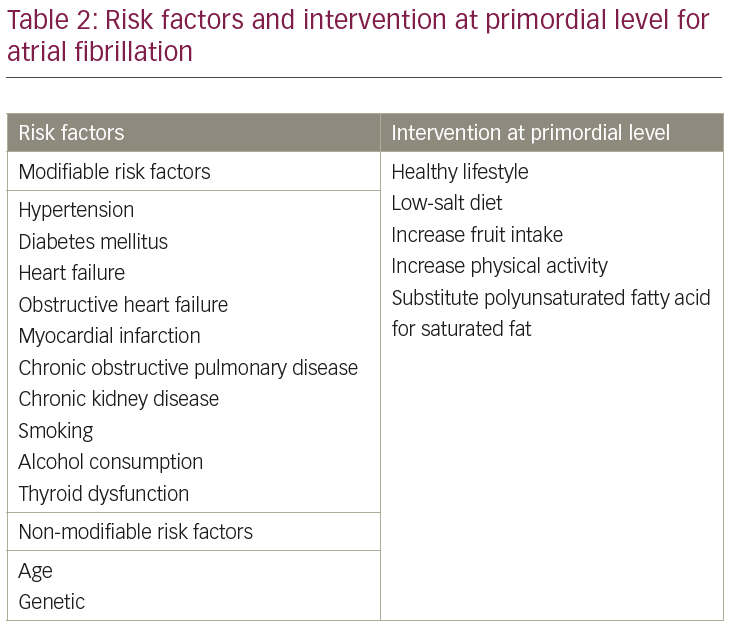
In the context of this article, the term ‘primordial’ is representative of early intervention prior to the onset of risk factors that precede disease. The goal of primordial prevention may be achieved by lifestyle modification. This aims to halt the development of modifiable risk factors (Table 2) that can set the stage for development of AF. The STRIP (the Special Turku Coronary Risk Factor Intervention Project for Children) trial investigated the effect of primordial level intervention by providing healthy fats; more fruits, vegetables and whole grains; and less sodium to selected populations from infancy to adolescents, on the prevalence of metabolic syndrome.9 STRIP Investigators recommended limiting salt intake, substituting unsaturated for saturated fats and promoting healthier foods starting in infancy and toddlerhood in order to help achieve ideal cardiovascular health. These recommendations were based on the fact that healthier outcomes were primarily driven by reduction of high blood pressure in both sexes and high triglyceride in boys. The government, along with the food industry, should help educate the public regarding the importance of a healthy diet and how to adhere to it. The co-operation of the food industry is required to achieve significant reductions in sodium intake.
Primary prevention
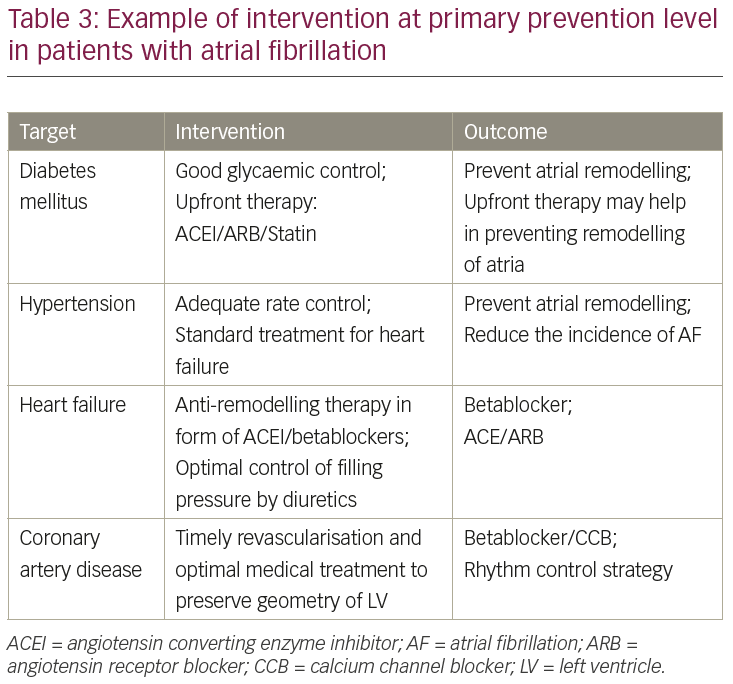
Analysis of the original Framingham Heart Study cohort has concluded that the risk factors for cardiovascular disease also predispose to AF.10 The authors confirmed the statistically significant association of diabetes (odds ratio [OR] 1.4 for men and 1.6 for women), hypertension (OR 1.5 for men and 1.4 for women) and congestive heart failure (OR 4.5 for men and 5.9 for women), with development of AF in both sexes.10 Optimal control and modification of these risk factors may substantially reduce the onset of AF. Intervention in these groups of patients may be in the form of angiotensin converting enzyme (ACE) inhibitors/angiotensin receptor blockers (ARB) and statins. As AF is one of the major causes of stroke, heart failure, sudden death and cardiovascular morbidity in the world,11 intervention to prevent the onset of AF in this target population will be a cost-effective means of reducing further burden (Table 3).
Secondary prevention
AF worsens quality of life and can cause a statistically significant increase in the risk of cardiovascular events (death, heart failure, stroke and sudden cardiac death).11 To prevent complications associated with AF, secondary prevention strategy is discussed in the following sections.
Lifestyle modification
Lifestyle modification in the form of smoking cessation, good quality sleep, alcohol cessation, incorporation of a Mediterranean diet, physical activity in any form and yoga are beneficial in the management of AF.12 Lifestyle intervention not only reduces the incidence of AF, but also induces AF remission and more successful ablation outcomes.12 Even if one may not able to completely reverse AF with lifestyle modification, intervention at the lifestyle level may likely enhance AF treatment efficacy.12
Optimisation of rate control of and normal sinus rhythm
Restoring and maintaining sinus rhythm should be an integral part of AF management. Antiarrhythmic drugs approximately double the rate of sinus rhythm compared with placebo.13–7 The effect of modern rhythm control management using catheter ablation, combination therapy, or early catheter ablation on major cardiovascular events is still under investigation.6,18 Catheter ablation may be considered as a second-line treatment (after failure of, or intolerance to, antiarrhythmic drug therapy) in restoring and maintaining sinus rhythm in patients with symptomatic paroxysmal, persistent and probably long-standing persistent AF.19–22 However, catheter ablation should not be used to prevent cardiovascular outcomes, to withdraw anticoagulant, or to reduce hospitalisations.18 AF catheter ablation has also shown promising results in heart failure with reduced left ventricular ejection fraction in terms of lower mortality rate and reduce hospitalisation for heart failure, especially in patients without prior myocardial infarction.18 However, since ablating AF can be demanding in these patients, selection of patients should be carefully balanced and the procedures should be performed in experienced centres only.
Fast ventricular rate in AF demands rate control on a priority basis. One must look for and treat the precipitating cause (anaemia, alcohol intake, pulmonary embolism, infection, hyperthyroidism, drug use, acute coronary syndrome, valvular heart disease etc). Rapid rate control during AF may be achieved by intravenous diltiazem/verapamil; both of which have rapid onset of action and are effective at high sympathetic tone.23,24 Other agents that may be used for rate control in specific conditions are beta blockers, digoxin (heart failure with AF) and amiodarone (AF with severe left ventricular systolic dysfunction).
Since clinical events, NYHA class, or hospitalisations rates among patients with lenient heart rate control (target of 110 bpm) are as good as strict heart rate control,25 either of the strategies may be used while opting for a rate-control strategy over rhythm-control strategy.
Achievement of adequate anticoagulation
Adequate anticoagulation should be achieved to minimise the risk of thromboembolic events in the setting of AF. The CHA2DS2-VASc score is widely used as a risk stratification tool for the initial decision to start oral anticoagulants in patients with AF. Patients with score of 0 (i.e., without any clinical stroke risk factors) do not need oral-anticoagulant therapy; while patients with CHA2DS2-VASc score of >1 in men, and >2 in women, need to be on oral anticoagulants to prevent ischaemic stroke.26 Bleeding risk must be assessed before starting oral anticoagulants. Notably, many of the risk factors for stroke and bleeding overlap with each other. Aspirin as monotherapy has no benefit for stroke prevention in patients of AF.27 Antiplatelet monotherapy therefore is not recommended for stroke prevention in patients with AF, irrespective of their stroke risk. Dual antiplatelet therapy offers significantly less protection against stroke, thromboembolism, myocardial infarction and vascular deaths when compared to vitamin K antagonists (VKAs; annual risk of 5.6% for aspirin and clopidogrel versus 3.9% with VKA therapy) but at the cost of similar bleeding risk (2.0% versus 1.3% with antiplatelet monotherapy; p=0.001).28 HASBLED, ORBIT and ABC are three bleeding risk scores that have been developed for risk assessment of bleeding in patients on VKAs.29–31 A high bleeding score should not be a reason to defer oral anticoagulants; rather one should identify and treat the underlying risk factors.
Left atrial appendage closure device
Left atrial appendage closure may be considered for patients with contraindication to long-term oral anticoagulants. Left atrial appendage occlusion has been found non-inferior to VKA treatment for the prevention of stroke in AF patients with moderate stroke risk, with a possibility of lower bleeding rates in the patients. Three studies have focused on left atrial appendage closure in patients with contraindications to oral-anticoagulant therapy and have shown improvement in the incidence of ischaemic stroke from expected
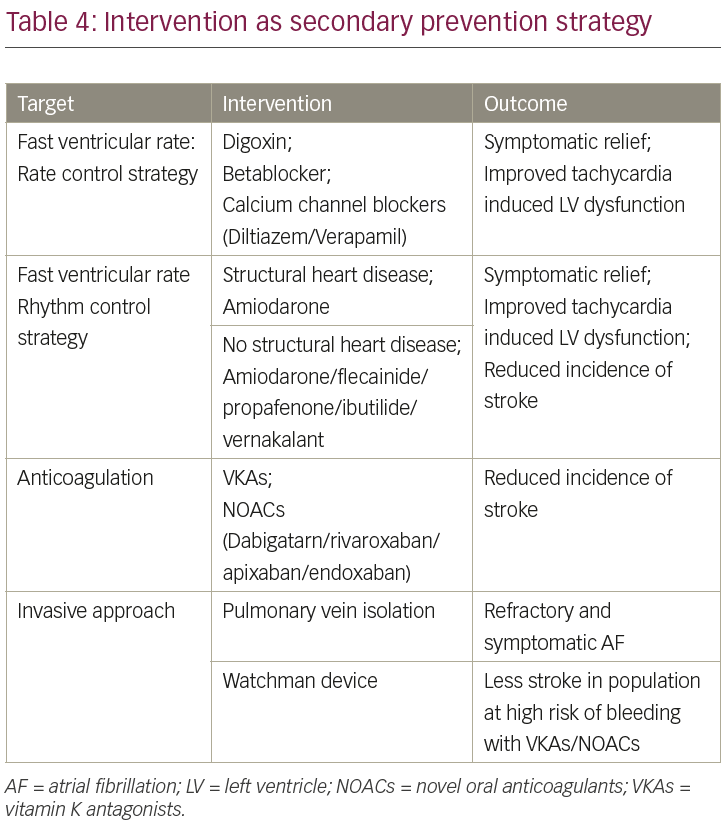
5.6–7.6% (based on CHADS2 score) to 1.7–3.2%.32–4 Surgical exclusion of left atrial appendage did not show a clear benefit of left atrial appendage exclusion for stroke prevention in a subgroup undergoing AF surgery.35 Some of the steps to intervene at secondary level and their outcomes are mentioned in Table 4.
Tertiary prevention
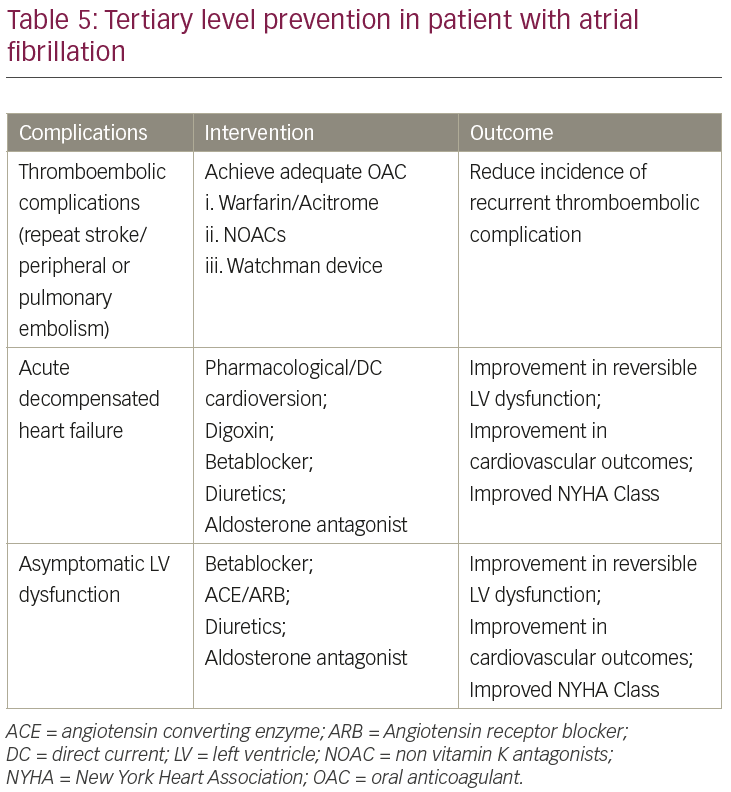
Tertiary prevention addresses the care of patients who have already suffered a stroke/transient ischaemic attack (Table 5). These measures are aimed at the prevention of a second or third stroke and reducing the disability through patient rehabilitation. Research shows that patients who suffer recurrent stroke have poorer outcomes than those who suffer a first stroke;36 hence, anticoagulation is the major goal of therapy in patients with AF. The Stroke Prevention Patient Outcomes Research Team (PORT) study found that 57% of patients with a first stroke survived 24 months after their stroke, compared with 48% of those who had a recurrent stroke.37 Patients with AF with a mechanical prosthetic valve, moderate to severe mitral stenosis, or those with advanced kidney disease (CrCl <30 mL/min), should be treated exclusively with VKAs.
Multiple randomised controlled trials have demonstrated non-inferiority/superiority of novel oral anticoagulants (NOACs; dabigatran, rivaroxaban, apixaban and edoxaban) in non-valvular AF as compared to VKAs.38–42 Also, since each anticoagulant carries risks for haemorrhagic complications, it is useful to risk-stratify patients with AF to identify appropriate candidates for anticoagulation.
Quaternary prevention
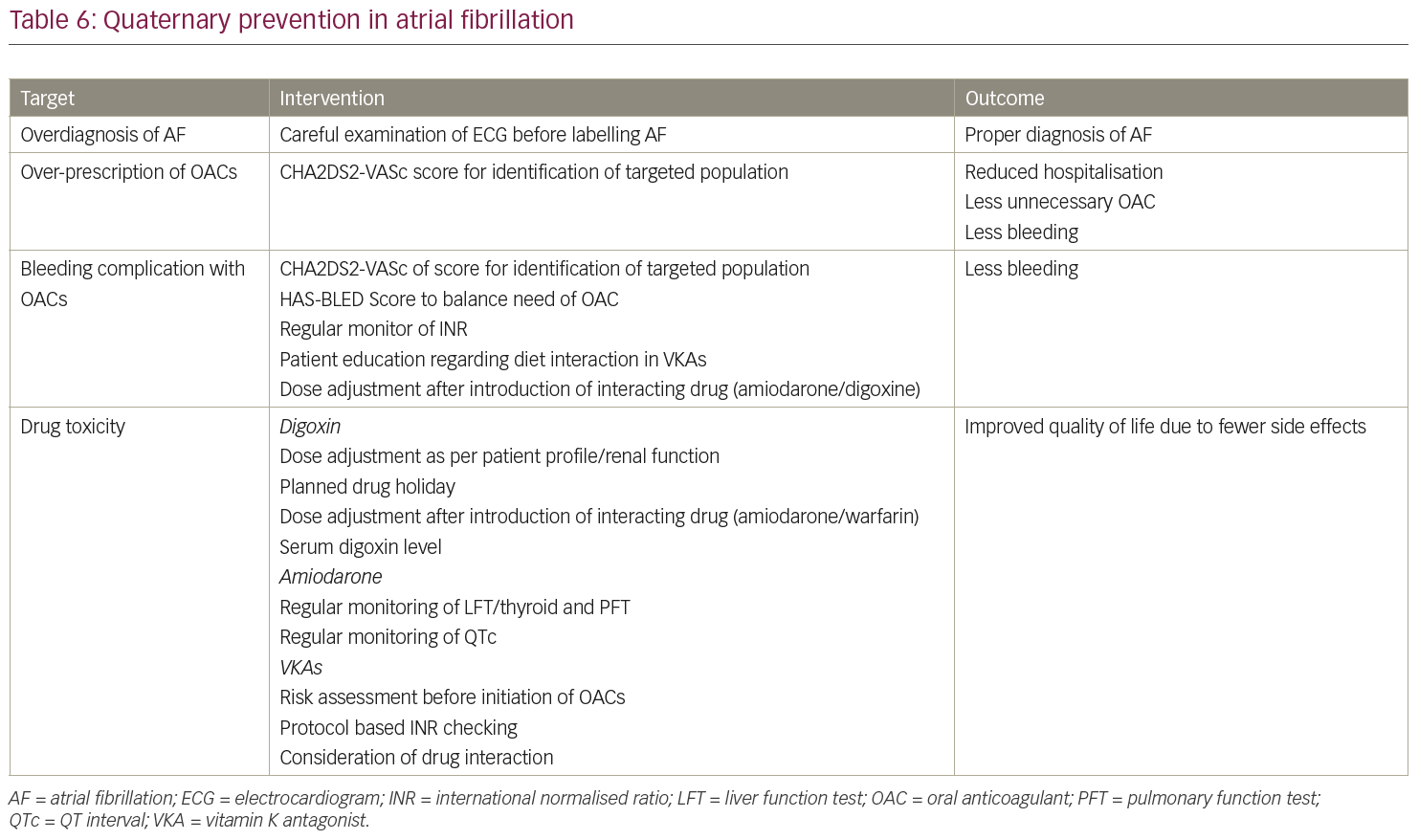
Quaternary prevention is an emerging concept that cautions against overdiagnosis and overtreatment of the disease (Table 6). A few of the considerations relevant to quaternary prevention are highlighted below as quaternary prevention of AF. Careful evaluation and interpretation of the underlying rhythm is of utmost importance. Treatment must be planned after considering the frequency and type of AF, underlying aetiology and associated risk factors. Over-prescription of oral anticoagulants must be avoided. One must
balance between thrombotic risk associated with AF and bleeding risk due to oral anticoagulants.
Overdiagnosis of atrial fibrillation
Many tachyarrhythmias may mimic AF. Attention should be given to regularity and rate. Atrial premature complexes, junctional ectopic tachycardias, ventricular premature complexes and sinus arrhythmia are the common mimickers of AF. Careful analysis of the rhythm and the presence of well-formed P wave may help one to rule out the possibility of AF.
Overtreatment of atrial fibrillation
Patients with AF are more likely to suffer stroke compared to those without AF,2–3 making oral anticoagulants (VKAs or NOACs) mandatory in patients with AF whenever the risk of stroke is high. However, one must balance the benefit of oral anticoagulants with risk of bleeding related to this class of therapy. CHA2DS2-VASc and HASBLED scores are available tools to justify initiation of oral anticoagulation. VKA treatment should further be monitored regularly by international normalised ratio (INR), keeping it in range of 2.0–3.0. The spectrum of overtreatment with various classes of therapy varies from gastrointestinal symptoms (nausea, vomiting or abdominal pain), thyroid dysfunction, abnormal pulmonary function test or bradycardia-induced syncope. Careful follow-up with intermittent treatment holidays may prevent such complications. Intervention at quaternary level related to AF management has been highlighted in Table 6.
Quinary prevention
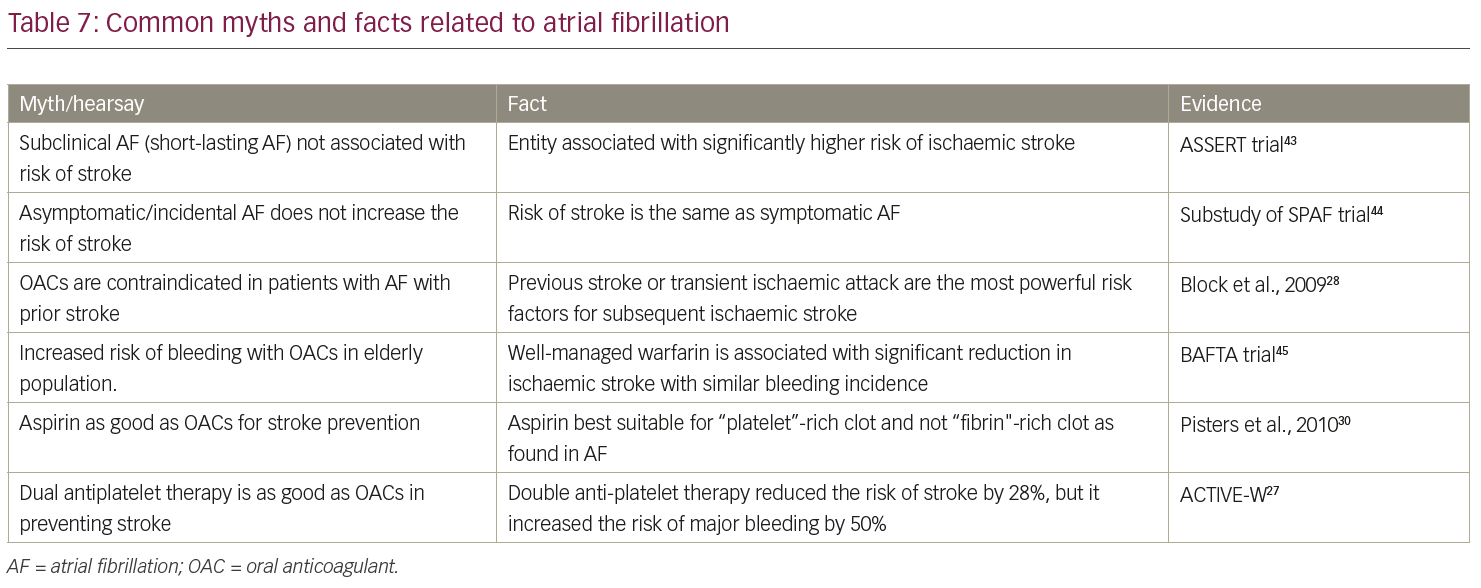
Quinary prevention deals with popular myths related to the concerned disease (Table 7).27,28,30,43–5 Quinary prevention is a new concept which has gained traction with the development of information technology and social media. A few examples are:
- asymptomatic/incidental AF does not increase the risk of stroke;
- oral anticoagulants are contraindicated in patients with AF with prior stroke; and
- there is an increased risk of bleeding with oral anticoagulants in elderly populations.
Summary
AF is a preventable disease and so are its complications. This review provides advice regarding the various methods for the prevention of AF and its related complications. The format described here is easy to understand and apply; it also enhances the appeal of preventive measures and underscores the need to integrate them in routine public health programmes, medical and cardiology practice.